Parathyroid Hormone (PTH): Normal Levels, Causes and Treatment
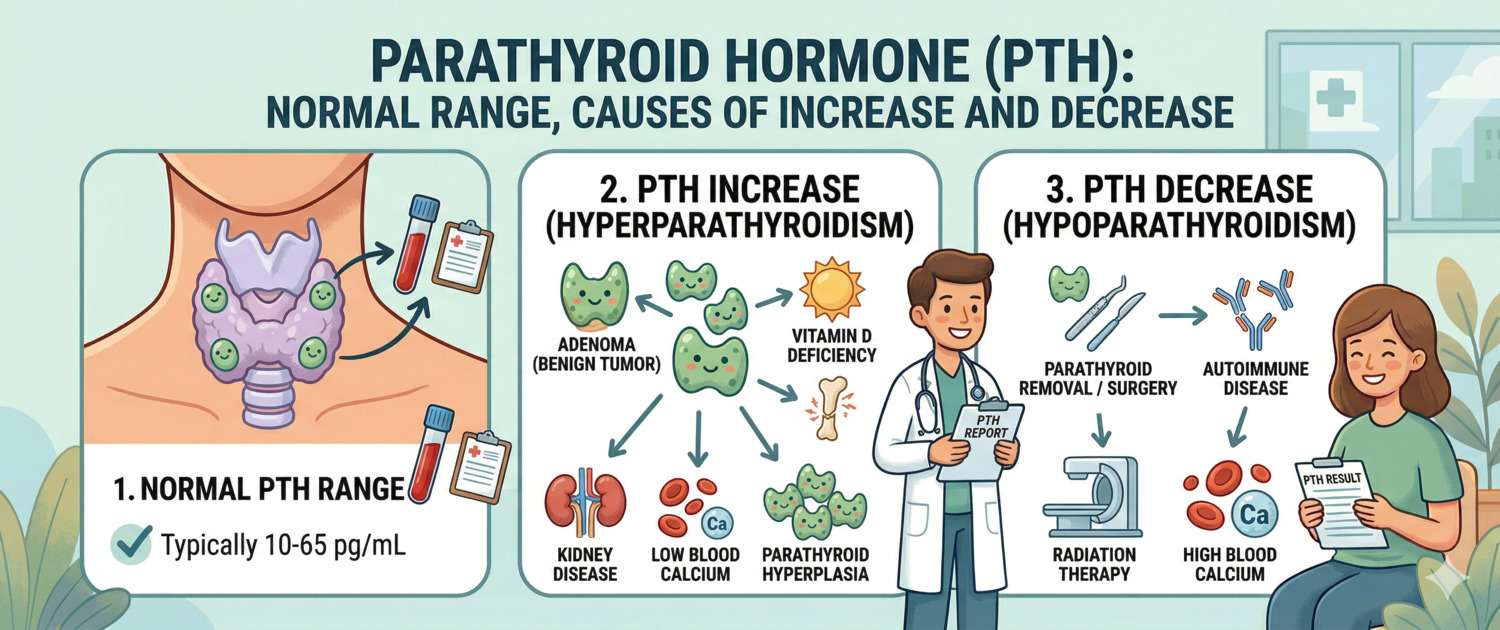
Parathyroid hormone is the invisible conductor of calcium-phosphorus metabolism. Most people never hear of it until an incidentally discovered high or low calcium prompts their doctor to order this test. Yet chronically abnormal PTH silently destroys bone, damages the kidneys, and disrupts neuromuscular function — often for years before a diagnosis is made. Let's break down how this hormone works and why it can never be interpreted without calcium and vitamin D.
What PTH Is and How It Regulates Calcium
Parathyroid hormone (PTH) is a polypeptide of 84 amino acids produced by the parathyroid glands. Humans have four of them — tiny structures the size of a grain of rice, located on the posterior surface of the thyroid gland. Despite their minuscule size, they control one of the most tightly regulated parameters in the body.
PTH is secreted in response to falling calcium in the blood. The response is nearly instantaneous — mediated by the calcium-sensing receptor (CaSR) on parathyroid cell surfaces. The feedback loop: calcium rises → PTH falls; calcium falls → PTH rises immediately.
PTH acts at three target sites:
Bone — the principal calcium reservoir (99% of total body calcium). PTH activates osteoclasts, which resorb bone and release calcium and phosphorus into the blood. Chronic PTH excess leads to osteoporosis and subperiosteal resorption.
Kidneys — PTH acts bidirectionally: it enhances calcium reabsorption (retaining it in blood) while increasing phosphate excretion (excreting phosphorus in urine). It also activates 1α-hydroxylase, converting inactive vitamin D₃ to active calcitriol.
Intestine — indirectly, through calcitriol: active vitamin D dramatically increases intestinal calcium absorption from food.
The net result: PTH raises calcium simultaneously from three sources — bone, kidneys, and intestine. This is precisely why vitamin D deficiency is one of the leading causes of secondary hyperparathyroidism: low vitamin D → poor calcium absorption → chronic hypocalcemia → persistent PTH stimulation.
A complete description of the physiology and clinical forms is available in the article parathyroid hormone: what this hormone is.
Normal Parathyroid Hormone Levels
PTH reference values depend on the analytical method and specific laboratory. Immunoradiometric and chemiluminescent methods are used; the standard is measurement of intact PTH (iPTH, 1–84).
| Group | Normal PTH (pg/mL) | Normal PTH (pmol/L) |
|---|---|---|
| Adults | 15–65 | 1.6–6.9 |
| Children under 10 years | 9–52 | 1.0–5.5 |
| Adolescents 10–17 years | 12–55 | 1.3–5.8 |
| Pregnant (1st trimester) | 10–60 | 1.1–6.4 |
| Pregnant (3rd trimester) | 6–25 | 0.6–2.7 |
| Elderly over 65 years | 15–75 | 1.6–8.0 |
Clinically important nuances:
During pregnancy, PTH physiologically falls in the third trimester: the fetus actively demands calcium, stimulating production of placental PTHrP (parathyroid hormone-related peptide), which partially assumes PTH's regulatory functions.
In chronic kidney disease, the reference range broadens: PTH of 65–300 pg/mL at CKD stage III–IV is considered "target range" by several guidelines — excessively suppressed PTH leads to adynamic bone disease, while very high PTH causes fibrous osteitis.
In older adults, the upper normal limit is slightly higher due to physiologically reduced vitamin D synthesis and intestinal calcium absorption.
How to Prepare for a PTH Blood Test
PTH is an unstable peptide with a plasma half-life of approximately 2–4 minutes. This imposes strict pre-analytical requirements.
- Draw blood strictly fasting — at least 8–12 hours without food: intake of calcium-containing foods transiently suppresses PTH
- Test in the morning between 8:00 and 10:00 AM — PTH follows a diurnal rhythm: peak at night and early morning, nadir at midday; fluctuations reach 40–50%
- Deliver the sample to the lab immediately — PTH degrades at room temperature. Transport on ice, centrifuge within 30 minutes
- For serial monitoring: use the same laboratory and the same method — different platforms produce results differing by 15–30%
- Disclose all calcium supplements, vitamin D, bisphosphonates, diuretics, and lithium
The test is almost always ordered alongside calcium (total and ionized), phosphorus, vitamin D (25-OH), and kidney function — the electrolyte panel is the mandatory backdrop for PTH interpretation.
Causes of High PTH (Hyperparathyroidism)
Hyperparathyroidism is classified as primary, secondary, and tertiary — each with fundamentally different mechanisms and treatment strategies.
Primary hyperparathyroidism — autonomous PTH hypersecretion by the parathyroid glands, independent of calcium levels. In 80–85% of cases: a single parathyroid adenoma. Less commonly: hyperplasia of all four glands (in MEN-1, MEN-2A). Very rarely: parathyroid carcinoma.
Characteristic pattern: high PTH + high calcium. Phosphorus is low (kidneys actively excrete phosphate under excess PTH drive). Vitamin D is often normal.
| Severity | PTH | Calcium | Clinical picture |
|---|---|---|---|
| Mild (asymptomatic) | 65–150 pg/mL | 2.5–2.85 mmol/L | Incidental finding |
| Moderate | 150–300 pg/mL | 2.85–3.0 mmol/L | Osteoporosis, kidney stones |
| Severe | > 300 pg/mL | > 3.0 mmol/L | Hypercalcemic crisis |
Secondary hyperparathyroidism — a physiologically appropriate parathyroid response to chronic hypocalcemia. The glands are functioning correctly; the problem is that calcium is persistently low.
Pattern: high PTH + normal or low calcium.
Main causes:
- Vitamin D deficiency — the most prevalent cause in the general population. Inadequate calcium absorption → chronic hypocalcemia → continuous PTH stimulation
- Chronic kidney disease — impaired active vitamin D synthesis + phosphate retention + acidosis → multiple simultaneous PTH-stimulating mechanisms
- Malabsorption syndromes (celiac disease, inflammatory bowel disease) — impaired calcium and vitamin D absorption
- Pregnancy and lactation — increased calcium demand
Tertiary hyperparathyroidism — develops after prolonged secondary: the parathyroid glands acquire autonomous function and continue hypersecretion even after the primary cause is removed (e.g., after kidney transplantation). Pattern: high PTH + high calcium — superficially resembling primary hyperparathyroidism but in the context of preceding CKD.
Causes of Low PTH (Hypoparathyroidism)
Hypoparathyroidism — PTH below normal — is far less common than hyperparathyroidism but equally significant clinically.
Postoperative hypoparathyroidism — the most common cause. During thyroidectomy or parathyroid surgery, the parathyroid glands may be accidentally removed or devascularized. Onset is within 24–48 hours postoperatively. May be transient (weeks) or permanent.
Autoimmune hypoparathyroidism — isolated or as part of autoimmune polyglandular syndrome type 1 (APS-1, APECED). Antibodies target the calcium-sensing receptor or parathyroid gland tissue.
DiGeorge syndrome — genetic defect in parathyroid gland development (22q11 deletion). Associated with cardiac malformations and immunodeficiency. Diagnosed in childhood.
Hypomagnesemia — severe magnesium deficiency impairs both PTH secretion and its action on target cells. Magnesium is required for calcium-sensing receptor function. Hypoparathyroidism unresponsive to treatment should always prompt magnesium measurement.
Radiation injury — following radiotherapy to the neck region.
Characteristic pattern in hypoparathyroidism: low PTH + low calcium + high phosphorus.
PTH, Calcium, Phosphorus and Vitamin D: Reading the Full Picture
None of these markers can be interpreted in isolation. Only the combination provides a complete clinical picture.
| PTH | Calcium | Phosphorus | Vitamin D | Most likely cause |
|---|---|---|---|---|
| ↑ High | ↑ High | ↓ Low | Normal | Primary hyperparathyroidism |
| ↑ High | Normal/↓ | Normal/↑ | ↓ Low | Secondary HPT — vitamin D deficiency |
| ↑ High | Normal/↓ | ↑ | ↓ Low | Secondary HPT — CKD |
| ↓ Low | ↓ Low | ↑ High | Normal | Hypoparathyroidism |
| ↓ Low | ↑ High | Normal | Normal/↑ | PTH-independent hypercalcemia (malignancy, sarcoidosis) |
| Normal | ↑ High | Normal | Normal | Familial hypocalciuric hypercalcemia (FHH) |
The second-to-last row is a critical clinical trap: malignant tumors secrete PTHrP (parathyroid hormone-related peptide), which is not detected by the standard PTH assay but causes hypercalcemia. Therefore, when calcium is high and PTH is low — an oncological workup is mandatory.
Kidney function is essential context for any PTH abnormality. A rising creatinine points to CKD as the driver of secondary hyperparathyroidism and determines treatment strategy. Albumin is needed to correctly interpret total calcium: in hypoalbuminemia, total calcium is falsely low and the ionized fraction must be evaluated directly.
When PTH Abnormalities Require Medical Attention
PTH is not a screening test. It is ordered when calcium or phosphorus deviations are already present, or when specific clinical indications exist.
Scheduled visit to an endocrinologist when:
- High PTH combined with high calcium — rule out primary hyperparathyroidism; parathyroid scintigraphy or ultrasound is indicated
- High PTH with normal or low calcium — identify secondary causes: vitamin D, kidney function, absorption
- Any PTH deviation after thyroid or parathyroid surgery
- Osteoporosis in a patient under 50 — exclude primary hyperparathyroidism as the underlying cause
Seek urgent care when:
- Calcium > 3.0 mmol/L combined with elevated PTH — risk of hypercalcemic crisis: nausea, vomiting, confusion, polyuria
- Calcium < 1.8 mmol/L in hypoparathyroidism — risk of tetany and seizures
- Tetany, seizures, or laryngospasm — acute severe hypocalcemia emergency
Effective treatment of hyperparathyroidism from a parathyroid adenoma is surgical. Parathyroidectomy normalizes calcium and PTH in over 95% of patients and measurably reduces the risk of nephrolithiasis and fractures.
This article is for informational purposes only and does not replace professional medical advice. Consult an endocrinologist if your PTH level is outside the normal range.
Frequently Asked Questions
When vitamin D is deficient, intestinal calcium absorption falls — leading to chronically low blood calcium. The parathyroid glands interpret this as a threat signal and continuously release PTH, attempting to restore calcium levels by drawing on bone and kidneys. This is called secondary hyperparathyroidism — the glands are functioning correctly, responding to a genuine substrate deficit. Replenishing vitamin D normalizes PTH within 3–6 months when no organic parathyroid pathology is present.
This is called normocalcemic primary hyperparathyroidism — a relatively newly recognized form. Calcium remains normal through compensatory mechanisms, but PTH is already autonomously elevated. It is also the typical pattern for secondary hyperparathyroidism from vitamin D deficiency or early-stage CKD. Distinguishing these two situations relies on creatinine, phosphorus, and vitamin D: in secondary hyperparathyroidism, calcium is normal or low and vitamin D is deficient; in normocalcemic primary hyperparathyroidism, vitamin D is normal.
Yes — when longstanding, it is seriously harmful. Chronic osteoclast overstimulation progressively reduces bone density and causes osteoporosis, particularly in cortical bone (radius, femoral neck). Simultaneously, calcium leached from bone deposits in the kidneys — the risk of nephrolithiasis in primary hyperparathyroidism is 5–10 times the population baseline. In severe disease: subperiosteal bone resorption and 'brown tumors.' Interpreting total calcium correctly requires albumin: hypoalbuminemia falsely lowers the total calcium reading.
Yes, and this is an important postoperative scenario. During thyroidectomy, the parathyroid glands may be transiently devascularized or accidentally removed. In the first 24–72 hours postoperatively, transient hypocalcemia with compensatory PTH elevation may develop. If all four glands are damaged, permanent hypoparathyroidism follows — characterized by persistently low PTH and chronic hypocalcemia — requiring lifelong calcium and active vitamin D (calcitriol) supplementation.
Frequency depends on CKD stage. In CKD stage III: every 6–12 months; in stage IV–V: every 3–6 months. PTH in CKD is always checked alongside calcium, phosphorus, and vitamin D. Target PTH values in CKD are higher than in healthy individuals — excessive suppression leads to adynamic bone disease. Specific target ranges are determined by the nephrologist based on stage and the overall clinical picture.
No. PTH without calcium cannot be interpreted — this is an absolute rule. The same PTH value of 90 pg/mL may represent a normal result, primary hyperparathyroidism (if calcium is high), or secondary hyperparathyroidism (if calcium is normal or low and vitamin D is deficient). The mandatory minimum panel: PTH + total and ionized calcium + phosphorus + 25-OH vitamin D + creatinine. Only this combination allows the correct diagnosis and guides treatment selection.
Upload your lab results photo or PDF
AI explains your results in 30 seconds
Choose fileRate the service
Your feedback helps us improve the service