Deep Vein Thrombosis: Symptoms, Diagnosis and Treatment
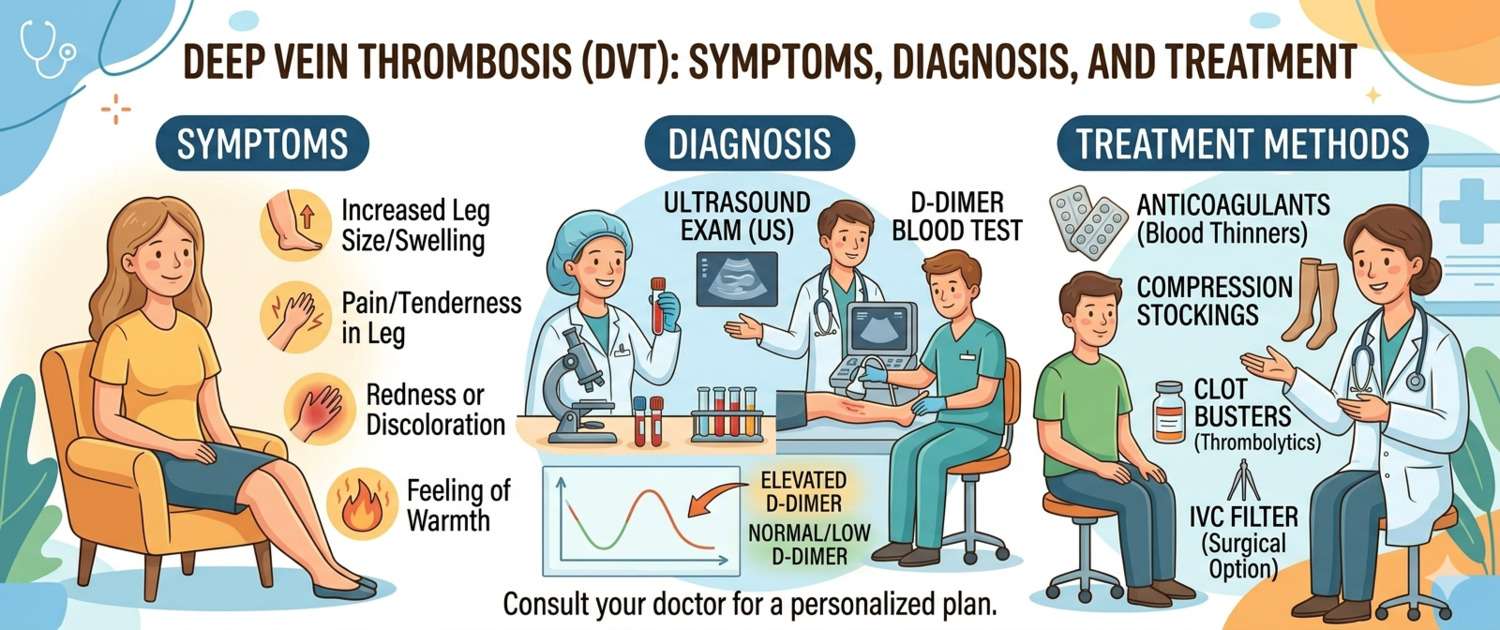
A swollen, painful leg after a long flight or bed rest — symptoms that are easy to write off as fatigue or a pulled muscle. Yet deep vein thrombosis is a condition that, without treatment, can progress to pulmonary embolism: a potentially fatal complication. Let's break down how to recognize it, which tests confirm the diagnosis, and how DVT is treated.
What Is Deep Vein Thrombosis
Deep vein thrombosis (DVT) is the formation of a blood clot in the deep veins — most often in the lower limbs: the calf, thigh, or pelvis. The clot partially or fully blocks venous return.
The main danger is clot detachment and migration to the pulmonary arteries. This is pulmonary embolism (PE) — one of the leading preventable causes of in-hospital death. DVT and PE together make up venous thromboembolism (VTE).
Causes and Risk Factors
Virchow's triad describes three conditions for clot formation: slowed blood flow, vessel wall damage, and increased blood coagulability. In practice risk factors often combine.
Triggering factors: prolonged immobility (bed rest after surgery or trauma, long flights over 4–6 hours); surgical procedures — especially joint replacement and pelvic surgery; cancer — tumors release procoagulants; pregnancy and the postpartum period; oral contraceptives and hormone replacement therapy.
Background factors: thrombophilia (factor V Leiden mutation, protein C or S deficiency); elevated homocysteine — one of the key acquired prothrombotic factors that damages vascular endothelium and activates coagulation; varicose veins; heart failure; obesity; age over 60.
Symptoms of DVT
The danger of DVT is that nearly half of cases are asymptomatic. The clot is found incidentally or after PE develops.
When symptoms are present, they are typically unilateral — an important clue:
- Swelling of one limb — from calf to thigh depending on clot level
- Pain and heaviness in the affected limb, worsening with walking
- Redness and local warmth over the clotted vein
- Homan's sign (calf pain on dorsiflexion of the foot) — low specificity, but should prompt investigation
Bilateral leg swelling is not typical for DVT — it more often points to heart or kidney failure.
Diagnosis: D-Dimer and Ultrasound
DVT diagnosis begins with clinical probability assessment using the Wells score, followed by lab testing.
D-Dimer — Screening Test
D-dimer is a fibrin degradation product released when a clot dissolves. It is elevated in thrombosis. The test's main value is a negative result: a normal D-dimer with low clinical probability virtually rules out DVT and PE, making further investigation unnecessary.
Key limitation: D-dimer rises with any inflammation, pregnancy, surgery, or cancer. A positive result alone does not confirm thrombosis — it requires further workup.
Compression Vein Ultrasound — Confirmatory Test
Compression ultrasonography of the leg veins is the diagnostic standard for DVT. The sign of thrombosis: the vein does not compress under probe pressure. Sensitivity for proximal thrombosis (femoral, popliteal veins) exceeds 95%.
Coagulation Test
A coagulation panel evaluates the clotting system overall and is needed before starting anticoagulants: INR, aPTT, prothrombin time.
| Test | Role |
|---|---|
| D-dimer | Screening: ruling out DVT at low probability |
| Vein ultrasound | Diagnosis confirmation |
| Coagulation test | Baseline clotting status before treatment |
Treatment of Deep Vein Thrombosis
The goal is to prevent clot extension, PE, and recurrence. The foundation is anticoagulant therapy.
Direct oral anticoagulants (DOACs) — apixaban, rivaroxaban — are now the first-line standard. No routine lab monitoring required. Contraindicated in severe renal failure.
Warfarin — requires regular INR monitoring (target 2.0–3.0). More complex to manage but essential in certain situations (mechanical heart valves, severe CKD).
Low molecular weight heparins — preferred in cancer, pregnancy.
Duration: provoked DVT (post-surgery, trauma) — 3 months. Unprovoked — 6 months or more; recurrent or thrombophilia-related — indefinite.
Elastic compression stockings reduce swelling, pain, and the risk of post-thrombotic syndrome — chronic venous insufficiency that develops in some patients after DVT.
Prevention of DVT
Prevention is especially important during high-risk periods: DOACs or LMWH are mandatory after joint replacement surgery; early mobilization, calf exercises, and compression stockings for prolonged immobility; for long flights — get up every 1–2 hours, stay hydrated, avoid alcohol.
When to Seek Urgent Medical Attention
Call emergency services immediately if leg swelling is accompanied by: sudden breathlessness or chest pain; coughing up blood; sudden drop in blood pressure, rapid pulse, loss of consciousness — these are signs of PE requiring emergency care.
See a doctor within hours for: new asymmetric leg swelling, especially after surgery, trauma, or prolonged immobility.
Summary
DVT responds well to treatment when diagnosed early. A normal D-dimer with low clinical probability virtually rules out the diagnosis. A swollen leg after surgery or a long flight is a reason to see a doctor immediately — not something to wait out.
This article is for informational purposes only. Interpretation of test results and treatment decisions are the responsibility of a physician.
Frequently Asked Questions
D-dimer is a fibrin breakdown product. Its elevation means active clot formation and fibrinolysis are occurring. However, D-dimer is non-specific: it rises with any inflammation, after surgery, in pregnancy, and in cancer. Its main value is the negative result: a normal D-dimer with low clinical probability reliably rules out thrombosis.
Yes — early moderate activity does not increase PE risk and actually speeds recovery. Bed rest for DVT is no longer standard practice. Walking is encouraged once anticoagulant therapy has started and compression stockings are worn. Complete immobility slows blood flow and worsens prognosis.
Superficial thrombophlebitis is inflammation of superficial veins with clotting: the vein is palpable as a painful firm cord with overlying red, warm skin. DVT affects deep venous trunks — they cannot be seen or felt. The key difference is risk: DVT carries a much higher chance of PE.
The minimum course is 3 months for thrombosis with a clear trigger (surgery, fracture). For unprovoked DVT — 6 months or more. After a second episode or with confirmed thrombophilia, indefinite therapy is often recommended. Never stop anticoagulants without medical advice.
Before anticoagulant therapy: coagulation panel (INR, aPTT), complete blood count (platelet count — critical, as heparin-induced thrombocytopenia changes the drug choice), kidney function (affects drug selection and dosing). For a first unprovoked DVT episode — thrombophilia screening is added.
Upload your lab results photo or PDF
AI explains your results in 30 seconds
Choose fileRate the service
Your feedback helps us improve the service