Food Allergy in Adults and Children: Symptoms, Diagnosis and Diet
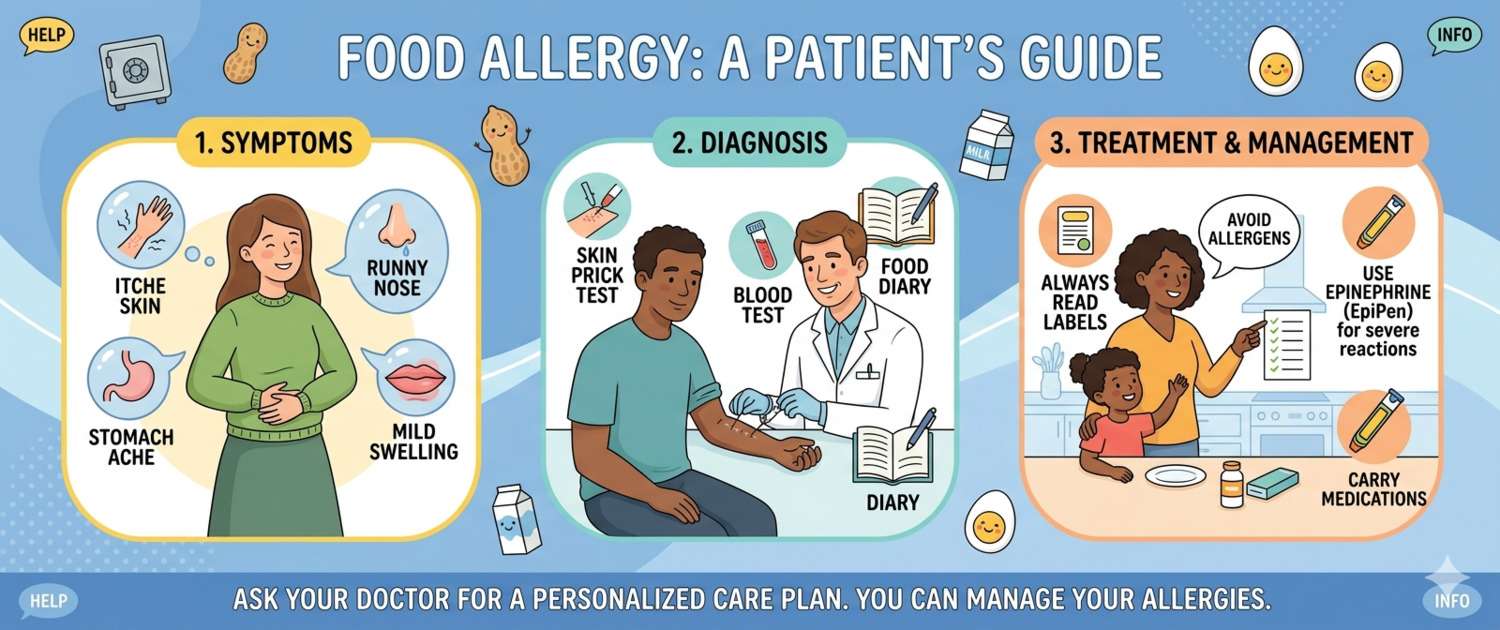
Reactions to food are among the most common reasons for visiting an allergist. But not every unpleasant food reaction is an allergy: most are food intolerances, with a fundamentally different mechanism. Let's clarify what true food allergy is, how it differs from intolerance, which foods most commonly cause it, and how to get an accurate diagnosis.
Food Allergy vs Food Intolerance: A Critical Distinction
Food allergy is an immune reaction: the immune system mistakenly identifies a food protein as a threat and produces IgE antibodies. On repeat exposure, IgE triggers histamine release and symptoms develop. The reaction can be acute and severe — up to anaphylaxis.
Food intolerance has nothing to do with the immune system. Examples: lactase deficiency (missing enzyme for milk sugar digestion), gluten intolerance/celiac disease (autoimmune but not IgE-mediated), reactions to histamine or tyramine in foods. Intolerance causes discomfort but never anaphylaxis.
The distinction is critical: treatment and restrictions differ completely between allergy and intolerance.
Top Eight Food Allergens: From Milk and Peanut Allergy to Shellfish
Eight food groups account for more than 90% of all food allergies:
| Allergen | Notes |
|---|---|
| Cow's milk | Leading cause in children under 3; most outgrow it by school age |
| Hen's eggs | Second most common allergen in children; usually to the white, not yolk |
| Peanuts | Among the most common in adults; high anaphylaxis risk |
| Tree nuts | Cashews, hazelnuts, walnuts, almonds — cross-reactions common |
| Fish | More common in adults; often persists lifelong |
| Shellfish | Shrimp, crab, lobster; often persists in adults |
| Wheat | Wheat allergy ≠ celiac disease — different mechanisms |
| Soy | Common in children with milk allergy |
Food Allergy Symptoms in Adults and Children
Symptoms appear within minutes to 2 hours after eating the trigger food.
Skin: urticaria (hives with itching); angioedema (swelling of lips, tongue, eyelids); skin flushing.
Gastrointestinal: nausea, vomiting, abdominal pain, diarrhea.
Respiratory: nasal congestion, sneezing, wheezing, cough.
Systemic — anaphylaxis: sudden blood pressure drop, loss of consciousness, laryngeal edema with breathing difficulty — a life-threatening emergency requiring immediate epinephrine.
Severity is unpredictable: a previous mild reaction does not guarantee the next won't be anaphylaxis.
Diagnosis of Food Allergy
The diagnosis cannot be made from symptoms alone or by self-imposed food elimination.
Specific IgE Blood Test
Blood test for specific IgE to suspected foods — can be done at any time, antihistamines don't affect the result. High IgE confirms sensitization, but does not always mean clinical allergy: a person may be sensitized but tolerate the food without symptoms.
A complete blood count indirectly indicates allergy: eosinophils are elevated in active allergic processes.
Skin Prick Tests
Performed by an allergist outside of flares, at least 2–4 weeks after stopping antihistamines. Results in 15–20 minutes. Correlate well with clinical allergy.
Oral Food Challenge (Double-Blind, Placebo-Controlled)
The gold standard — but performed only in an allergy clinic due to the risk of severe reaction. The patient receives the suspected food in gradually increasing doses under observation.
Elimination Diet with Food Diary
Eliminating the suspected food for 2–4 weeks followed by controlled reintroduction helps establish the link between symptoms and a specific food.
Treatment of Food Allergy
Strict allergen avoidance — the only reliable prevention. General allergy classification and diagnostic principles are covered in the allergy guide. Reading ingredient labels carefully is essential: milk, eggs, and peanuts hide under many names.
Antihistamines (cetirizine, loratadine) — relieve mild skin and respiratory symptoms.
Epinephrine autoinjector (EpiPen) — mandatory for patients at high anaphylaxis risk. Those with confirmed severe food allergy must carry it at all times.
Oral immunotherapy (OIT) — gradual introduction of increasing allergen doses to reduce sensitivity. Used for peanut, milk, and egg allergy; a peanut OIT product (Palforzia) is approved. Performed only under allergist supervision.
When to Seek Urgent Medical Attention
Call emergency services immediately for: difficulty breathing, wheezing; tongue or throat swelling; sudden drop in blood pressure, loss of consciousness; hives combined with any of the above — this is anaphylaxis.
Scheduled allergist visit: repeated reactions to the same food; unexplained reaction with skin symptoms; confirmation of diagnosis and anaphylaxis management education.
Summary
Food allergy requires accurate diagnosis — not self-imposed elimination of entire food groups. Unnecessarily broad exclusion diets can lead to nutritional deficiencies, especially in children. Only an allergist using specific IgE testing and skin prick tests can confirm the diagnosis and create a rational dietary plan.
This article is for informational purposes only. Interpretation of test results and treatment decisions are the responsibility of a physician.
Frequently Asked Questions
Food allergy is an immune IgE reaction: fast-onset, can be severe up to anaphylaxis, even with tiny amounts. Food intolerance is a non-immune mechanism (enzyme deficiency, direct irritation): usually dose-dependent, symptoms only with larger amounts, and never causes anaphylaxis. Lactose intolerance is an intolerance, not an allergy.
Main test: specific IgE to suspected foods (blood, can be done any time). Additional: skin prick tests (outside of flares). Gold standard: oral food challenge under allergist supervision. A complete blood count with eosinophils is an indirect marker of allergic inflammation.
Depends on the allergen and age. Milk and egg allergy resolves in 50–80% of children by school age. Peanut, tree nut, fish, and shellfish allergy more often persists lifelong — only 20–25% of patients with peanut allergy experience spontaneous remission.
For mild symptoms (hives only): take an antihistamine (cetirizine). If symptoms escalate — breathing difficulty, throat swelling, or blood pressure drop — immediately use the epinephrine autoinjector (if available) and call emergency services. After anaphylaxis: mandatory observation in hospital for at least 4–6 hours.
With IgE-mediated food allergy — no: even trace amounts can trigger a severe reaction. This is fundamentally different from food intolerance, where small amounts are often tolerated. Anaphylaxis from peanut traces in oil or the smell of cooking has been reported. If you have atopic dermatitis, the risk of food sensitisation is further increased.
Upload your lab results photo or PDF
AI explains your results in 30 seconds
Choose fileRate the service
Your feedback helps us improve the service