Complete Blood Count in Pregnancy: Normal Ranges by Trimester
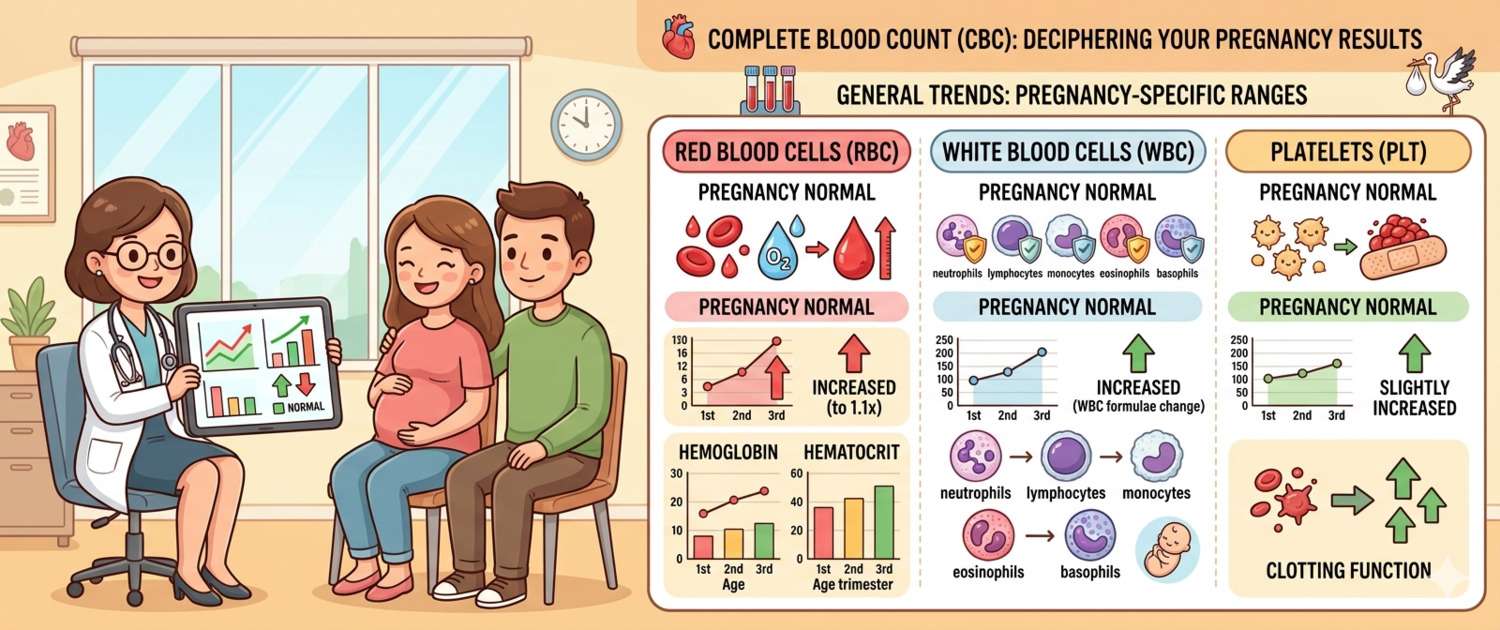
A blood test during pregnancy is one of the most common sources of anxiety. "Haemoglobin is low," "WBC is elevated" — and the woman leaves the clinic worried for no good reason. But pregnancy fundamentally changes blood composition, and most of these apparent abnormalities are not disease — they are normal physiology. The key is knowing where the boundary lies between physiological adaptation and something that genuinely needs treatment. Let's go through the complete blood count in pregnancy trimester by trimester.
The Central Phenomenon: Haemodilution
Pregnancy is a state of controlled blood "dilution." Circulating plasma volume expands by 40–50% by the end of the second trimester, while red cell volume increases by only 20–30%. As a result, all "red" parameters — haemoglobin, haematocrit, red cell count — fall relative to non-pregnant norms. This is called physiological haemodilution.
Haemodilution is not accidental. It reduces blood viscosity, improves uteroplacental blood flow, and protects against thrombosis. The body deliberately "dilutes" blood for the benefit of the fetus.
The practical implication: CBC norms in pregnancy are lower than usual, and that is correct. Comparing a pregnant woman's result to non-pregnant reference ranges is inappropriate.
Haemoglobin in Pregnancy: Normal Ranges by Trimester
| Trimester | Normal haemoglobin (g/L) | Mild anaemia | Moderate anaemia |
|---|---|---|---|
| I (1–13 wk) | 110–160 | 100–109 | 70–99 |
| II (14–27 wk) | 105–155 | 100–104 | 70–99 |
| III (28–40 wk) | 100–155 | 100–104 | 70–99 |
The lowest haemoglobin is expected in the second trimester — that is when haemodilution peaks. After 30 weeks plasma volume stabilizes and haemoglobin partially recovers.
Physiological fall vs true anaemia
The key clinical question: how to distinguish normal haemodilution from iron deficiency anaemia that genuinely requires treatment?
Haemoglobin alone does not answer this. Ferritin is needed:
- Ferritin ≥ 30 µg/L — iron stores are adequate; the haemoglobin fall is physiological dilution.
- Ferritin < 30 µg/L — iron deficiency exists, even if haemoglobin is still within the pregnant-women range.
- Ferritin < 12 µg/L — significant deficiency; iron supplementation is required.
Iron deficiency anaemia of pregnancy is the most common cause of true anaemia during pregnancy. Iron requirements in the second and third trimester rise to 27 mg/day (versus 18 mg outside pregnancy). Without supplementation, most women cannot meet this demand.
MCV: A Useful Additional Marker
MCV helps differentiate types of anaemia:
- Low MCV (< 80 fL) — microcytic anaemia → rule out iron deficiency first
- Normal MCV — dilutional anaemia or mixed
- High MCV (> 100 fL) — macrocytic anaemia → B12 or folate deficiency; during pregnancy folate is especially important for neural tube defect prevention
WBC in Pregnancy: Physiological Leukocytosis
WBC rises predictably during pregnancy — this is not a sign of infection.
| Period | Normal WBC (×10⁹/L) |
|---|---|
| Non-pregnant | 4.0–9.0 |
| 1st trimester | 6.0–12.0 |
| 2nd trimester | 7.0–14.0 |
| 3rd trimester | 8.0–15.0 |
| Labour and first 24 hours postpartum | up to 25–30 |
Mechanism: oestrogen and cortisol stimulate neutrophil release from bone marrow — an evolutionary protective response. WBC of 10–14×10⁹/L in the second and third trimester is normal.
Signs of pathological leukocytosis requiring attention: WBC above 15–16×10⁹/L in the first trimester, or a sudden spike with fever and other symptoms; left shift (band neutrophils > 6–10%); elevated C-reactive protein — that is an inflammatory response, not physiology.
Platelets in Pregnancy: Gestational Thrombocytopenia
In 5–8% of pregnant women, platelets fall to 100–150×10⁹/L without any underlying pathology — this is gestational thrombocytopenia. Mechanism: accelerated platelet destruction in the placenta plus haemodilution.
| Platelet level | Interpretation |
|---|---|
| 150–400 × 10⁹/L | Normal |
| 100–149 × 10⁹/L | Mild thrombocytopenia — most often gestational |
| 70–99 × 10⁹/L | Cause requires clarification |
| < 70 × 10⁹/L | Urgent haematology consultation |
Gestational thrombocytopenia: appears in the third trimester, is not accompanied by bleeding, and resolves spontaneously after delivery. It must be distinguished from HELLP syndrome (thrombocytopenia + liver dysfunction + haemolysis) and immune thrombocytopenia — both require active treatment.
Other Parameters: What Else Matters in Pregnancy
ESR physiologically accelerates during pregnancy — up to 40–50 mm/h in the third trimester. Using ESR as an inflammation marker in pregnancy is essentially impossible — the baseline is too high.
Reticulocytes — if anaemia is worsening, the doctor may order reticulocytes to assess erythropoiesis activity. A normal level in dilutional anaemia; reduced in true deficiency states.
HbA1c and glucose — gestational diabetes screening is mandatory during pregnancy. HbA1c is less informative in pregnancy due to accelerated red cell turnover — the oral glucose tolerance test is preferred.
When Falling Haemoglobin in Pregnancy Is Dangerous
Anaemia in pregnancy is not merely discomfort. Severe anaemia (haemoglobin < 70 g/L) increases the risk of: preterm birth; low birth weight; postpartum haemorrhage; impaired neonatal neurological development.
Moderate anaemia (70–99 g/L) in pregnancy is treated with oral iron — generally effective. Severe anaemia or intolerance of oral preparations is an indication for intravenous iron.
When to Seek Urgent Medical Attention
Immediately: haemoglobin below 70 g/L; platelets below 70×10⁹/L; WBC above 16×10⁹/L with fever and pain; combination of thrombocytopenia + jaundice + right upper quadrant pain — possible HELLP syndrome.
Within a few days: protein in urine + elevated blood pressure — rule out preeclampsia; haemoglobin below 100 g/L at the first first-trimester test — check ferritin immediately; platelets below 100×10⁹/L in the first or second trimester — cause requires clarification.
Summary
A CBC in pregnancy is a separate language with separate norms. Haemodilution lowers haemoglobin, pregnancy raises WBC, and the placenta "consumes" platelets — all of this is physiology. The fundamental question is always: adaptation or disease? The answer comes from ferritin for anaemia, differential count and CRP for leukocytosis, and clinical picture for thrombocytopenia. Have a complete blood count done each trimester and discuss results with your obstetrician — do not interpret them on your own.
This article is for informational purposes only. Interpretation of test results and treatment decisions are the responsibility of a physician.
Frequently Asked Questions
Normal haemoglobin in pregnancy is lower than outside it, due to physiological haemodilution. In the first trimester — 110–160 g/L; second — 105–155 g/L; third — 100–155 g/L. The minimum acceptable level without an anaemia diagnosis is 100 g/L. Comparing to non-pregnant norms (120–155 g/L) leads to over-diagnosis.
By checking ferritin. In physiological haemodilution, ferritin is normal — ≥ 30 µg/L. In iron deficiency anaemia, ferritin falls below 30 µg/L, often below 12. MCV provides additional information: in iron deficiency, red cells are small (MCV < 80 fL); in haemodilution, MCV is normal.
Physiological leukocytosis is a normal response to pregnancy. Oestrogen and cortisol stimulate WBC release from bone marrow — an evolutionary defence for mother and fetus. WBC of 10–14×10⁹/L in the second and third trimester is normal. Concern arises only when WBC exceeds 15–16×10⁹/L combined with fever, pain, and a left shift in the differential.
Gestational thrombocytopenia is a physiological fall in platelets to 100–149×10⁹/L in 5–8% of pregnant women in the third trimester. It causes no bleeding, requires no treatment, and normalizes spontaneously after delivery. Dangerous thrombocytopenia is below 70×10⁹/L or combined with HELLP syndrome symptoms — that requires urgent consultation.
A complete blood count should be done at least three times: at the first antenatal visit (first trimester), at 18–20 weeks (second trimester), and at 28–30 weeks (third trimester). More frequently if abnormalities are found. Alongside the first-trimester CBC, ferritin should always be checked — iron store depletion precedes the haemoglobin fall by weeks.
Global recommendations differ. The WHO recommends prophylactic iron (60 mg/day) for all pregnant women, especially in the second and third trimester. European guidelines favour an individualised approach based on ferritin: if ferritin falls below 30 µg/L, supplementation is started. In established iron deficiency anaemia, treatment is mandatory regardless of approach.
Protein in urine during pregnancy is a separate and critically important parameter, independent of the CBC. Protein above 0.3 g/day in the second or third trimester combined with elevated blood pressure is a sign of preeclampsia — a serious condition even when haemoglobin and WBC are perfectly normal. A CBC and urinalysis are complementary, not interchangeable tests.
Upload your lab results photo or PDF
AI explains your results in 30 seconds
Choose fileRate the service
Your feedback helps us improve the service