Hypoglycemia and Panic Attacks: Sugar Crashes and Anxiety
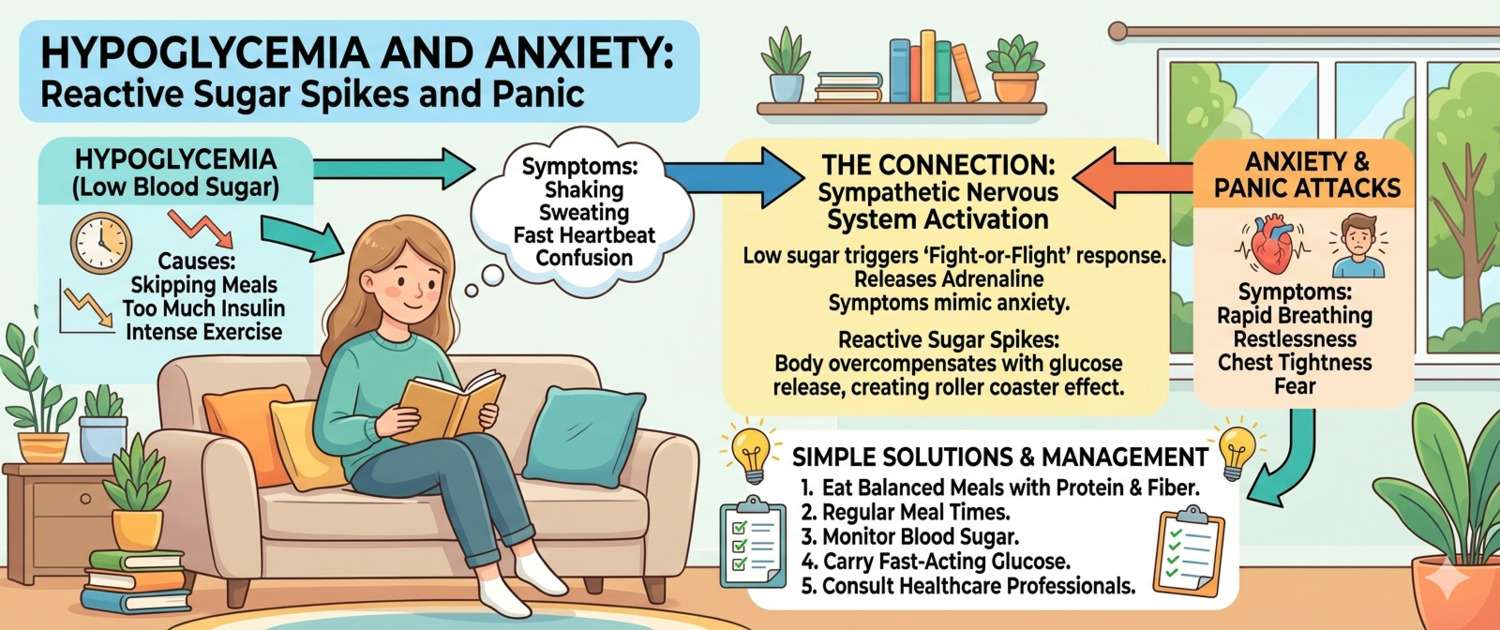
Reactive hypoglycemia is a state in which blood glucose falls sharply 1.5–3 hours after a meal, typically one rich in fast-acting carbs. The biochemical symptoms — palpitations, sweating, tremor, anxiety, fear — are identical to a panic attack. In a substantial share of patients diagnosed with "panic attacks," the cause is hypoglycemic, and it isn't picked up by a standard fasting glucose test. Here's how to tell, which tests help, and what to do.
What Hypoglycemia Is and Why It Causes Anxiety
Hypoglycemia is a drop in blood glucose below 3.5–3.9 mmol/L. When the brain senses the fall, it triggers a powerful emergency response through the sympathetic nervous system: an adrenaline and cortisol surge designed to mobilize glucose stores.
The adrenergic response produces a characteristic symptom complex:
- Rapid heartbeat, the sensation of a "pounding" heart
- Sweating, particularly cold sweating
- Hand tremor, internal shakiness
- Anxiety, fear that "something bad is about to happen"
- Pallor, dizziness
- Hunger, often overwhelming
- Sometimes — impaired concentration, mental confusion
This is a panic attack — biochemically. The difference is that in a "classic" panic attack, adrenaline releases without an obvious cause (a false brain alarm), while in hypoglycemia it's a response to a real physiological signal. The symptoms are identical, but the mechanisms differ.
Reactive Postprandial Hypoglycemia
The most common clinically meaningful form of hypoglycemia in non-diabetics is reactive (postprandial) hypoglycemia. The scenario:
- The person eats a meal with fast carbs (sweet breakfast, pastry, soda)
- Blood glucose rises sharply — within 30–60 minutes to 8–10 mmol/L
- The pancreas releases a powerful "insulin response"
- 1.5–3 hours later, glucose drops sharply — sometimes below 3.5 mmol/L
- The brain triggers an adrenergic response — a panic attack
At-risk groups:
- Insulin resistance (HOMA-IR > 2.5) — the pancreas overshoots with excess insulin
- Fans of "fast" carbs on an empty stomach
- Long meal gaps (more than 5–6 hours)
- Alcohol on an empty stomach
- Post-bariatric patients (dumping syndrome)
- Rare causes — insulinoma (β-cell pancreatic tumor)
If anxiety attacks occur 1.5–3 hours after meals and resolve with eating, that's a strong argument for a hypoglycemic component.
Hypoglycemia Symptoms vs Panic Attack
Biochemically the symptoms overlap almost completely. The differences are in the details:
| Feature | Panic attack | Reactive hypoglycemia |
|---|---|---|
| Timing | Random, no obvious trigger | 1.5–3 hours after eating |
| Link to food | None | Direct |
| Relief from eating | None | Yes, noticeable |
| Hunger | May be absent | Often pronounced |
| Relation to exercise | Weak | Worsens with exercise on empty stomach |
| Severe tremor | Possible | More pronounced |
| Relief from glucose (sugar, juice) | Weak | Quick (5–10 minutes) |
A key diagnostic clue: if someone carries a candy and eats a piece during an "attack" — and feels better in 5–10 minutes — it's not a panic attack, it's hypoglycemia.
Which Tests to Take
A standard "fasting glucose" is often normal in reactive hypoglycemia. Catching the problem requires other approaches:
Base block:
- Fasting glucose — within 4.1–5.9 mmol/L
- Fasting insulin — target 3–8 µIU/mL
- HOMA-IR (calculated from glucose and insulin) — target < 2.0
- HbA1c — glycated hemoglobin for average glycemia
For suspected insulin resistance:
- Fasting C-peptide — assesses real insulin secretion
Oral glucose tolerance test (OGTT) with insulin:
Performed in a lab: fasting glucose + insulin, followed by 75 g glucose, then measurements at 30, 60, 120 minutes. In reactive hypoglycemia patients:
- At 60–90 min — peak glucose and sharp insulin spike
- At 120 min — glucose falls below baseline, sometimes below 3.5 mmol/L
- Anxiety/panic symptoms appear
This is the gold standard for diagnosing reactive hypoglycemia.
Food + symptom diary:
The cheapest and often most informative tool. For 2 weeks, record everything eaten, the time, and any anxiety symptoms. The "1.5–3 hours after eating → attack" pattern becomes obvious.
All these markers are conveniently drawn via the anxiety causes panel or the hormone panel.
How to Stabilize Blood Sugar: Food and Lifestyle
The main principle is glucose stabilization through food:
Do:
- Eat every 4–5 hours; avoid gaps over 5–6 hours
- Combine protein + slow carbs + healthy fats at every meal
- A protein breakfast (eggs, cottage cheese, fish) prevents morning swings
- Sweets only after meals, never on an empty stomach
- Avoid fast carbs on empty stomach (fruit, juice, pastry)
- Caffeine — after eating, not on empty stomach (which raises cortisol and provokes hypoglycemic swings)
Don't:
- Long meal gaps
- Strict intermittent fasting if hypoglycemia is suspected
- Alcohol on empty stomach
- Sweet breakfast (cereals, pastry, fruit juice) — almost guaranteed swing
- Keto without adaptation — some people get hypoglycemic episodes in the first weeks
Helpful:
- Magnesium — stabilizes the insulin response
- Chromium — insulin signaling cofactor
- Regular moderate exercise — improves insulin sensitivity
Stable glucose isn't a "diet" — it's a steady background on which anxiety symptoms drop substantially in many people.
When to See a Doctor
To an endocrinologist — for:
- Confirmed reactive hypoglycemia on OGTT
- HOMA-IR > 4 (significant insulin resistance)
- Fasting hypoglycemia episodes (could be insulinoma)
- Hypoglycemia in a diabetic on insulin or sulfonylureas
To a psychiatrist/psychotherapist — if:
- Tests and OGTT are normal
- Panic symptoms are unrelated to meals
- Anxiety disorder exists as a primary diagnosis
For details on insulin resistance and treatment see insulin resistance and fasting insulin. For the full panic approach see panic attacks: causes, symptoms and tests.
This article is for informational purposes only and does not replace professional medical advice. Recurrent hypoglycemia episodes warrant endocrinology evaluation.
Frequently Asked Questions
Reactive hypoglycemia happens 1.5–3 hours after eating (especially fast carbs) and resolves quickly with food or glucose. A panic attack happens "for no reason" and isn't relieved by eating. Carrying a piece of sugar or juice and eating it during an attack — with hypoglycemia, relief comes in 5–10 minutes; with a panic attack, no. Keep a food + symptom diary for 2 weeks — the pattern becomes obvious. Tests — fasting insulin with HOMA-IR and, if suspected, OGTT with insulin.
Fasting glucose alone is often normal, so it's not enough. Informative: fasting glucose + insulin with HOMA-IR, HbA1c, C-peptide. Gold standard — OGTT with insulin: 75 g glucose with measurements at 30, 60, 120 minutes. In reactive hypoglycemia patients there's a characteristic pattern: high 60-min insulin peak and 120-min glucose below baseline. The full set is convenient via the anxiety causes panel.
Classic reactive hypoglycemia. Fast carbs (sugar, juice, pastry) cause a sharp glucose rise → strong insulin response → 1.5–3 hours later glucose falls below baseline → the brain triggers an adrenergic response → anxiety, palpitations, sweating. In people with insulin resistance (HOMA-IR > 2.5) this effect is especially pronounced — the pancreas overshoots, and the swings are deeper. The fix — protein and slow carbs with sweets, never on empty stomach.
With reactive hypoglycemia — yes, substantially. Glucose stabilization via protein-slow-carb meals, no fast sugars on empty stomach, and meal regularity reduces panic episodes substantially in 2–4 weeks for most people. This isn't a "trendy" diet — it's biochemical stabilization. With panic without hypoglycemia, sugar-free eating doesn't help directly — psychotherapy works there. For more see fasting insulin.
If reactive hypoglycemia symptoms exist (anxiety/panic 1.5–3 hours post-meal) and fasting glucose and insulin are normal — OGTT with insulin confirms or excludes the diagnosis. It's a 3-hour lab session with blood draws at 0, 30, 60, 90, 120 minutes. The test is safe but unpleasant for symptomatic patients — symptoms can occur during the test, which is itself diagnostic. Ordered by an endocrinologist.
Upload your lab results photo or PDF
AI explains your results in 30 seconds
Choose fileRate the service
Your feedback helps us improve the service