Chronic Kidney Disease: Stages, Symptoms and Treatment
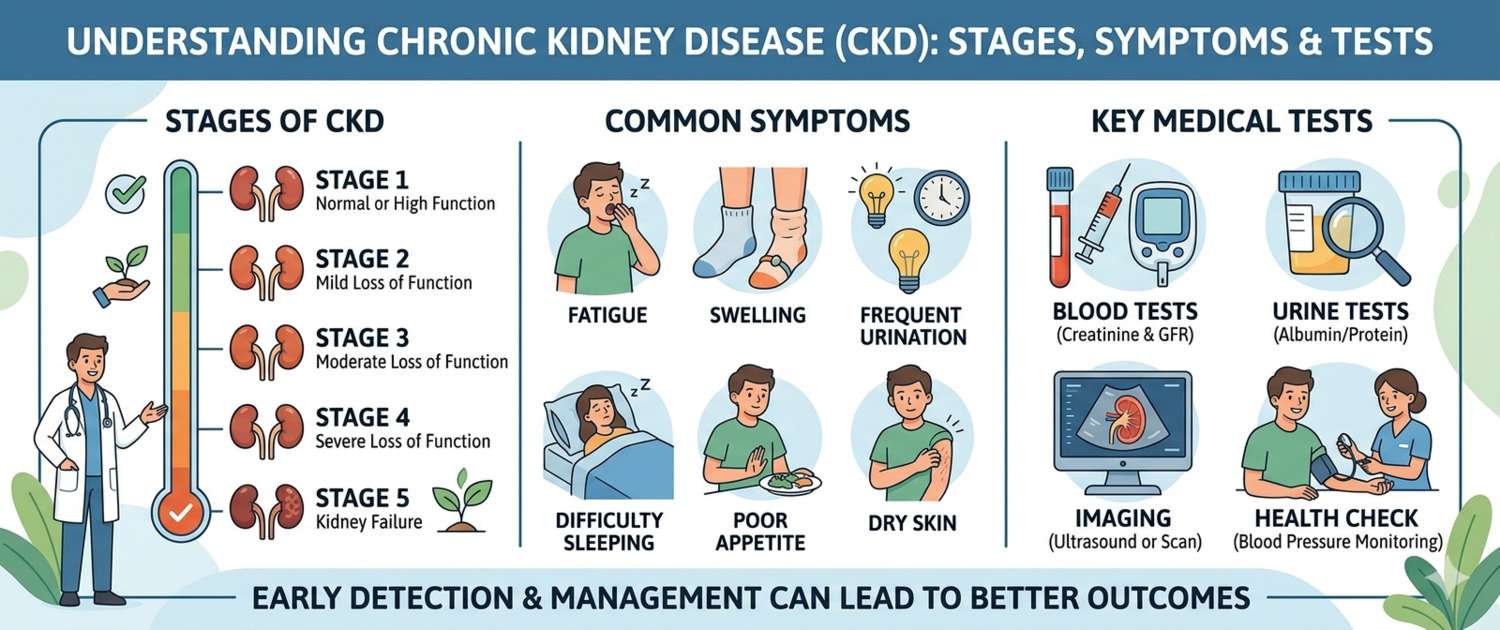
Kidneys do not hurt — until 70–80% of their function has been lost. This is precisely what makes chronic kidney disease (CKD) so dangerous: it develops over years, progresses without symptoms, and is frequently discovered incidentally — on a routine blood or urine test. This article explains what CKD is, how it is diagnosed by stage, which tests are needed, how to slow its progression, and when urgent nephrology consultation is required.
What Is Chronic Kidney Disease and How Is It Defined
Chronic kidney disease is a sustained reduction in kidney function or the presence of markers of kidney damage for three or more months. The three-month criterion is fundamental: a single low GFR or proteinuria result is not yet CKD — the changes must be persistent.
Two key diagnostic markers:
GFR (glomerular filtration rate) — the volume of blood the kidneys filter per minute. Calculated from blood creatinine using the CKD-EPI formula, adjusted for age, sex, and race. Normal is above 90 mL/min/1.73 m².
Albuminuria / proteinuria — the presence of protein in urine. Healthy kidneys do not allow protein through. Persistent proteinuria is one of the earliest and most sensitive markers of glomerular filter damage.
CKD is diagnosed when at least one of these markers is present over three months. Importantly, a normal GFR does not exclude CKD — if persistent proteinuria or structural kidney changes (on ultrasound) are present, the diagnosis is valid.
CKD Stages: GFR and Albuminuria Classification
The international KDIGO classification divides CKD into five GFR stages and three albuminuria categories — their combination determines the risk of progression and cardiovascular complications.
| Stage | GFR (mL/min/1.73 m²) | Description |
|---|---|---|
| G1 | ≥ 90 | Normal or high GFR + damage marker |
| G2 | 60–89 | Mildly reduced + damage marker |
| G3a | 45–59 | Mildly to moderately reduced |
| G3b | 30–44 | Moderately to severely reduced |
| G4 | 15–29 | Severely reduced |
| G5 | < 15 | Kidney failure (end-stage) |
Albuminuria categories: A1 — normal or mildly increased (< 30 mg/g), A2 — moderately increased (30–300 mg/g, microalbuminuria), A3 — severely increased (> 300 mg/g, macroalbuminuria).
The combination of stage and category creates a risk colour map: green — low, yellow — moderate, orange — high, red — very high. A patient classified G3b A3 faces very high risk of progression and cardiovascular events.
Causes of Chronic Kidney Disease
Any chronic condition that damages kidney tissue can lead to CKD. Two causes dominate by a wide margin:
Type 2 diabetes — the most common cause of CKD worldwide. Diabetic nephropathy develops in 30–40% of patients with long-standing diabetes. Chronically elevated glucose damages the glomerular endothelium and basement membrane — first microalbuminuria appears, then proteinuria, then GFR declines. In diabetes, testing the albumin-to-creatinine ratio in urine annually is essential — it allows nephropathy to be caught at a stage when it is still reversible.
Hypertension — the second most common cause. Chronically elevated blood pressure damages the afferent arterioles of the glomeruli, increases intraglomerular pressure, and leads to nephron loss. Keeping blood pressure below 130/80 mmHg is one of the most important measures for slowing CKD.
Other causes: chronic glomerulonephritis (autoimmune glomerular disease), chronic pyelonephritis and other interstitial nephritides, polycystic kidney disease (hereditary), systemic diseases (systemic lupus erythematosus, amyloidosis, vasculitis), long-term nephrotoxic drug use (NSAIDs, certain antibiotics, contrast agents), and urolithiasis with chronic obstruction.
Symptoms of CKD: Why They Are Absent for So Long
At stages G1–G3 (GFR above 30), CKD produces virtually no symptoms — there are still enough functioning nephrons to compensate. Symptoms appear gradually as GFR falls.
Early signs (frequently dismissed):
- Nocturia — increased night-time urination (kidneys losing concentrating ability)
- Morning puffiness — particularly periorbital
- Rising blood pressure without another explanation
- Unexplained fatigue
At GFR 15–30 (stage G4):
- Significant ankle and leg oedema
- Anaemia (kidneys reduce erythropoietin production)
- Increasing weakness
- Reduced appetite, nausea
At end-stage (GFR < 15):
- Uraemia — accumulation of toxins the kidneys no longer excrete: nausea, vomiting, skin itching, neurological symptoms, pericarditis
- Severe anaemia
- Hyperkalaemia — life-threatening cardiac arrhythmia risk
- Severe oedema, dyspnoea
Which Tests Are Needed in CKD
CKD monitoring involves regular tracking of several parameter groups. Frequency depends on stage: G1–G2 — annually; G3 — every 6 months; G4–G5 — every 3 months or more frequently.
Kidney function: creatinine with GFR calculation — the primary dynamic marker. Urea — additional azotaemia marker. The kidney function test covers both parameters.
Urinary sediment: general urinalysis and spot urine albumin-to-creatinine ratio — for quantitative proteinuria assessment. Urinalysis also evaluates inflammatory activity.
Electrolytes: potassium — hyperkalaemia risk rises when GFR < 30; sodium — fluid and electrolyte disorders; bicarbonate — metabolic acidosis in CKD.
Bone and mineral metabolism (when GFR < 45): calcium, phosphorus, parathyroid hormone — secondary hyperparathyroidism develops in most patients with CKD stages 3b–5. For more on the PTH–CKD relationship, see the article parathyroid hormone: what this hormone is.
Vitamin D — activation in the kidneys is impaired in CKD; deficiency is universal and requires correction.
Complete blood count — to detect renal anaemia (haemoglobin fall due to erythropoietin deficiency).
Treatment and Slowing CKD Progression
CKD is not curable in the sense that lost nephrons do not regenerate. But progression can be substantially slowed — and in some causes (early diabetic nephropathy) partially reversed.
Blood pressure control — target < 130/80 mmHg in CKD with proteinuria. Preferred agents are ACE inhibitors or ARBs (angiotensin receptor blockers): they not only lower blood pressure but also reduce intraglomerular pressure, decrease proteinuria, and slow progression independently of the antihypertensive effect.
Glucose control in diabetes — target HbA1c < 7–7.5%. SGLT-2 inhibitors (empagliflozin, dapagliflozin) lower glucose and have proven nephroprotective effects.
Proteinuria reduction — the lower the urinary protein, the slower CKD progresses. Target in diabetic nephropathy: albuminuria < 30 mg/g.
CKD diet:
- Protein restriction (0.6–0.8 g/kg/day when GFR < 30) reduces the load on remaining nephrons
- Phosphorus restriction (dairy products, nuts, legumes, carbonated drinks) for hyperphosphataemia
- Potassium restriction (bananas, potatoes, tomatoes, oranges) for hyperkalaemia
- Sodium restriction (< 2 g/day) for blood pressure and oedema control
Renal replacement therapy (RRT) at end-stage CKD (GFR < 10–15): haemodialysis, peritoneal dialysis, or kidney transplantation. Preparation for RRT begins well in advance — when GFR falls below 20.
When to Seek Urgent Nephrology Consultation
A routine nephrology referral is appropriate when GFR first falls below 60, or at any CKD stage with worsening proteinuria.
Urgent consultation is needed for:
- Rapid GFR decline — more than 5 mL/min/1.73 m² per year, or an acute fall over several weeks (acute-on-chronic kidney injury)
- Hyperkalaemia — potassium above 6.0 mmol/L: life-threatening arrhythmia risk
- Severe uncontrolled hypertension in the context of CKD
- Marked oedema with nephrotic-range proteinuria (> 3 g/day)
- Uraemic symptoms — escalating nausea, vomiting, encephalopathy
CKD is a diagnosis that changes a person's lifestyle — but it is not a sentence. Detected at an early stage and managed correctly, many patients maintain stable kidney function for decades. The key is regular monitoring, blood pressure and glucose control, and early nephroprotective therapy.
This article is for informational purposes only and does not replace medical advice. For any suspected kidney disease, consult a nephrologist or general practitioner.
Frequently Asked Questions
CKD stage is determined by two parameters: the glomerular filtration rate (GFR), calculated from blood creatinine using the CKD-EPI formula, and the level of albuminuria in urine. GFR above 90 is stage G1, 60–89 is G2, 45–59 is G3a, 30–44 is G3b, 15–29 is G4, below 15 is G5. Both markers must be confirmed over three or more months — a single low result is not yet a CKD diagnosis.
At early stages (G1–G3), CKD is almost entirely asymptomatic. As it progresses: nocturia (increased night-time urination), morning puffiness, rising blood pressure, and fatigue appear first. With severe GFR reduction (< 30): significant oedema, anaemia, nausea, and reduced appetite. At end-stage: uraemia with skin itching, nausea, neurological symptoms, and potentially life-threatening hyperkalaemia.
The key principles: protein restriction (0.6–0.8 g/kg/day when GFR < 30) to reduce the load on remaining nephrons; phosphorus restriction (dairy, nuts, legumes, carbonated drinks) for hyperphosphataemia; potassium restriction (bananas, potatoes, tomatoes, oranges) for hyperkalaemia; and sodium restriction for blood pressure and oedema control. The specific diet depends on CKD stage and current kidney function test results — it is prescribed by a nephrologist.
It cannot be fully stopped, but it can be substantially slowed. The main tools are: blood pressure control below 130/80 mmHg (ACE inhibitors or ARBs), proteinuria reduction, tight diabetes management (including SGLT-2 inhibitors for diabetic nephropathy), adherence to a kidney-appropriate diet, and avoiding nephrotoxic drugs (NSAIDs). When detected at an early stage, many patients maintain stable kidney function for years.
Frequency depends on stage. At G1–G2 — annually: urinalysis, creatinine with GFR, urine albumin-to-creatinine ratio, blood pressure. At G3 — every 6 months, adding electrolytes and haemoglobin. At G4–G5 — every 3 months or more: the full previous panel plus calcium, phosphorus, parathyroid hormone, and vitamin D. The monitoring schedule is set by the nephrologist.
Yes — this is one of the central aspects of CKD. Patients with CKD have a 10–30 times higher risk of cardiovascular death than of reaching end-stage renal disease. Contributing factors include chronic inflammation, anaemia, dyslipidaemia, hyperphosphataemia with vascular calcification, chronic hypervolaemia, and renin–angiotensin system activation. This is why blood pressure, urinary protein, and cardiovascular risk factor control are mandatory in CKD.
Upload your lab results photo or PDF
AI explains your results in 30 seconds
Choose fileRate the service
Your feedback helps us improve the service