Reticulocytes in Blood: Normal Levels, Causes and Meaning
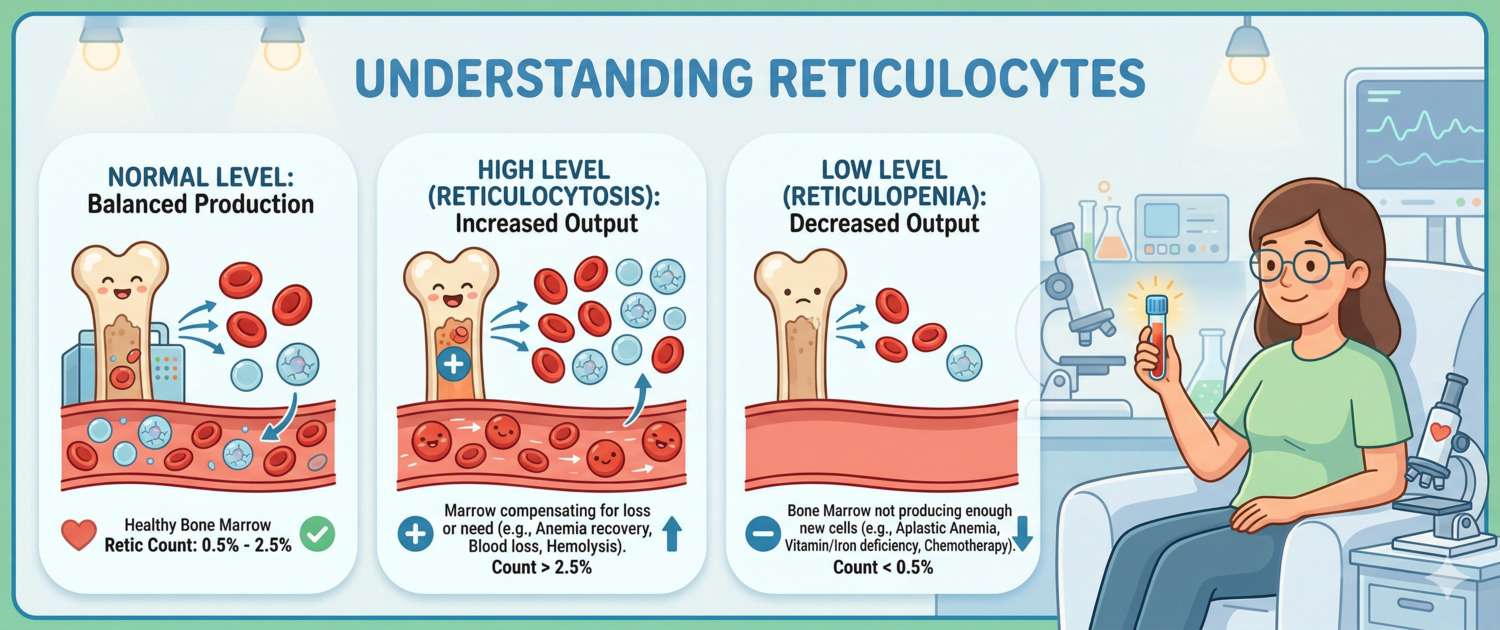
Reticulocytes are young red blood cells that have just left the bone marrow. Their count in blood is a direct window into hematopoietic activity: when reticulocytes rise, the bone marrow is working harder; when they fall, erythropoiesis is suppressed. This is why reticulocytes are indispensable in the differential diagnosis of anemia — they immediately answer the question of whether the bone marrow is the problem or whether the cause lies elsewhere. This marker is rarely included in a routine blood count, but when hemoglobin deviates from normal, it becomes one of the most informative values available.
What Reticulocytes Are and How They Form
Reticulocytes are immature red blood cells — an intermediate stage between the normoblast (a nucleated precursor) and the mature erythrocyte. They form in the bone marrow during erythropoiesis: once an erythroblast expels its nucleus, it enters the bloodstream as a reticulocyte still containing remnants of ribosomes and mitochondria. These organelles, staining with special dyes, produce the characteristic "net-like" pattern — hence the name.
Under normal conditions, a reticulocyte matures in the bloodstream within 1–2 days, becoming a fully mature anucleate red cell. Their proportion in blood directly reflects the rate of new red cell production. The principal driver of erythropoiesis is erythropoietin (EPO), produced by the kidneys in response to tissue hypoxia.
The speed of the reticulocyte response to a stimulus is one of its key diagnostic features. In acute blood loss or hemolysis, the bone marrow sharply increases output: the reticulocytosis peak occurs at 5–7 days. When treatment for iron deficiency anemia begins, reticulocytes start rising within 3–5 days — the first laboratory sign of a therapeutic response.
Normal Reticulocyte Levels
Reticulocytes are expressed in two ways: as a percentage of total red blood cells (relative value) and as an absolute count (cells per liter). The absolute count is more informative in anemia: when total red cell count drops sharply, the relative percentage can appear "normal" even though the bone marrow is actually working inadequately.
| Group | Normal (%) | Normal (×10⁹/L) |
|---|---|---|
| Newborns (days 1–7) | 2.0–6.0 | 110–450 |
| Infants under 2 weeks | 0.5–1.5 | 30–100 |
| Infants 2 weeks – 1 year | 0.5–1.5 | 25–85 |
| Children 1–6 years | 0.5–1.5 | 25–75 |
| Children 6–12 years | 0.5–1.5 | 25–70 |
| Adult men | 0.5–1.5 | 25–75 |
| Adult women | 0.5–2.0 | 25–85 |
| Pregnant women | up to 2.5 | up to 100 |
A more precise tool is the reticulocyte production index (RPI): it corrects the relative percentage for the degree of anemia and the reticulocyte maturation time. RPI = (Reticulocyte% × Patient hematocrit) / (Normal hematocrit × Maturation time). RPI > 2 = adequate bone marrow response; RPI < 2 = inadequate, hypoproliferative anemia.
How to Prepare for a Reticulocyte Test
Reticulocytes are measured as part of an extended complete blood count — using automated hematology analyzers or manual stained smear counting.
- Blood is drawn from a vein in the morning, fasting or 3–4 hours after a light meal — food intake does not significantly affect the result
- Intense exercise the day before transiently raises reticulocytes — avoid strenuous training for 24 hours before the draw
- Blood transfusions in the preceding 4–6 weeks distort the result — donor cells alter the ratio
- Recently initiated treatment with iron, vitamin B12, or folate causes reticulocytosis — this is an expected therapeutic response, not pathology; inform the physician interpreting the result
- For serial monitoring (e.g., tracking treatment response) use the same laboratory each time
Reticulocytes should always be interpreted alongside hemoglobin, hematocrit, and other blood indices — in isolation they provide very limited information.
Causes of High Reticulocytes (Reticulocytosis)
Reticulocytosis — above 2% or > 100×10⁹/L — means the bone marrow has sharply accelerated red cell production. This is always a response to something: blood loss, hemolysis, or the start of anemia treatment.
Blood loss. Acute or chronic blood loss is the most common cause of reticulocytosis. The hypoxia that develops with anemia stimulates EPO production, which drives the bone marrow. The response peaks on days 5–7 after the bleeding episode.
Hemolytic anemia. When red cells are destroyed prematurely — by autoimmune, mechanical, or toxic mechanisms — the bone marrow increases output to compensate. Reticulocytosis in hemolysis is often marked: > 5%, in severe cases > 10–15%. Characteristic combination: reticulocytosis + elevated indirect bilirubin + reduced haptoglobin.
Response to anemia treatment. Three to five days after starting iron therapy for iron deficiency anemia, or vitamin B12/folate for megaloblastic anemia, reticulocytes begin rising — the "reticulocyte crisis." This is the first laboratory sign of an effective treatment response. The peak occurs on days 7–10.
Physiological causes: in newborns during the first week of life, reticulocytosis up to 6% is normal — fetal hemoglobin is being replaced. Moderate reticulocytosis up to 2–2.5% is also physiological in pregnancy. High-altitude residence sustains chronically elevated levels through persistent mild hypoxia.
Less common causes: polycythemia vera — autonomous red cell overproduction; bone marrow metastases displacing normal cells (leukoerythroblastic reaction); extramedullary hematopoiesis in myelofibrosis.
Causes of Low Reticulocytes (Reticulocytopenia)
Reticulocytopenia — below 0.5% or < 20×10⁹/L in the setting of anemia — signals that the bone marrow is failing to keep up. This is a hypoproliferative anemia: the problem is not loss or destruction of red cells, but insufficient production.
Deficiency anemias before treatment. In iron deficiency anemia and megaloblastic anemia (B12 or folate deficiency), the bone marrow cannot produce red cells normally because the necessary substrate is absent — reticulocytes are reduced or at the low end of normal.
Aplastic anemia. Severe damage to bone marrow stem cells — autoimmune, toxic, or idiopathic. Pancytopenia with reticulocytopenia is the classic presentation: simultaneous drops in hemoglobin, leukocytes, and platelets with no reticulocyte response.
Chronic kidney disease. Renal erythropoietin is the primary bone marrow stimulus. When kidney function declines, EPO production falls disproportionately — producing a normochromic normocytic anemia with an inappropriately low reticulocyte count for the degree of anemia.
Malignancy and chemotherapy. Bone marrow infiltration by tumor cells or suppression of hematopoiesis by cytotoxic agents — direct causes of reticulocytopenia.
Other causes: hypothyroidism (reduced metabolic demands decrease erythropoiesis), chronic inflammation (anemia of chronic disease — reticulocytes low or normal despite low hemoglobin), direct alcohol toxicity to erythroblasts.
Reticulocytes in the Differential Diagnosis of Anemia
The main clinical value of reticulocytes is separating anemias into regenerative and aregenerative. This is the first and most fundamental step in diagnosing any anemia.
| Type of anemia | Reticulocytes | Hemoglobin | Typical cause |
|---|---|---|---|
| Hemolytic | Markedly ↑ (> 5%) | Low | Autoimmune hemolysis, hemoglobinopathies |
| Post-hemorrhagic (acute) | ↑ (peak days 5–7) | Low | Bleeding |
| Iron deficiency | Low or normal | Low | Iron deficit: low ferritin |
| Megaloblastic (B12/folate) | Low | Low | Vitamin B12 or folate deficiency |
| Aplastic | Markedly ↓ | Low | Bone marrow failure |
| Renal (EPO deficiency) | Low | Low | CKD, normocytosis |
| Anemia of chronic disease | Low or normal | Low | Inflammation, iron redistribution |
The algorithm is straightforward: in any anemia, look at reticulocytes first. High → investigate blood loss or hemolysis. Low → assess bone marrow, iron stores, B12, folate, kidney function. This two-step approach saves time and avoids unnecessary testing.
When Reticulocyte Abnormalities Require Medical Attention
An isolated minor reticulocyte deviation with normal hemoglobin is generally not a cause for concern. Clinical significance arises when reticulocytes deviate in the context of anemia or progressive symptoms.
Scheduled visit to a doctor when:
- Anemia with below-normal reticulocytes — to identify the cause of hypoproliferation
- Reticulocytosis without an obvious cause (no recent blood loss, no anemia treatment) — rule out hemolysis
- Reticulocytes > 5% combined with jaundice or dark urine
Seek urgent care when:
- Reticulocytopenia combined with pancytopenia — possible aplastic anemia
- Worsening anemia with reticulocytes < 0.2% — critically suppressed bone marrow
- Reticulocytosis > 10% — severe hemolytic crisis
After starting anemia treatment: a follow-up reticulocyte count at 7–10 days confirms the bone marrow response before hemoglobin has time to normalize — this is the earliest reliable marker of treatment efficacy.
This article is for informational purposes only and does not replace professional medical advice. Consult a GP or hematologist if your reticulocyte count is outside the normal range.
Frequently Asked Questions
Elevated reticulocytes mean the bone marrow is actively producing new red blood cells in response to some stimulus. Most commonly this is blood loss, hemolysis (accelerated red cell destruction), or the start of anemia treatment with iron, vitamin B12, or folate. Reticulocytosis in a patient who has just begun iron deficiency anemia treatment is a good sign — the body is responding to therapy as expected. Reticulocytosis without an identified cause is an indication to search for occult blood loss or hemolysis.
In iron deficiency, the bone marrow cannot synthesize hemoglobin normally — iron is required to build heme. Erythroblasts divide but stall at the maturation stage, failing to release sufficient reticulocytes into circulation. This is what distinguishes iron deficiency anemia from hemolytic anemia: hemolysis gives high reticulocytes, while deficiency anemias give low or normal counts. ESR in iron deficiency is typically low or normal — another distinguishing feature from inflammatory anemias.
Reticulocytes respond to effective treatment far faster than hemoglobin. With correctly chosen therapy — iron, vitamin B12, or folate depending on the deficiency — reticulocytes begin rising within 3–5 days, peaking on days 7–10 (the 'reticulocyte crisis'). Hemoglobin starts rising only after 2–4 weeks. A follow-up reticulocyte count at 7–10 days after starting treatment is therefore the earliest way to confirm that therapy is working, well before hemoglobin normalizes.
Yes. In newborns during the first week of life, reticulocytosis up to 6% is a physiological norm — fetal hemoglobin is transitioning to adult hemoglobin. Moderate reticulocytosis up to 2–2.5% is also normal in pregnancy. At high altitude, chronic mild hypoxia maintains a persistently elevated level. A transient rise after intense physical exercise is possible. In all these cases, hemoglobin is normal or elevated — a key distinguishing feature from pathological reticulocytosis.
They reflect different stages of the same process. Transferrin reflects transport capacity — how much iron the blood can carry to the bone marrow: in iron deficiency it rises as a compensatory response. Reticulocytes reflect the end result: how many new red cells the bone marrow is actually releasing into the blood. In iron deficiency anemia, transferrin is high while reticulocytes are low — the body is trying to transport iron but there is none to carry. After treatment begins, transferrin starts falling as reticulocytes rise.
On modern automated analyzers, reticulocytes can be counted automatically as part of an extended complete blood count — it is sufficient to specify this when ordering the test. Standard CBC panels without specific instructions often do not include reticulocytes. When anemia is suspected, treatment is being monitored, or bone marrow function is being assessed, specifically request a 'CBC with reticulocytes' or order reticulocytes separately — it requires the same blood draw with no additional preparation.
Upload your lab results photo or PDF
AI explains your results in 30 seconds
Choose fileRate the service
Your feedback helps us improve the service