Normal Hemoglobin Levels: Table by Age, Sex and Pregnancy
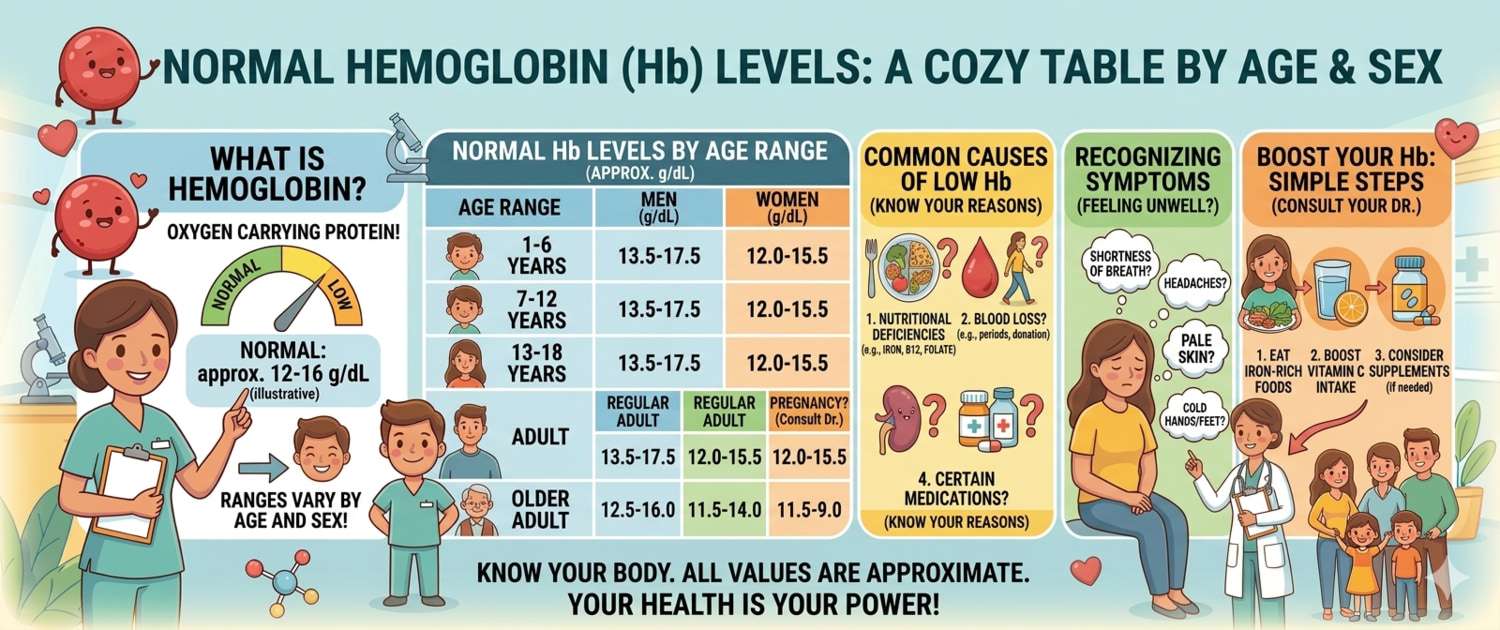
Hemoglobin is in every complete blood count, yet few people understand why the normal range differs between men and women, why it is lower in pregnancy, and why newborns have values far above the adult range. Understanding these distinctions matters — both to avoid unnecessary alarm and to know when a result genuinely warrants medical attention. This article provides complete reference tables, explains the logic behind the differences, and gives a clear interpretation of what deviations mean.
What Is Hemoglobin and Why Is It Measured?
Hemoglobin is a protein inside red blood cells that contains an iron atom. It carries oxygen from the lungs to every tissue in the body and transports carbon dioxide back. Without enough hemoglobin, cells begin to "suffocate" — even with normal breathing and heart function.
Hemoglobin is measured as part of a complete blood count — there is no separate "hemoglobin-only" test. Results are expressed in grams per litre (g/L) or grams per decilitre (g/dL): 1 g/dL = 10 g/L.
Why do normal ranges differ between groups? Because hemoglobin levels depend on several physiological factors:
- Sex: testosterone in men stimulates erythropoietin production and haemoglobin synthesis. As a result, men's normal hemoglobin is 10–20 g/L higher than women's.
- Age: newborns have very high hemoglobin (foetal hemoglobin, adapted to low oxygen in the womb), which then drops sharply by 2–3 months, rises again toward school age, and reaches adult values by adolescence.
- Pregnancy: plasma volume expands by 40–50% during pregnancy, while red cell mass increases by only 20–30%. Blood is "diluted," physiologically lowering hemoglobin.
- Altitude: residents of high-altitude areas have elevated hemoglobin as an adaptation to reduced oxygen partial pressure.
How to Get Tested
Hemoglobin is measured by automated analyser from capillary (fingerstick) or venous blood. It is relatively stable and does not require the strict preparation needed for hormonal tests. A few guidelines nonetheless:
- Ideally draw blood fasting in the morning — eating beforehand can cause a mild haemodilutional drop.
- Avoid intense physical exercise for 24 hours: strenuous activity causes transient haemoconcentration.
- Smoking within 30 minutes before the draw raises carboxyhaemoglobin (an inactive form), slightly inflating the total.
- For serial monitoring — always use the same laboratory: different measurement methods yield marginally different values.
- Important: dehydration (heat, vomiting, diarrhoea) falsely elevates hemoglobin through haemoconcentration. Conversely, excessive fluid intake causes haemodilution and a falsely low result.
Normal Hemoglobin in Adults: Men and Women
Adult reference ranges are well established. Minor differences between laboratories are possible, but the overall picture is consistent.
| Category | Normal (g/L) | Normal (g/dL) |
|---|---|---|
| Men 18–64 years | 130–174 | 13.0–17.4 |
| Men 65 years and older | 126–174 | 12.6–17.4 |
| Women 18–49 years | 117–155 | 11.7–15.5 |
| Women 50 years and older | 117–161 | 11.7–16.1 |
The lower limit of normal is the key practical threshold: it is at this point that an anaemia diagnosis is made. For men, the anaemia cut-off is below 130 g/L; for non-pregnant women, below 120 g/L (WHO criteria).
The upper limit matters too: values above 174 g/L in men or above 161 g/L in women require investigation — polycythaemia, chronic hypoxia, or dehydration.
In older men, the lower limit is slightly reduced — physiologically related to declining testosterone and erythropoietin levels with age. A hemoglobin of 126–130 g/L in an older man is not automatically pathological, but warrants monitoring.
Normal Hemoglobin in Children: Table by Age
Children's reference ranges differ substantially from adults and change throughout the growth period. Adult references must never be applied to children's results.
| Age | Normal (g/L) |
|---|---|
| Newborns (1–3 days) | 145–225 |
| 1 week | 135–215 |
| 1 month | 100–180 |
| 2–3 months | 90–135 |
| 6 months | 105–140 |
| 1 year | 105–140 |
| 2–6 years | 110–140 |
| 7–12 years | 115–145 |
| Boys 13–17 years | 125–165 |
| Girls 13–17 years | 112–152 |
Key points:
- Physiological anaemia of infancy — by 2–3 months hemoglobin drops to its nadir (90–110 g/L). This is normal: foetal hemoglobin breaks down while adult hemoglobin production is still ramping up. No treatment is required.
- Iron deficiency anaemia is the most common cause of low hemoglobin in children aged 6 months to 3 years (a period of rapid growth with high iron demand).
- Sex differences in adolescents emerge at puberty: boys' hemoglobin rises under the influence of testosterone; girls' hemoglobin falls with the onset of menstruation and regular blood loss.
Normal Hemoglobin in Pregnancy
Pregnancy is the one physiological state for which the WHO establishes separate, lower reference ranges for healthy women. This is not pathology — it is a normal adaptation.
| Trimester | Normal (g/L) | Anaemia defined as (g/L) |
|---|---|---|
| 1st trimester | 110–160 | < 110 |
| 2nd trimester | 105–160 | < 105 |
| 3rd trimester | 110–160 | < 110 |
The second-trimester drop reflects the peak haemodilutional effect — plasma volume reaches its maximum. By the third trimester, hemoglobin recovers slightly as red cell production accelerates.
Anaemia in pregnancy is common: the WHO estimates it affects approximately 40% of pregnant women worldwide. Even mild anaemia is associated with an increased risk of preterm birth, foetal growth restriction, and postpartum haemorrhage. For detailed norms and CBC interpretation during pregnancy, see complete blood count in pregnancy.
Low Hemoglobin: Grades of Anaemia and Main Causes
Anaemia is hemoglobin below the lower limit of normal for sex and age. Severity is classified by level:
| Grade | Hemoglobin (g/L) | Symptoms |
|---|---|---|
| Mild | 90 – lower limit of normal | Often asymptomatic or mild fatigue |
| Moderate | 70–89 | Exertional breathlessness, palpitations, pallor |
| Severe | < 70 | Breathlessness at rest, tachycardia, dizziness, syncope |
| Life-threatening | < 40–50 | Heart failure, altered consciousness |
Causes of low hemoglobin by mechanism:
Insufficient red cell production:
- Iron deficiency anaemia — the most common anaemia worldwide. Ferritin is low, red cells are small (microcytosis). Full details: iron deficiency anaemia.
- Vitamin B12 or folate deficiency — megaloblastic anaemia, red cells are large (macrocytosis)
- Anaemia of chronic disease — inflammation, malignancy, chronic kidney disease
- Aplastic anaemia — bone marrow suppression
Accelerated red cell destruction (haemolysis):
- Autoimmune haemolytic anaemia
- Inherited haemolytic anaemias (sickle cell disease, thalassaemia)
- Infections (malaria)
Blood loss:
- Acute — trauma, surgery, gastrointestinal haemorrhage
- Chronic — heavy menstruation, peptic ulcer, polyps, occult bleeding
High Hemoglobin: When It Matters
Elevated hemoglobin is a less obvious concern than low, but clinically equally significant. Excess hemoglobin makes blood viscous, slowing microcirculation and raising thrombotic risk.
Physiological causes (no treatment needed):
- High-altitude residence
- Intense regular athletic training
- Dehydration — spurious haemoconcentration, normalises with rehydration
- Smoking — chronic hypoxia from carboxyhaemoglobin
Pathological causes requiring investigation:
- Polycythaemia vera — a myeloproliferative disorder with autonomous red cell overproduction. Hemoglobin > 185 g/L in men, > 165 g/L in women
- Secondary erythrocytosis — from chronic hypoxia: COPD, sleep apnoea, congenital heart defects, erythropoietin-secreting tumours
- Anabolic steroid use — pharmacological stimulation of erythropoiesis
Hemoglobin above 170 g/L in men or above 160 g/L in women warrants a GP or haematology consultation.
When Hemoglobin Deviations Require Medical Attention
A moderate hemoglobin drop with good general wellbeing calls for a scheduled appointment and workup. Emergency situations:
- Hemoglobin below 70 g/L — regardless of symptoms
- Rapid drop of 20 g/L or more in a short period — suspected acute bleeding or haemolysis
- Low hemoglobin with black stools or blood in faeces — possible gastrointestinal haemorrhage
- Breathlessness and palpitations at rest alongside low hemoglobin
- Hemoglobin above 185 g/L in men or above 165 g/L in women — rule out polycythaemia
- Anaemia in a child not responding to iron therapy after 4–6 weeks
- Hemoglobin below 100 g/L in pregnancy — urgent obstetric review
This content is for informational purposes only and does not replace professional medical advice.
Frequently Asked Questions
The normal hemoglobin range for women of reproductive age (18–49) is 117–155 g/L. After age 50 the upper limit rises slightly to 161 g/L. In pregnancy, lower limits apply: a drop to 105 g/L in the second trimester is acceptable. A value below 120 g/L in a non-pregnant woman (WHO criteria) constitutes anaemia and requires identifying the cause — most often iron deficiency from heavy menstruation.
The difference is driven by testosterone. The male sex hormone stimulates erythropoietin production — a kidney hormone that triggers red cell synthesis in the bone marrow. As a result, men have more red cells and higher hemoglobin. The gap is roughly 10–20 g/L. After age 65, with the age-related decline in testosterone, the gap narrows, although men's reference ranges remain higher.
Hemoglobin below normal means anaemia — a reduction in the blood's oxygen-carrying capacity. Severity is determined by the level: mild — 90 g/L to the lower reference limit; moderate — 70–89 g/L; severe — below 70 g/L. The causes are numerous: most commonly iron deficiency, less often vitamin deficiencies, chronic disease, or blood loss. For what to do when hemoglobin is low, see low hemoglobin.
Yes. Dehydration (heat, vomiting, diarrhoea) concentrates the blood — hemoglobin appears higher than it really is. Excessive fluid intake or intravenous fluids dilute the blood — hemoglobin appears lower. Smoking elevates it via carboxyhaemoglobin. This is why the test is performed under standard conditions: fasting, without excessive fluid intake the evening before, and without intense recent exercise.
This is the key pair for identifying the cause of anaemia. When hemoglobin is low, a doctor always checks MCV — mean corpuscular volume. Small red cells (MCV < 80 fL, microcytosis) with low hemoglobin point to iron deficiency or thalassaemia. Large red cells (MCV > 100 fL, macrocytosis) suggest vitamin B12 or folate deficiency. Normal MCV with anaemia — anaemia of chronic disease, haemolysis, or acute blood loss.
Only when iron deficiency is confirmed — meaning low ferritin or reduced transferrin saturation. Taking iron for anaemia of another type (B12 deficiency, haemolysis, anaemia of chronic disease) is either ineffective or harmful. For a correct prescription, a doctor evaluates the iron panel alongside hemoglobin. Self-prescribing iron supplements without an established cause of anaemia is a common and potentially dangerous mistake.
Upload your lab results photo or PDF
AI explains your results in 30 seconds
Choose fileRate the service
Your feedback helps us improve the service