Anti-TG Antibodies: Normal Levels and What Elevated Results Mean
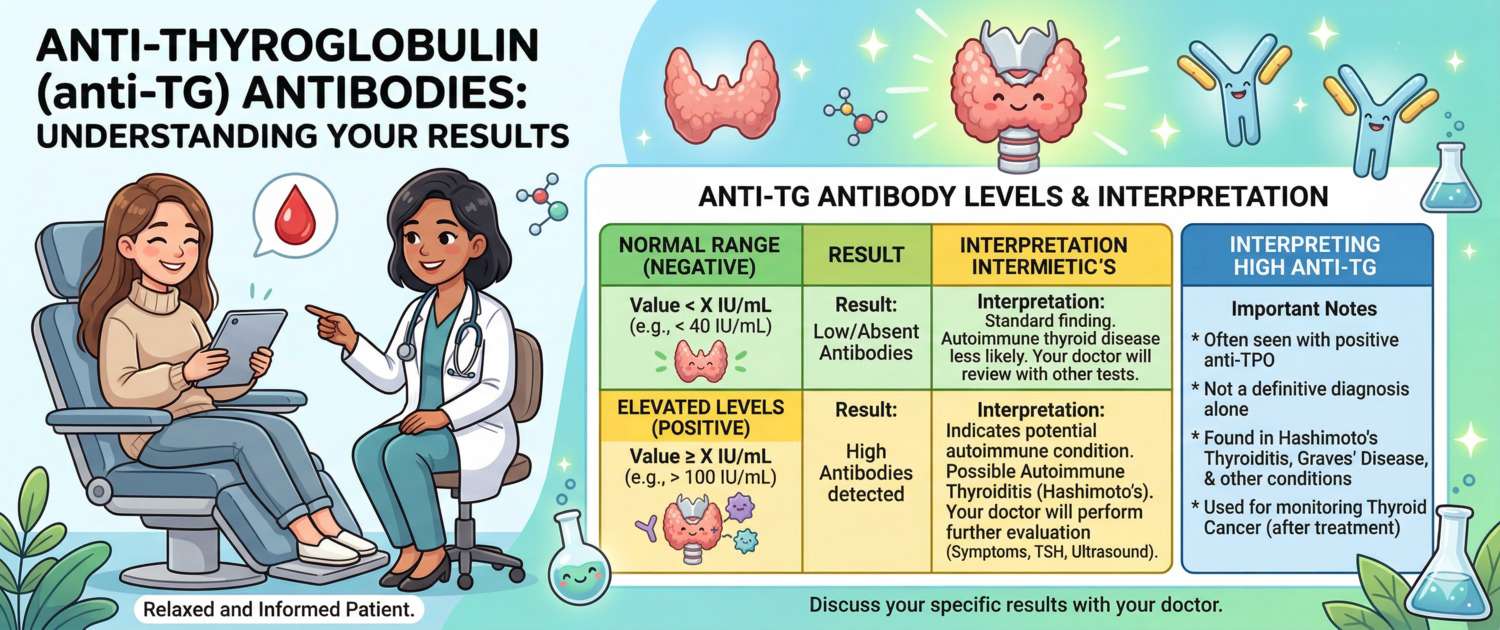
Anti-thyroglobulin antibodies (anti-TG) are the second major marker of autoimmune thyroid disease. They complement anti-TPO in diagnosing Hashimoto's thyroiditis — and after total thyroidectomy for cancer, anti-TG takes on a different, critical role: it interferes with measuring thyroglobulin, the primary tumour recurrence marker, making its own trend the key monitoring tool instead.
What Is Thyroglobulin and Why Does the Body Produce Antibodies Against It
Thyroglobulin is a large protein produced exclusively by thyroid cells. It acts as a storage molecule and precursor for thyroid hormones T3 and T4, which are cleaved from it by enzymes before entering the bloodstream.
Under normal conditions, thyroglobulin rarely leaves the thyroid, so the immune system leaves it alone. In autoimmune inflammation, this barrier breaks down: thyroglobulin enters circulation, the immune system recognises it as foreign, and produces anti-TG antibodies. These antibodies do not destroy tissue as aggressively as anti-TPO, but they are a reliable indicator of autoimmune activity.
Anti-TG is often ordered together with anti-TPO, TSH and calcitonin as part of a comprehensive thyroid panel.
Anti-TG Normal Range
Reference values depend on the assay method, so the only reliable benchmark is your laboratory's own reference range. Most modern immunochemiluminescent assays use:
| Category | Normal Range (IU/mL) |
|---|---|
| Adults (men and women) | < 115 IU/mL |
| After thyroidectomy (monitoring) | target: undetectable |
After total thyroidectomy for cancer, the absolute value matters less than the trend: a consistent rise in anti-TG alongside undetectable thyroglobulin is a warning sign.
Causes of Elevated Anti-TG Antibodies
Hashimoto's thyroiditis — the most common cause. Anti-TG is elevated in 60–80% of patients. In Hashimoto's thyroiditis it typically appears alongside elevated anti-TPO, though the ratio between them varies.
Graves' disease — autoimmune hyperthyroidism. Anti-TG is elevated in 50–70% of patients, but TSH receptor antibodies (TRAb) are the primary diagnostic marker here.
Differentiated thyroid cancer — papillary and follicular types. Here elevation signals that anti-TG is interfering with thyroglobulin measurement, which is itself considered an unfavourable sign for post-surgical monitoring.
Other autoimmune conditions — lupus, rheumatoid arthritis, pernicious anaemia. Mild anti-TG elevation can occur as a non-specific autoimmune reaction.
Isolated mild elevation in anti-TG with normal anti-TPO and TSH is found in 3–5% of healthy individuals and requires observation without immediate treatment.
Anti-TG in Thyroid Cancer: A Recurrence Marker
After total thyroidectomy for cancer, thyroglobulin should become undetectable — the organ producing it is gone. Rising thyroglobulin signals recurrence or metastasis.
The problem: anti-TG binds to thyroglobulin and interferes with its accurate measurement, artificially lowering reported values. When anti-TG is present, thyroglobulin becomes unreliable as a tumour marker. In such patients, the trend in anti-TG itself becomes the primary monitoring tool — a falling trend is reassuring, a rising trend warrants thorough investigation.
Thyroid cancer has an excellent prognosis when detected and treated early, which makes monitoring precision critically important.
Anti-TG vs Anti-TPO: What Is the Difference
Both tests detect autoimmune thyroid involvement, but with different strengths:
| Marker | Sensitivity in Hashimoto's | Primary use |
|---|---|---|
| Anti-TPO | ~95% | Diagnosing autoimmune thyroiditis |
| Anti-TG | ~60–80% | Post-thyroidectomy monitoring |
In practice, both are ordered together. If anti-TPO is normal but anti-TG is elevated, an autoimmune process is still present and warrants attention.
How to Prepare for the Anti-TG Test
Blood is drawn from a vein after an 8-hour fast. No special preparation is required, but note:
- thyroid hormone medication is taken on your usual schedule unless your doctor advises otherwise
- avoid iodine-containing supplements and contrast agents 2–3 days before
- result is not affected by menstrual cycle phase
Anti-TG should never be interpreted in isolation — it is always evaluated alongside anti-TPO, TSH and clinical findings. After thyroid surgery, add thyroglobulin to the panel.
When to See a Doctor
See an endocrinologist if anti-TG is elevated together with abnormal TSH or symptoms such as fatigue, weight changes, swelling, or palpitations. After thyroidectomy, any rising anti-TG trend — especially with undetectable thyroglobulin — requires investigation to rule out recurrence.
This information is for educational purposes only. Diagnosis and treatment are provided exclusively by a qualified physician.
Frequently Asked Questions
Elevated anti-TG points to an autoimmune thyroid process. The most common causes are Hashimoto's thyroiditis and Graves' disease. In patients after thyroid surgery, rising anti-TG is a reason to rule out cancer recurrence. A confirmed autoimmune process warrants monitoring for hypothyroidism.
Most laboratories set the upper limit at 115 IU/mL. After thyroidectomy, the target is an undetectable level. The reference range depends on the specific laboratory's method — always check your own report.
Anti-TPO targets the hormone synthesis enzyme and is positive in 95% of Hashimoto's cases — it is the primary diagnostic marker and more sensitive overall. Anti-TG targets the hormone precursor protein and is especially valuable for post-surgical cancer monitoring. Both are typically ordered together.
After thyroidectomy, anti-TG interferes with thyroglobulin measurement — the key cancer recurrence marker. When anti-TG is present, thyroglobulin values are underestimated and become unreliable. In this situation, the trend in anti-TG itself guides clinical decisions: falling is good, rising needs investigation.
There is no specific treatment to reduce anti-TG. Management depends on context: in Hashimoto's thyroiditis — TSH monitoring and thyroid hormone replacement if hypothyroidism develops. After thyroid cancer surgery — an individualised monitoring programme with an oncologist and endocrinologist.
Blood is drawn after an 8-hour fast. Avoid iodine-containing supplements 2–3 days before. Thyroid hormone medication is taken on your usual schedule. Time of day and menstrual cycle phase do not affect the result. A calcitonin test may also be ordered for comprehensive assessment.
Upload your lab results photo or PDF
AI explains your results in 30 seconds
Choose fileRate the service
Your feedback helps us improve the service