Ovulation: What It Is, Signs and How to Track Your Cycle
Every menstrual cycle is the body's preparation for a potential pregnancy — and ovulation is the moment everything hinges on. It lasts only a matter of hours, yet conception is only possible during this narrow window. Understanding when ovulation occurs, how to recognise it, and what to do if it is disrupted is useful for every woman, whether she is trying to conceive or simply wants to understand her own cycle.
What Is Ovulation and How Does It Happen?
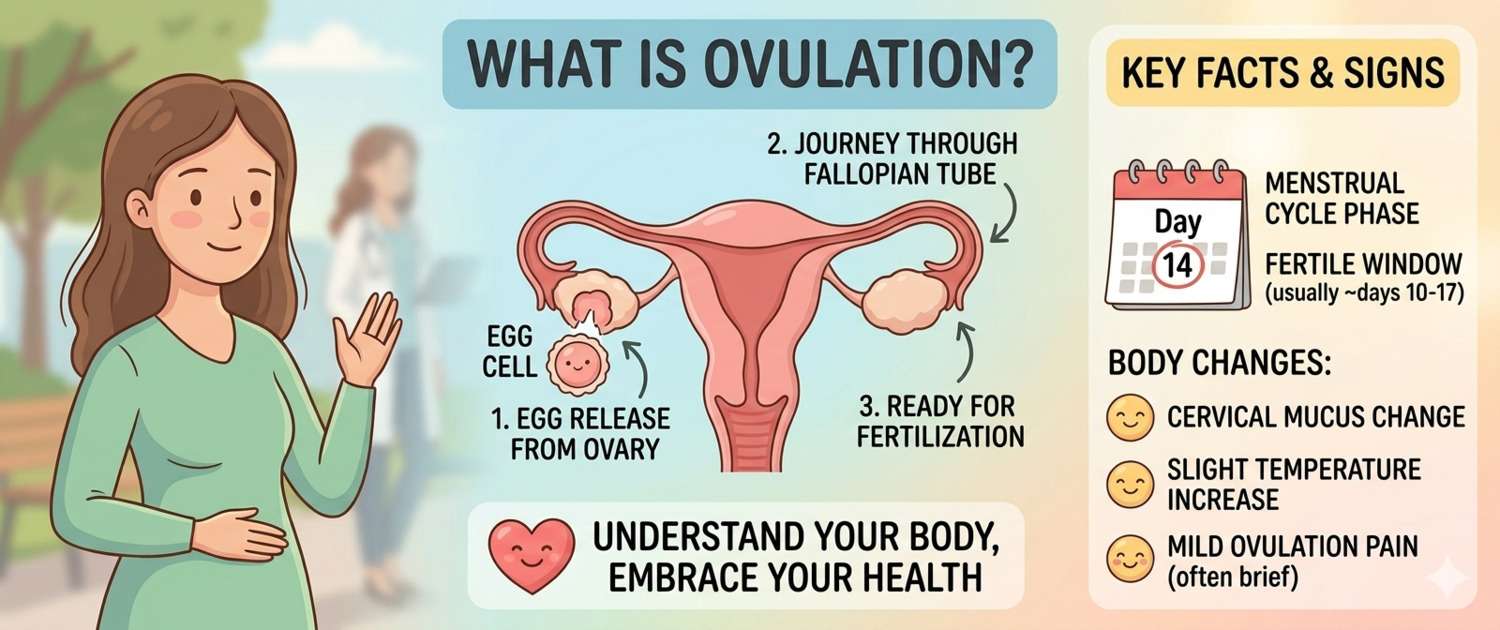
Ovulation is the release of a mature egg from an ovarian follicle into the fallopian tube. Simple in concept, it is the product of a precise hormonal sequence that resets with every cycle.
In the first half of the cycle (the follicular phase), follicle-stimulating hormone (FSH) prompts several follicles in the ovary to begin maturing. One — the dominant follicle — outpaces the rest and continues to grow. As it grows, it secretes increasing amounts of estradiol: when estradiol reaches its peak, it signals the pituitary gland to release a surge of luteinizing hormone (LH). This LH surge triggers the final maturation of the egg. Approximately 36–40 hours later, the follicle ruptures and the egg is released.
After rupture, the empty follicle transforms into the corpus luteum — a temporary gland that begins producing progesterone. Progesterone primes the endometrium for implantation. If fertilisation does not occur, the corpus luteum degenerates within 10–14 days, progesterone falls, and menstruation begins.
When Does Ovulation Occur: Calculating Your Day
The key rule: ovulation happens approximately 14 days before the next menstrual period — not 14 days after the previous one began, as is commonly assumed.
This distinction matters with irregular cycles. For a perfect 28-day cycle, both calculations give the same answer — day 14. But for a 35-day cycle, ovulation falls around day 21, not day 14.
The calculation:
- Find your average cycle length over the last 3–6 months
- Subtract 14 — that is your estimated ovulation day
For a 26-day cycle: 26 − 14 = day 12 For a 32-day cycle: 32 − 14 = day 18
This is an estimate only. Even in women with regular cycles, the actual ovulation day can shift by 1–3 days depending on stress, illness, sleep disruption, and other factors.
Signs of Ovulation: How to Recognise When It Happens
The body gives several signals around ovulation. They are not universal — some women notice none of them, while others experience them clearly.
Changes in cervical mucus — the most reliable physical sign. In the days leading up to ovulation, discharge becomes abundant, clear, and stretchy, resembling raw egg white. This consistency facilitates sperm movement. After ovulation, mucus quickly becomes thick and scant.
Mid-cycle pelvic pain (Mittelschmerz) — a dull or cramping pain on one side of the lower abdomen, lasting from a few minutes to several hours. It is caused by peritoneal irritation when the follicle ruptures. Occurs in 20–40% of women.
Increased libido — physiologically driven: the peak in estrogens and androgens around ovulation heightens sexual desire.
Mild breast tenderness — a result of the hormonal shift before and during ovulation.
Light spotting — a small amount of bloody discharge at the moment of follicular rupture. Uncommon, but a normal variant.
Rise in basal body temperature (BBT) — after ovulation, progesterone raises BBT by 0.2–0.5 °C. This is a retrospective sign: the temperature rise happens after the egg has already been released, confirming that ovulation has occurred.
How to Detect Ovulation at Home
Several methods exist, with varying accuracy and practicality.
Ovulation predictor kits (LH tests) — the most accurate home method. They detect the LH surge in urine. A positive result means ovulation is expected within 24–36 hours. Testing should begin 4–5 days before the estimated ovulation day, twice daily — morning and midday (not the first morning urine, unlike a pregnancy test).
Basal body temperature (BBT) charting — rectal or oral temperature measured every morning before getting up. After ovulation, temperature rises and stays elevated until menstruation. The method requires consistency across at least 3 cycles to identify a pattern and is unreliable with disrupted sleep, fever, or anti-inflammatory medication.
Cervical mucus method (Billings method) — observing the character of vaginal discharge. It requires practice but has reasonable accuracy when applied correctly.
Ultrasound folliculometry — the gold standard for medical purposes. A series of ultrasounds tracks the dominant follicle's growth and the moment of rupture. Ordered when planning pregnancy, treating infertility, or monitoring ovulation induction.
Cycle-tracking apps are useful as supplementary tools but should not be relied upon for conception planning: they calculate from an algorithm, not from actual hormone measurements.
How Long Ovulation Lasts and What the Fertile Window Means
The actual release of the egg takes only a few minutes. The egg survives 12–24 hours after release — 48 hours at most. That sounds like a very narrow target.
But sperm can survive in favorable cervical mucus for up to 5 days. This is why the fertile window — the period when conception is possible — spans approximately 6 days: the five days before ovulation and one day after.
This explains why unprotected sex several days before ovulation can be just as effective as sex on the day of egg release itself. For more on what happens in the body after successful fertilisation, see first signs of pregnancy.
Ovulation with an Irregular Cycle
An irregular cycle — varying by more than 7–8 days from month to month — makes calendar prediction unreliable. If your cycle ranges from 24 to 38 days, the ovulation date shifts accordingly, and the simple "minus 14" formula falls short.
In these cases, LH tests or folliculometry are far more practical. Testing should begin earlier — from day 8–10 of the cycle — and continue for longer.
It is important to distinguish an irregular but ovulatory cycle from a cycle with no ovulation at all. With an irregular ovulatory cycle, periods still come, however unpredictably. With an anovulatory cycle, menstruation may arrive on schedule — but the follicle never ruptured, no egg was released, and conception was impossible that month.
Ovulation Disorders: Causes and Contributing Factors
Absent or infrequent ovulation is one of the leading causes of female infertility. The causes are varied.
Polycystic ovary syndrome (PCOS) — the most common cause of chronic anovulation. Multiple small follicles develop but none becomes dominant. Accompanied by menstrual irregularity, elevated androgens, and often insulin resistance.
Thyroid dysfunction — both hypothyroidism and hyperthyroidism interfere with sex hormone synthesis and can suppress ovulation. TSH is part of the standard hormonal workup for cycle irregularities.
Hyperprolactinemia — elevated prolactin inhibits FSH and LH secretion, which are required for follicle maturation. Often accompanied by nipple discharge outside of pregnancy or breastfeeding. For more on this hormone and its causes: prolactin: what is this hormone.
Significant weight loss and low body weight — adipose tissue participates in estrogen synthesis. At a BMI below 17–18 kg/m², the hypothalamus reduces gonadotropin output and ovulation ceases. The same occurs in eating disorders.
Intense athletic training — female athletes with high training loads and low body fat percentage frequently develop the "female athlete triad": anovulation, osteoporosis, and energy deficiency.
Chronic stress — cortisol suppresses pulsatile GnRH secretion, disrupting the entire hormonal axis. A single stressful event can delay ovulation by a few days; chronic stress can cause prolonged cycle disruption.
Age-related decline in ovarian reserve — after age 35–37, the quantity and quality of follicles progressively decreases, and anovulatory cycles become increasingly frequent.
When to See a Doctor
Most women do not track ovulation routinely — and that is perfectly normal. But several situations call for a consultation with a gynaecologist or reproductive specialist:
- Cycles consistently shorter than 21 or longer than 38 days over 3 or more months
- Absence of menstruation for more than 3 months with pregnancy ruled out
- No conception after 12 months of regular unprotected intercourse (6 months after age 35)
- Confirmed absent ovulation based on LH tests or BBT across several consecutive cycles
- Nipple discharge unrelated to pregnancy or breastfeeding
- Progressively worsening mid-cycle pain from month to month
Ovulation disorders respond well to treatment when identified early. In most cases, addressing the underlying cause — normalising weight, correcting hormone levels, or reducing training load — is sufficient.
This content is for informational purposes only and does not replace professional medical advice.
Frequently Asked Questions
In a standard 28-day cycle, ovulation typically falls on day 14 — exactly mid-cycle. However, this is an average estimate: the actual day can shift by 1–3 days in either direction due to stress, illness, or sleep disruption. For a more reliable answer, LH ovulation tests are a better tool than the calendar method alone.
The main retrospective sign is a sustained rise in basal body temperature — 0.2–0.5 °C above your pre-ovulation baseline — that holds for several days. At the same time, cervical mucus becomes thick, scant, and opaque. An LH test that was positive at the peak will be negative again within a day or two. These changes together confirm that ovulation has occurred and the luteal phase has begun.
The physical release of the egg from the follicle takes only minutes. The egg itself remains viable for 12–24 hours after release — 48 hours at most. However, because sperm can survive in cervical mucus for up to 5 days, the fertile window is approximately 6 days wide: five days before ovulation and one day after.
Yes, though it is uncommon. Dual ovulation can occur within a single cycle — but both eggs are released within 24 hours of each other, not weeks apart. This is how fraternal twins are conceived. Two separate LH surges in one cycle separated by weeks are extremely rare and should not be assumed when planning contraception.
An anovulatory cycle is one where menstruation occurs but ovulation did not — the follicle matured incompletely or failed to rupture. One or two anovulatory cycles per year are considered normal in otherwise healthy women. Frequent or persistent anovulation signals a hormonal imbalance. One common cause is elevated prolactin, which suppresses follicle maturation. Evaluation by a gynaecologist and a hormonal panel are needed to identify the cause.
A standard hormonal workup includes FSH, LH, estradiol, and progesterone — drawn on specific cycle days as directed by the doctor. Thyroid function is always evaluated (thyroid panel), along with prolactin. If PCOS is suspected, androgens and fasting insulin are added. A gynaecologist will specify the exact panel based on your history and symptoms.
Upload your lab results photo or PDF
AI explains your results in 30 seconds
Choose fileRate the service
Your feedback helps us improve the service