CRP (C-Reactive Protein): Normal Range, Causes and Interpretation
A doctor ordered an "inflammation test" — and the result came back with an unfamiliar value: CRP. C-reactive protein is the fastest and most sensitive laboratory marker of acute inflammation. It responds to bacterial infection, tissue injury, or necrosis within six to twelve hours, at a stage when other markers are still within normal range. Here's what it measures, why there are two fundamentally different CRP tests, and how to interpret the result depending on the clinical situation.
What Is C-Reactive Protein and Why Is It Measured
C-reactive protein is an acute-phase protein synthesised by the liver in response to the signalling cytokine interleukin-6 (IL-6). It got its name in 1930, when researchers discovered that a protein from the blood of pneumonia patients reacted with the C-polysaccharide of pneumococcus. It was later found that CRP is produced universally — in any inflammation, infection, or tissue necrosis, regardless of the cause.
The mechanism is straightforward: when damage or threat is detected, immune cells release IL-6. The liver receives the signal and within hours sharply increases CRP synthesis. This protein binds to dead cells and pathogens, activates the complement system, and flags targets for phagocytes. CRP is among the first organised responses to tissue injury.
In clinical practice, CRP is measured in two formats — and understanding which one is in front of you is essential before interpreting the result.
Two Types of Test: Standard CRP and High-Sensitivity hs-CRP
These are not the same test in different units — they are two fundamentally different clinical tools with different purposes.
Standard CRP (sensitivity down to 5–8 mg/L) is used to diagnose and monitor acute inflammation: infections, autoimmune flares, post-surgical status. It cannot detect changes below its sensitivity threshold — which means it is not suitable for assessing low-grade chronic inflammation.
High-sensitivity CRP (hs-CRP) (sensitivity down to 0.1 mg/L) is used to assess long-term cardiovascular risk in apparently healthy individuals or those at established risk. Chronic subclinical inflammation in arterial walls — invisible to the standard test — is detected by hs-CRP.
Important: if the report simply says "CRP" without qualification, it is almost certainly the standard test. If it says "hs-CRP" or "high-sensitivity CRP," it is a cardiovascular risk test.
Normal CRP Values: Standard Test and hs-CRP
Reference ranges differ fundamentally depending on which test is used:
Standard CRP:
| Value | Interpretation |
|---|---|
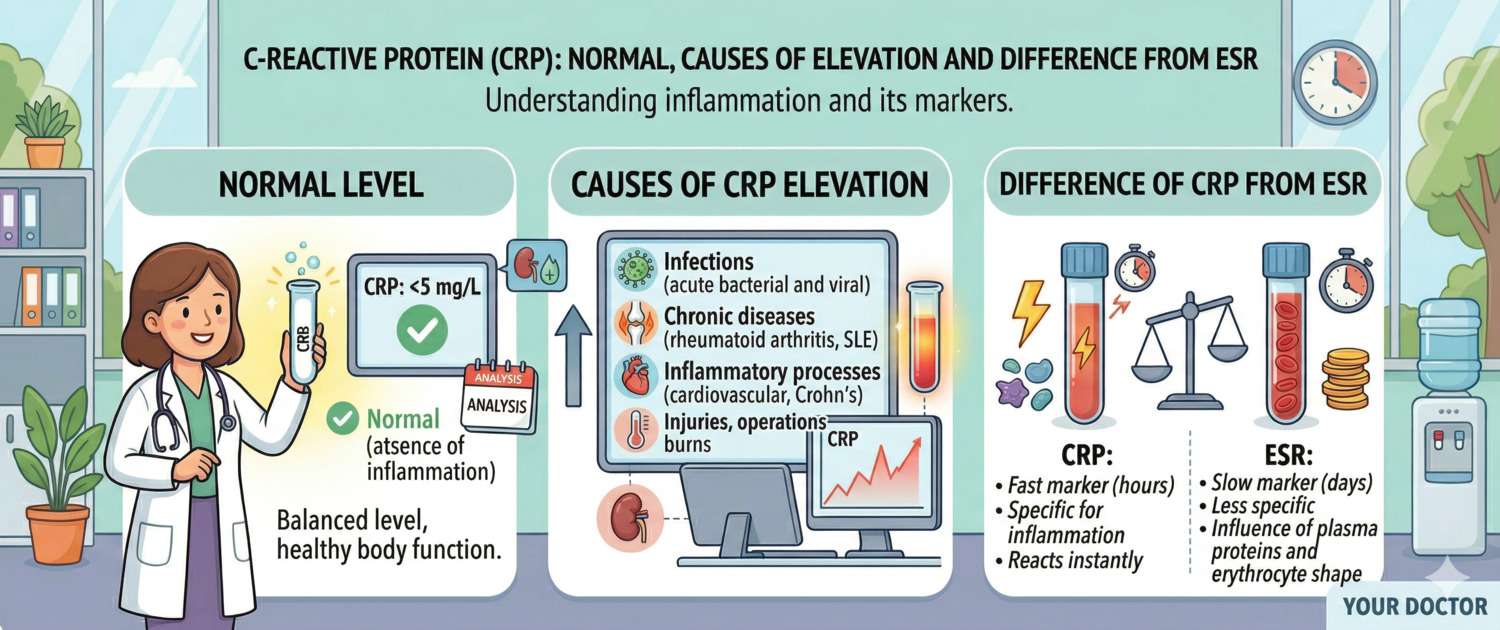
| < 5 mg/L | Normal, no inflammation |
| 5–10 mg/L | Mild elevation |
| 10–100 mg/L | Moderate to significant elevation |
| > 100 mg/L | Marked elevation |
High-sensitivity hs-CRP (cardiovascular risk):
| Value | Cardiovascular Event Risk |
|---|---|
| < 1 mg/L | Low |
| 1–3 mg/L | Moderate |
| > 3 mg/L | High |
| > 10 mg/L | Acute inflammation present — not interpretable as cardiac risk |
Reference ranges may vary slightly between laboratories. Always use the values printed on your specific report.
Why CRP Is Elevated: Degrees and Causes
The degree of CRP elevation helps orient the clinical search — though the result alone never establishes a diagnosis without the full clinical picture.
Mild elevation (5–20 mg/L): viral infections (respiratory viruses, influenza), chronic inflammatory conditions in remission, moderate physical exertion, obesity. In uncomplicated viral respiratory illness, CRP rarely exceeds 20–30 mg/L — this is a useful practical threshold.
Moderate to significant elevation (20–100 mg/L): bacterial infections (pneumonia, pyelonephritis, cellulitis), autoimmune flares (rheumatoid arthritis, systemic lupus, Crohn's disease), surgical procedures and trauma. CRP above 50 mg/L during an acute respiratory illness is an argument in favour of a bacterial cause or complication.
Marked elevation (> 100 mg/L): severe bacterial infection, sepsis, extensive tissue necrosis — as occurs in myocardial infarction. In septic states, CRP can exceed 300–400 mg/L. Values at this level require immediate investigation.
A separate category is malignancy: in many cancers, CRP is chronically mildly elevated without infectious cause, reflecting paraneoplastic inflammation.
CRP vs ESR: The Key Differences
Both are inflammation markers, but with different kinetics and clinical meaning. Together they give a more complete picture than either alone.
| Parameter | CRP | ESR |
|---|---|---|
| Response to inflammation | Within 6–12 hours | Within 24–48 hours |
| Normalisation | Within 3–7 days | Over weeks to months |
| Specificity | Higher | Lower |
| Response to viral infections | Weak | Moderate |
| Effect of pregnancy | Unchanged | Elevated |
| Best use | Acute monitoring, antibiotic response | Chronic inflammation activity |
In practice: CRP is better for diagnosing acute conditions and tracking antibiotic response — if CRP does not fall within 48–72 hours of therapy, the treatment plan is reassessed. ESR is more inert and better reflects the activity of chronic inflammatory disease over time.
How to Prepare for the Test
Blood is drawn fasting — after eight hours without food. Avoid alcohol and intense physical activity for 24 hours beforehand: physical stress mildly raises CRP through muscle inflammation.
Important: do not test during an acute illness if the goal is to assess baseline cardiovascular risk using hs-CRP. Any active infection or inflammation will push the value above 10 mg/L — making the result uninformative for risk stratification.
Tell your doctor about all medications. Statins reliably lower hs-CRP independently of their cholesterol effect — their use changes the interpretation of results. Oral contraceptives raise CRP. NSAIDs (ibuprofen, diclofenac) may artificially suppress the value.
For a complete assessment of the inflammatory picture, CRP is always read alongside neutrophils, ESR, and when relevant, liver function tests — an elevated CRP alongside abnormal liver enzymes may point to a hepatological source of inflammation.
When to Seek Urgent Medical Attention
Call emergency services immediately if high CRP is accompanied by:
- Temperature above 39°C with chills and rapidly worsening weakness — signs of sepsis.
- Chest pain — high CRP in the context of infarction reflects the scale of myocardial necrosis.
- Confusion or sudden drop in blood pressure.
Schedule a routine appointment with a GP if:
- CRP is elevated on repeat tests without an obvious cause.
- hs-CRP is consistently above 3 mg/L — even without symptoms.
- CRP is falling more slowly than expected during antibiotic treatment.
Conclusion
C-reactive protein is the most timely marker of inflammation: it responds earlier than ESR, rises in proportion to disease severity, and falls as recovery proceeds. The degree of elevation helps distinguish viral from bacterial infection, assess severity, and track treatment response. High-sensitivity hs-CRP is a separate tool — designed for those without acute inflammation who have questions about long-term cardiovascular risk.
For the role of hs-CRP in assessing biological age and long-term health monitoring strategy, see the article biological age by blood tests. For chronic inflammation (inflammaging), optimal hs-CRP targets for longevity and a reduction protocol, see the article hs-CRP and longevity.
This article is for informational purposes only. Interpreting test results and prescribing treatment is exclusively the responsibility of a physician.
Frequently Asked Questions
Elevated CRP means inflammation, infection, or tissue necrosis is present somewhere in the body. A level of 5–20 mg/L is typical of viral infections and mild inflammation. Values above 50 mg/L point to bacterial infection or an autoimmune flare. Above 100 mg/L indicates severe inflammation requiring urgent investigation. CRP should always be interpreted alongside ESR and the clinical picture.
They are two different clinical tools. Standard CRP is used to diagnose acute inflammation — infections, chronic disease flares, trauma. High-sensitivity hs-CRP is used to assess long-term cardiovascular risk in people without obvious inflammation: a value above 3 mg/L on hs-CRP indicates elevated risk of heart attack and stroke.
Both reflect inflammation, but at different speeds. CRP responds within 6–12 hours and normalises in 3–7 days — making it better for acute diagnosis and treatment monitoring. ESR rises more slowly (24–48 hours) and remains elevated for weeks — it better reflects chronic inflammatory activity over time. Used together, they complement each other.
Yes. Beyond infections, CRP rises with autoimmune diseases (rheumatoid arthritis, lupus, Crohn's disease), malignancies, myocardial infarction, surgery, and trauma. Mild chronic hs-CRP elevation without symptoms may indicate subclinical vascular inflammation. Obesity itself chronically raises baseline CRP levels.
Fast for eight hours before the draw. Avoid alcohol and intense physical activity for 24 hours. If the goal is cardiovascular risk assessment with hs-CRP, do not test during an acute illness — any active infection will push the value above 10 mg/L and make the result uninterpretable for risk purposes. Tell your doctor about statins and NSAIDs, as both affect CRP levels.
With appropriate antibiotic therapy, CRP begins declining within 24–48 hours. If the level does not fall — or continues rising — after 72 hours of treatment, this signals treatment failure, a complication, or an unrecognised infection focus. This is exactly why CRP is used as a treatment response marker: doctors order a repeat test two to three days into therapy to assess the trend.
Upload your lab results photo or PDF
AI explains your results in 30 seconds
Choose fileRate the service
Your feedback helps us improve the service