Atherosclerosis: Mechanism, Symptoms, Diagnosis and Treatment
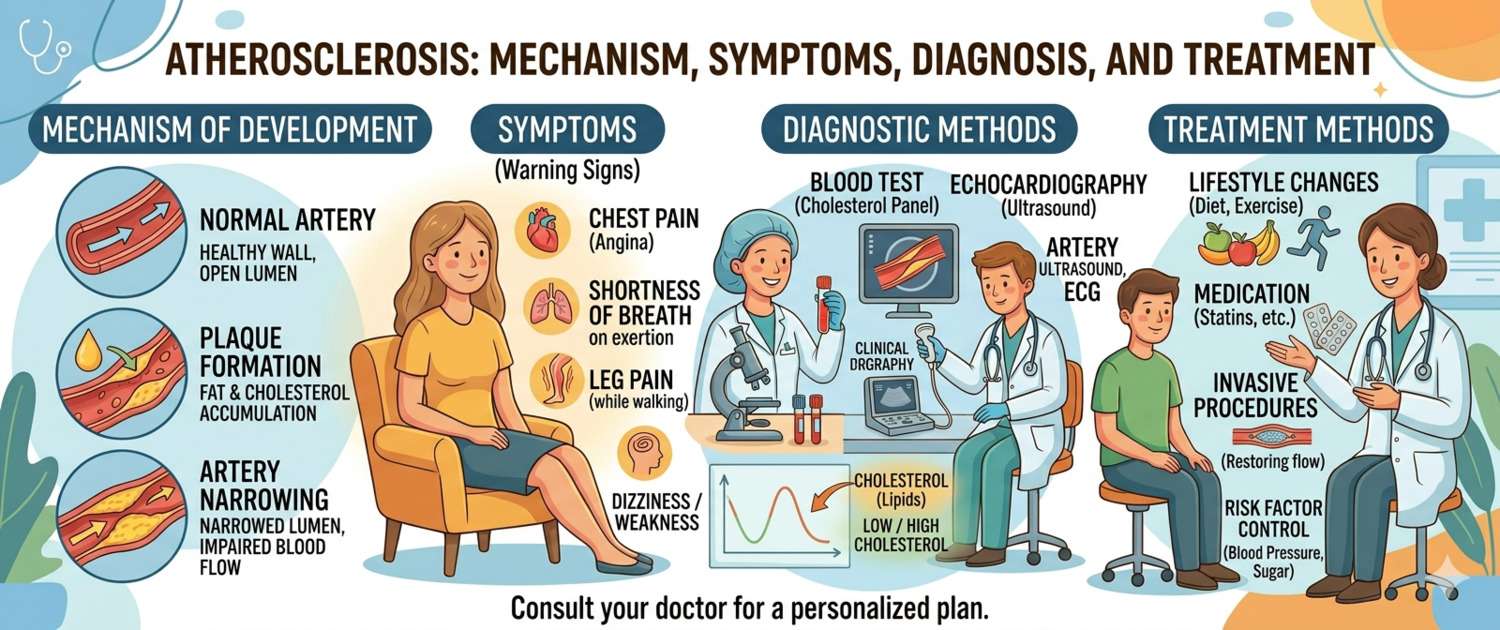
Atherosclerosis begins in youth — the first fatty streaks in the aortic wall appear in teenagers. For decades the disease progresses without symptoms, and the first sign is often a heart attack or stroke. Let's look at how an atherosclerotic plaque forms, which tests detect risk at an early stage, and what actually works to slow progression.
What Is Atherosclerosis and How Plaques Form
Atherosclerosis is a chronic inflammatory disease of the arteries in which lipids accumulate in their walls, forming atherosclerotic plaques. Plaques narrow the arterial lumen, disrupt blood flow, and can rupture — triggering thrombosis and acute vessel occlusion.
The mechanism is a multi-act story. It begins with endothelial damage — injury to the inner lining of the artery. High blood pressure, smoking, elevated glucose, chronic inflammation — all scratch this fragile surface. LDL (bad cholesterol) molecules penetrate the damaged area, oxidize, and are engulfed by macrophages that transform into "foam cells" — lipid depots that can no longer leave the vessel wall. Gradually a fibrous plaque forms with a lipid core and fibrous cap. Rupture of that cap is the trigger for thrombosis and heart attack.
Risk Factors for Atherosclerosis
Non-modifiable: age (men over 45, women over 55); male sex; family history (heart attack in first-degree relatives before 55 in men, 65 in women).
Modifiable: elevated LDL and low HDL; arterial hypertension; smoking — doubles risk; type 2 diabetes; obesity; physical inactivity; elevated triglycerides; chronic inflammation — marker C-reactive protein.
Symptoms of Atherosclerosis: When the Plaque Obstructs
Atherosclerosis is usually asymptomatic until an artery narrows by 50–70%. Symptoms depend on which arteries are affected.
Coronary arteries: angina pectoris (chest pain on exertion), myocardial infarction.
Carotid and cerebral arteries: transient ischemic attacks (TIA), stroke; tinnitus, memory and concentration decline.
Lower limb arteries: intermittent claudication — leg pain on walking that resolves at rest; in advanced cases, critical ischemia and gangrene.
Renal arteries: renovascular hypertension resistant to treatment.
Diagnosis: Lipid Panel Is the Central Test
The primary tool for atherosclerosis risk assessment is the lipid panel.
| Marker | Optimal | High risk |
|---|---|---|
| LDL | < 3.0 mmol/L | ≥ 4.0 mmol/L |
| HDL (men) | > 1.0 mmol/L | < 1.0 mmol/L |
| HDL (women) | > 1.2 mmol/L | < 1.2 mmol/L |
| Triglycerides | < 1.7 mmol/L | ≥ 2.3 mmol/L |
| Total cholesterol | < 5.0 mmol/L | ≥ 6.2 mmol/L |
After a heart attack or stroke, the target LDL level is far stricter — below 1.4–1.8 mmol/L.
High-sensitivity C-reactive protein — an inflammatory marker and independent predictor of cardiovascular events. CRP above 3 mg/L with normal LDL is a reason for more aggressive prevention.
Imaging: carotid ultrasound with intima-media thickness (IMT) measurement — direct plaque visualization; coronary calcium score (CT) — quantitative assessment of coronary artery calcification; coronary angiography — when significant stenosis is suspected.
Treatment and Prevention of Atherosclerosis
Treatment means reducing total cardiovascular risk — not just lowering cholesterol.
Lifestyle Changes
A diet low in saturated fats (red meat, butter, cheese) and trans fats (processed baked goods, fast food). The Mediterranean diet reduces cardiovascular events by 30%. Physical activity — 150 minutes of moderate exercise per week: raises HDL, lowers triglycerides and inflammation. Smoking cessation — the single most powerful risk-reduction intervention.
Statins
HMG-CoA reductase inhibitors (atorvastatin, rosuvastatin) — first-line drugs. Reduce LDL by 30–60%, decrease plaque inflammation, and stabilize the fibrous cap. Taken lifelong at high risk. Muscle pain is the most common side effect and requires monitoring.
Additional Therapy
When LDL target is not reached on statins: ezetimibe or PCSK9 inhibitors (evolocumab, alirocumab) — the latter reduce LDL by an additional 50–60%.
When to Seek Urgent Medical Attention
Immediately if: crushing chest pain radiating to the arm or jaw — possible myocardial infarction; sudden weakness or numbness of half the face, arm, or leg — possible stroke; sudden vision loss in one eye; leg pain at rest with skin color change — critical limb ischemia.
Summary
Atherosclerosis is a manageable disease with early diagnosis and active treatment. A lipid panel every 5 years from age 35–40 is the minimum screening standard. The earlier elevated LDL is found and corrected, the fewer plaques have time to form.
This article is for informational purposes only. Interpretation of test results and treatment decisions are the responsibility of a physician.
Frequently Asked Questions
The main test is a lipid panel: LDL, HDL, triglycerides, and total cholesterol. Additionally, high-sensitivity C-reactive protein as a marker of vascular wall inflammation. Fast for 9–12 hours before the test. Screening is recommended from age 35–40 every 5 years, annually with risk factors.
Complete plaque regression is rare, but stabilization and partial reduction are achievable. Intensive LDL lowering with statins combined with lifestyle change demonstrably reduces plaque volume on intravascular ultrasound. The primary goal is to make the plaque stable and prevent rupture.
LDL carries cholesterol from the liver to tissues and deposits in arterial walls when in excess — hence 'bad.' HDL removes cholesterol from tissues and returns it to the liver for elimination — 'good,' protective. The ratio matters: high LDL + low HDL is the most unfavorable combination.
At high and very high cardiovascular risk — generally yes. Atherosclerosis is a chronic disease and risk doesn't disappear once target LDL is reached. Stopping statins returns cholesterol to previous levels. At moderate risk — an individualized decision based on lifestyle and lab dynamics.
Very closely. Type 2 diabetes accelerates atherosclerosis 2–4 fold: chronically elevated glucose damages the endothelium, while the lipid profile abnormalities of diabetes — elevated triglycerides and low HDL — further increase plaque formation risk.
Yes, though the effect is moderate with normal metabolism. Saturated and trans fats raise LDL. The Mediterranean diet (olive oil, fish, vegetables, nuts) reduces cardiovascular events by 25–30%. In familial hypercholesterolemia, diet alone is insufficient — LDL cannot normalize without statins.
Upload your lab results photo or PDF
AI explains your results in 30 seconds
Choose fileRate the service
Your feedback helps us improve the service