Phosphorus in Blood: Normal Levels, Causes and Treatment
Phosphorus rarely gets much attention — it's not part of a standard blood panel, and most people only think about it when something comes back abnormal. Yet this mineral is involved in the function of every cell in the body: without it, ATP synthesis, DNA replication, and bone maintenance are impossible. Let's break down what blood phosphorus levels reveal, why they deviate from normal, and which conditions lie behind those deviations.
What Phosphorus Does and Why the Body Needs It
Phosphorus is the second most abundant mineral in the human body after calcium. About 85% of the body's stores are concentrated in bones and teeth; the remaining 15% are distributed across soft tissues, cell membranes, and blood.
Its roles are extensive. Phosphorus is a core component of ATP — the cell's primary energy currency — meaning cells literally cannot function without it. Phospholipids containing phosphorus form the bilayer of every cell membrane. Phosphate also participates in regulating blood acid-base balance and in activating enzymes and hormones.
In laboratory testing, inorganic phosphorus is measured — the fraction circulating freely in blood plasma. It represents a small but clinically meaningful portion of total body stores.
The key regulatory pair is phosphorus and calcium: their blood levels are tightly interdependent. When one rises, the other often falls, and vice versa. The conductor of this balance is parathyroid hormone.
Normal Blood Phosphorus Levels by Age
Reference values vary by age: children have higher phosphorus levels than adults — a normal reflection of active bone growth.
| Age | Normal range (mmol/L) |
|---|---|
| Newborns | 1.78–2.65 |
| Children under 2 years | 1.45–2.16 |
| Children 2–12 years | 1.45–1.78 |
| Adolescents 12–18 years | 0.81–1.62 |
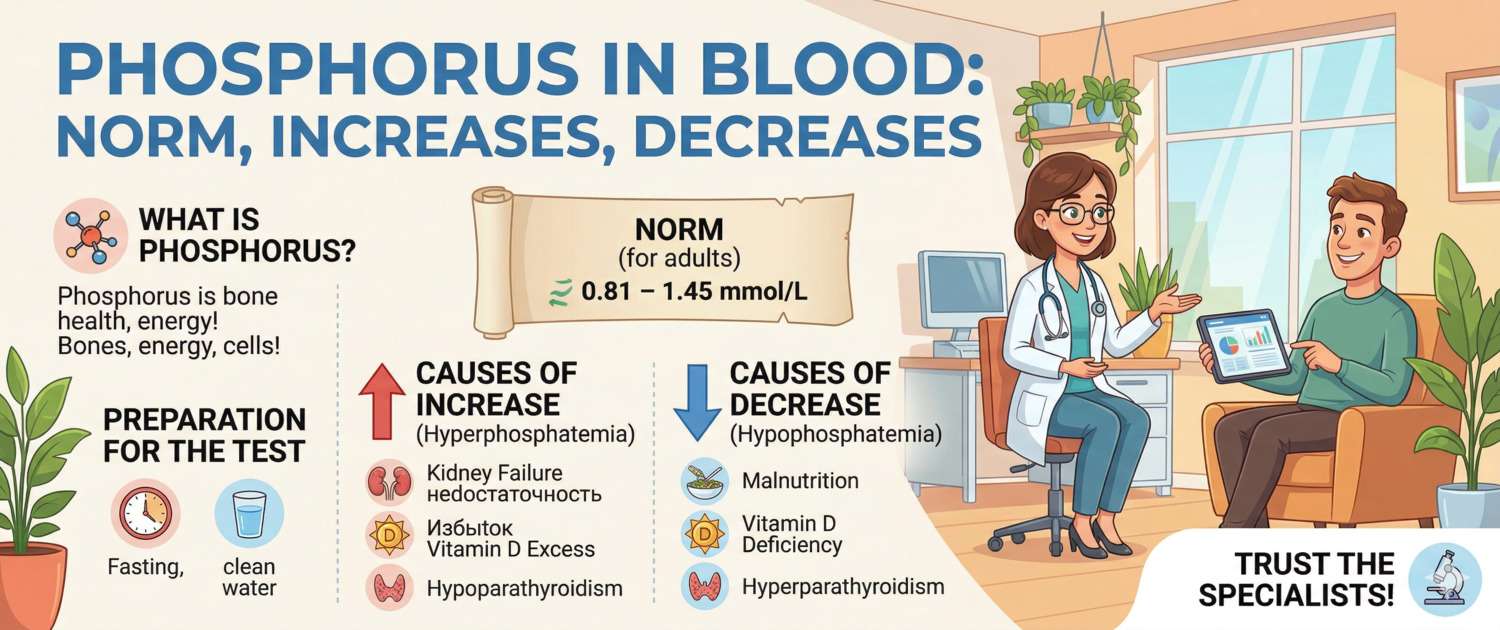
| Adults 18–60 years | 0.87–1.45 |
| Adults over 60 years | 0.74–1.20 |
In postmenopausal women, the lower reference limit is slightly reduced due to changes in phosphocalcic metabolism. During pregnancy, phosphorus levels may decrease modestly — this is physiological.
Important: reference ranges can differ slightly between laboratories and analytical methods. Always compare results against the ranges printed on your specific lab report.
How to Prepare for a Phosphorus Blood Test
Blood phosphorus levels fluctuate throughout the day and are sensitive to food intake. For a reliable result:
- Fast for at least 8 hours before the draw — eating transiently lowers phosphorus
- Avoid phosphorus-rich foods the evening before: dairy, fish, nuts, legumes
- Skip intense exercise before the test — it causes a transient drop in phosphorus
- Inform your doctor about antacids, vitamin D supplements, and diuretics — all of these significantly affect phosphorus levels
- Avoid prolonged storage of the blood sample — phosphorus leaks from red blood cells during hemolysis, causing falsely elevated readings
Phosphorus is almost always ordered together with calcium, parathyroid hormone, and kidney function markers — isolated phosphorus interpretation provides very limited information.
Causes of High Phosphorus in Blood (Hyperphosphatemia)
Hyperphosphatemia — phosphorus above 1.45 mmol/L in adults — is most commonly caused by impaired renal excretion.
Chronic kidney disease is the leading cause. As kidney function declines, the ability to excrete phosphorus diminishes. In chronic kidney disease, phosphorus rises in parallel with worsening filtration, aggravating vascular calcification and bone disease. This is why kidney function testing is always part of the workup when phosphorus is abnormal.
Hypoparathyroidism — insufficient parathyroid hormone secretion. PTH normally reduces phosphorus reabsorption in the kidneys; when PTH is deficient, phosphorus is retained and calcium falls.
Vitamin D excess — enhances intestinal absorption of both phosphorus and calcium. Hyperphosphatemia from vitamin D toxicity often coexists with hypercalcemia.
Acute acidosis and tissue breakdown — in rhabdomyolysis, massive hemolysis, or tumor lysis syndrome, phosphorus floods out of cells into the bloodstream, causing acute hyperphosphatemia.
Diet and medications — excessive phosphate-containing foods and some sodium phosphate laxatives can produce moderate elevation.
Causes of Low Phosphorus in Blood (Hypophosphatemia)
Hypophosphatemia — phosphorus below 0.87 mmol/L — is less common but can be severe and symptomatic.
Primary hyperparathyroidism — excess PTH secretion drives urinary phosphorus excretion. Calcium is elevated in parallel — a classic reciprocal pattern.
Vitamin D deficiency — impairs intestinal phosphorus absorption. Rickets in children and osteomalacia in adults are the classic manifestations of chronic hypophosphatemia combined with vitamin D deficiency.
Refeeding syndrome — occurs during aggressive nutritional support after prolonged starvation. Insulin released in response to carbohydrates drives phosphorus into cells, causing a sharp plasma drop — a life-threatening emergency in intensive care settings.
Chronic alcohol use disorder — impairs phosphorus absorption and increases urinary losses. Severe hypophosphatemia in this population can cause muscle weakness and neurological damage.
Aluminum- and magnesium-based antacids — bind phosphorus in the gut, reducing absorption. Prolonged unsupervised use is a real-world cause of hypophosphatemia.
Phosphorus, Calcium, and Parathyroid Hormone: How the System Works
Understanding phosphorus deviations without considering calcium and PTH is nearly impossible — they form a single regulatory system.
The logic: when blood calcium falls, the parathyroid glands release parathyroid hormone. PTH simultaneously mobilizes calcium from bone, enhances intestinal calcium absorption (by activating vitamin D), and drives phosphorus excretion in the kidneys. The net result: calcium rises, phosphorus falls.
This explains the classic picture of primary hyperparathyroidism: high calcium + low phosphorus + high PTH. And the reverse pattern in hypoparathyroidism: low calcium + high phosphorus + low PTH.
This is why phosphorus is almost never interpreted in isolation — it is always evaluated alongside calcium, PTH, and kidney function.
Symptoms and When to See a Doctor
Hyperphosphatemia is often asymptomatic at moderate elevations. With significant and prolonged elevation, soft tissue and vascular calcifications develop, along with skin itching, bone pain, and joint discomfort.
Hypophosphatemia is more overtly symptomatic: muscle weakness, bone pain, fatigue, impaired concentration and memory. Severe hypophosphatemia (< 0.32 mmol/L) can cause seizures, respiratory failure from weakened breathing muscles, and hemolytic anemia.
A scheduled visit to a doctor is warranted for any phosphorus deviation found on a blood test. Seek urgent care if you experience:
- Severe muscle weakness combined with bone pain
- Tetany, cramps, or muscle spasms — possible concurrent severe hypocalcemia
- Altered consciousness in a patient with known kidney disease or diabetes
- Sudden phosphorus drop after reintroduction of feeding following starvation
This article is for informational purposes only and does not replace professional medical advice. Consult a general practitioner, endocrinologist, or nephrologist if your blood phosphorus is outside the normal range.
Frequently Asked Questions
The kidneys are the primary route for phosphorus excretion. As kidney function declines, their capacity to excrete phosphorus falls and it accumulates in the blood. Hyperphosphatemia accelerates progression of kidney disease, drives vascular calcification, and worsens bone disease. Assessing the full picture of kidney mineral handling is best done with an electrolyte panel alongside other kidney function markers.
They share a reciprocal relationship: rising phosphorus often accompanies falling calcium, and vice versa. Parathyroid hormone regulates both simultaneously — it raises calcium and lowers phosphorus by increasing renal excretion. This is why any phosphorus abnormality is always evaluated together with calcium and PTH. Creatinine is typically added to assess kidney filtration function, which directly governs phosphorus metabolism.
Mild hypophosphatemia is often asymptomatic and found incidentally. At moderate levels, muscle weakness, easy fatigue, dull bone pain, and difficulty concentrating appear. Severe hypophosphatemia (below 0.32 mmol/L) can cause seizures, confusion, and respiratory compromise due to weakness of the breathing muscles — a medical emergency requiring immediate treatment.
Yes, though less dramatically than for most other electrolytes — the kidneys regulate phosphorus across a wide range of dietary intake. That said, chronically excessive phosphate consumption (carbonated drinks, processed foods, fast food) combined with reduced kidney function can produce sustained hyperphosphatemia. Prolonged use of aluminum-based antacids reduces intestinal phosphorus absorption and can lead to hypophosphatemia over time.
Yes. The test must be done fasting — at least 8 hours without food, as eating transiently lowers phosphorus. Limit dairy, fish, and nuts the evening before. Tell your doctor about antacids, vitamin D supplements, diuretics, and laxatives — all of these significantly influence results. The test is almost always ordered together with calcium and PTH for meaningful clinical interpretation.
Most commonly: kidney disease, parathyroid gland disorders (hyper- and hypoparathyroidism), and bone metabolism disorders. Also: rickets and osteomalacia, osteoporosis, monitoring of vitamin D therapy, unexplained muscle weakness, and bone pain. In critical care, phosphorus monitoring is mandatory when refeeding syndrome is a risk.
Upload your lab results photo or PDF
AI explains your results in 30 seconds
Choose fileRate the service
Your feedback helps us improve the service