Parathyroid Hormone (PTH): Normal Levels and What Changes Mean
Bone pain without injury, recurrent kidney stones, persistent weakness — or at the opposite extreme, muscle cramps and numb fingertips. All of these can point to dysfunction of four tiny glands that most people have never heard of. Parathyroid hormone (PTH) is produced by the parathyroid glands and serves as the body's primary regulator of calcium metabolism. When it deviates from normal — in either direction — it disrupts the function of bones, kidneys, muscles, and the nervous system. This article explains how PTH works, what constitutes a normal result, why it becomes abnormal, and when treatment is needed.
What Is Parathyroid Hormone and How Does It Regulate Calcium?
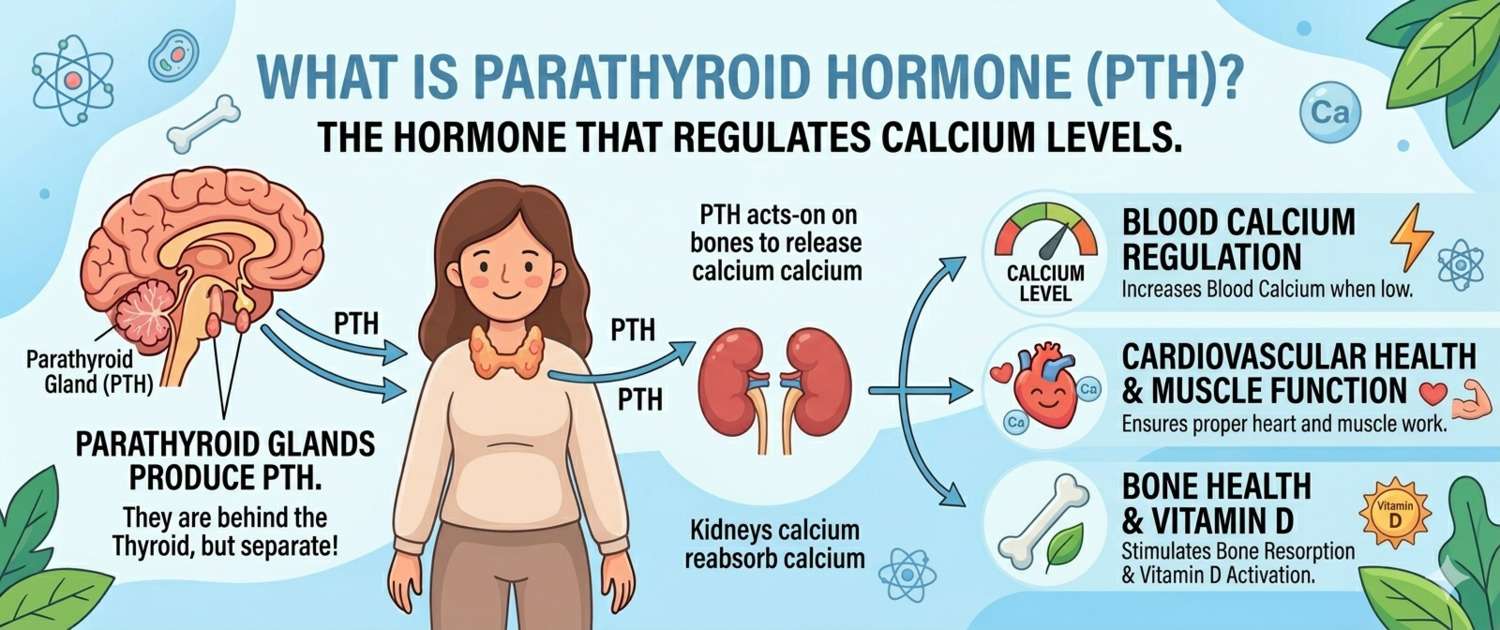
The parathyroid glands are four small, rice-grain-sized structures located on the posterior surface of the thyroid. Despite their size, they control one of the body's most critical mineral balances.
PTH is a polypeptide hormone whose primary task is to keep calcium in the blood within the narrow range of 2.15–2.55 mmol/L. This range is critical: calcium is required for muscle contraction, nerve impulse transmission, blood clotting, and bone mineralisation. Even minor deviations disrupt these processes.
The regulatory mechanism is a classic negative feedback loop:
- Blood calcium falls → parathyroid glands release PTH
- PTH acts on three target organs: bone (stimulates resorption, releasing calcium into the blood), kidneys (enhances calcium reabsorption and activates vitamin D), and intestine (via vitamin D, increases dietary calcium absorption)
- Blood calcium rises → PTH secretion is suppressed
PTH simultaneously reduces phosphorus reabsorption in the kidneys, which is why hyperparathyroidism produces a characteristic laboratory pair: rising calcium and falling phosphorus.
The close relationship between PTH and vitamin D makes their combined assessment essential: vitamin D deficiency is one of the leading causes of secondary PTH elevation.
How to Get Tested for PTH
PTH is measured in serum using immunoassay or electrochemiluminescence methods. It is almost always ordered alongside total and ionised calcium, phosphorus, and vitamin D — only in this combination does the result become clinically meaningful.
Preparation guidelines:
- Blood is drawn fasting in the morning — at least 8–12 hours after the last meal.
- Avoid alcohol and intense exercise for 24 hours beforehand.
- Calcium supplements and vitamin D should be stopped 2–3 days before the test in consultation with your doctor — they can artificially normalise the picture.
- Lithium, thiazide diuretics, and corticosteroids affect calcium metabolism — inform your doctor.
- For follow-up testing, always use the same laboratory: PTH assay methods vary significantly between labs.
Indications for ordering PTH:
- Hypercalcaemia or hypocalcaemia found on a biochemical panel
- Urinary stone disease, especially calcium-based stones
- Osteoporosis or reduced bone mineral density on densitometry
- Chronic kidney disease — mandatory monitoring
- Symptoms of hypocalcaemia: cramps, numbness, tingling
- Incidental finding during workup for fatigue or weakness
Parathyroid Hormone Normal Range: Table by Age
Reference ranges vary depending on the analytical method and laboratory.
| Category | Normal (pg/mL) | Normal (pmol/L) |
|---|---|---|
| Adults 18–30 years | 10–65 | 1.05–6.84 |
| Adults 30–70 years | 15–65 | 1.58–6.84 |
| Elderly > 70 years | 15–75 | 1.58–7.89 |
| Pregnant women | 10–60 | 1.05–6.31 |
In older adults, the upper reference limit is slightly higher — a physiological consequence of decreased calcium absorption and reduced vitamin D activation with age. A mild PTH elevation in this group does not always require treatment; the context of calcium and vitamin D levels is decisive.
During pregnancy, PTH physiologically decreases in the first half due to active calcium transfer to the foetus through the placenta and increased intestinal calcium absorption. A rise in PTH during pregnancy warrants investigation.
High PTH (Hyperparathyroidism): Causes and Symptoms
Hyperparathyroidism — excess PTH secretion — comes in three forms: primary, secondary, and tertiary.
Primary hyperparathyroidism — autonomous PTH hypersecretion by the parathyroid glands themselves, independent of blood calcium. Causes: parathyroid adenoma (80–85% of cases), hyperplasia of all four glands, rarely carcinoma. Laboratory pattern: high PTH + high calcium + low phosphorus. This is the most common cause of hypercalcaemia in outpatients.
Symptoms of primary hyperparathyroidism are classically described as "bones, stones, and groans":
- Bones: bone pain, pathological fractures, osteoporosis, cystic lesions
- Stones: recurrent kidney stones — calcium oxalate and phosphate calculi
- Groans (gastrointestinal): nausea, constipation, peptic ulcer, pancreatitis
- Neuropsychiatric symptoms: fatigue, depression, cognitive impairment; in severe hypercalcaemia — stupor and coma
Secondary hyperparathyroidism — a reactive rise in PTH in response to chronic hypocalcaemia or impaired vitamin D metabolism. The parathyroid glands are functioning normally but are forced to secrete more because of persistently low calcium. The main causes:
- Chronic kidney disease — the most common cause of secondary hyperparathyroidism in adults. Damaged kidneys fail to activate vitamin D and retain phosphorus, driving calcium down and PTH up compensatorily. In chronic kidney disease, PTH is monitored at every visit.
- Vitamin D deficiency — especially with poor nutrition, sedentary lifestyle, or malabsorption
- Malabsorption syndromes (coeliac disease, Crohn's disease, bowel resection)
- Pregnancy and breastfeeding with insufficient calcium intake
In secondary hyperparathyroidism, calcium is normal or low — unlike primary, where it is elevated. This is the key differential finding.
Tertiary hyperparathyroidism — develops after years of secondary hyperparathyroidism (most often in dialysis patients), when the glands acquire autonomy and continue to hypersecrete PTH even after calcium is normalised.
Low PTH (Hypoparathyroidism): Causes and Manifestations
Hypoparathyroidism — insufficient PTH secretion — is less common than hyperparathyroidism but clinically equally significant.
Causes of hypoparathyroidism:
- Post-surgical — the most common cause. Accidental removal or damage to the parathyroid glands during thyroid or neck surgery. Transient hypoparathyroidism occurs in 10–30% of patients after total thyroidectomy; permanent hypoparathyroidism in 1–3%.
- Autoimmune — antibodies against parathyroid cells, often as part of polyglandular autoimmune syndromes.
- Genetic — congenital absence or underdevelopment of the parathyroid glands (DiGeorge syndrome).
- Hypomagnesaemia — severe magnesium deficiency blocks PTH secretion: another reason why phosphorus and magnesium are always checked alongside calcium in calcium metabolism disorders.
- Metastatic involvement of the glands by malignant tumours.
Symptoms of hypoparathyroidism are a direct consequence of hypocalcaemia:
- Tetany — painful muscle spasms and cramps
- Paraesthesia — numbness and tingling around the mouth, hands, and feet
- Chvostek's sign (facial muscle twitch on tapping the facial nerve)
- Trousseau's sign (carpal spasm with blood pressure cuff inflation)
- Laryngospasm — potentially life-threatening
- Seizures and psychosis in severe hypocalcaemia
- Cataracts and basal ganglia calcification with prolonged disease
When PTH Results Require Medical Attention
A PTH result is always interpreted together with calcium, phosphorus, and vitamin D — in isolation it conveys little. Reasons to consult an endocrinologist:
- PTH above 100 pg/mL combined with hypercalcaemia — high probability of primary hyperparathyroidism
- PTH elevated with normal or low calcium — secondary hyperparathyroidism; vitamin D deficiency and kidney disease must be excluded
- Calcium above 3.0 mmol/L regardless of PTH level — possible hypercalcaemic crisis
- Symptoms of hypocalcaemia (cramps, numbness) with low PTH — hypoparathyroidism requiring replacement therapy
- Recurrent calcium kidney stones — screen for hyperparathyroidism
- Osteoporosis in young patients without obvious risk factors — rule out hyperparathyroidism
- After thyroid surgery — PTH and calcium monitoring in the first 24 hours
Treatment depends on the form: symptomatic primary hyperparathyroidism is treated surgically — parathyroidectomy. Secondary forms are managed by addressing the cause. Hypoparathyroidism is treated with calcium supplements and active vitamin D analogues.
Conclusion
Parathyroid hormone is an unassuming but indispensable regulator, working in constant dialogue with calcium, phosphorus, and vitamin D. Its deviation upward or downward is not a diagnosis — it is a signal: of vitamin D deficiency, a kidney problem, a parathyroid adenoma, or a surgical consequence. Correct interpretation requires combining PTH with calcium and the full clinical picture. Any abnormality warrants an endocrinology consultation and further workup — not self-treatment with calcium supplements.
This content is for informational purposes only and does not replace professional medical advice.
Frequently Asked Questions
PTH is a hormone produced by the parathyroid glands that is the body's primary regulator of blood calcium. It acts on bones, kidneys, and the gut to keep calcium in a narrow normal range. It is tested when calcium is abnormal on a biochemical panel, in recurrent kidney stones, osteoporosis, symptoms of hypocalcaemia (cramps, numbness), and chronic kidney disease. PTH alone is rarely informative — it is always ordered alongside calcium and vitamin D.
For adults aged 18–70 years, the normal PTH range is 15–65 pg/mL (1.58–6.84 pmol/L). In adults over 70, the upper limit extends slightly to 75 pg/mL. Reference ranges vary considerably between laboratories depending on the method — always check the values on your specific report. An elevated PTH is interpreted very differently depending on whether calcium is simultaneously high, normal, or low.
In primary hyperparathyroidism, the parathyroid glands produce excess PTH autonomously — most commonly due to an adenoma. Calcium is elevated. In secondary hyperparathyroidism, the glands respond correctly but are forced to work at maximum capacity because of chronically low calcium — for example, from vitamin D deficiency or chronic kidney disease. Calcium is normal or low. This key distinction determines the treatment approach.
In chronic kidney disease, vitamin D activation is impaired and phosphorus accumulates, leading to falling calcium and a compensatory rise in PTH — secondary hyperparathyroidism. Chronically elevated PTH erodes bone and accelerates vascular calcification, worsening patient outcomes. For this reason, PTH is regularly monitored in kidney disease patients alongside the kidney function test.
Cramps are a direct consequence of hypocalcaemia caused by insufficient PTH. Calcium is essential for normal neuromuscular transmission: when it falls, neurons become abnormally excitable and begin spontaneously activating muscle fibres. This is why tetany — tonic cramps, especially of the hands and face — is the hallmark symptom of hypoparathyroidism. Cramps from hypocalcaemia require prompt medical assessment.
It depends on the cause. In secondary hyperparathyroidism from vitamin D deficiency — yes: correcting the deficiency normalises PTH without surgery. In symptomatic primary hyperparathyroidism (kidney stones, osteoporosis, hypercalcaemia), the standard of care is surgical removal of the adenoma (parathyroidectomy). Medical management with calcimimetics is an option when surgery is contraindicated. Treatment strategy is determined exclusively by an endocrinologist. For more on this indicator, see parathyroid hormone.
Upload your lab results photo or PDF
AI explains your results in 30 seconds
Choose fileRate the service
Your feedback helps us improve the service