Total Cholesterol: Normal Levels, Causes and Treatment
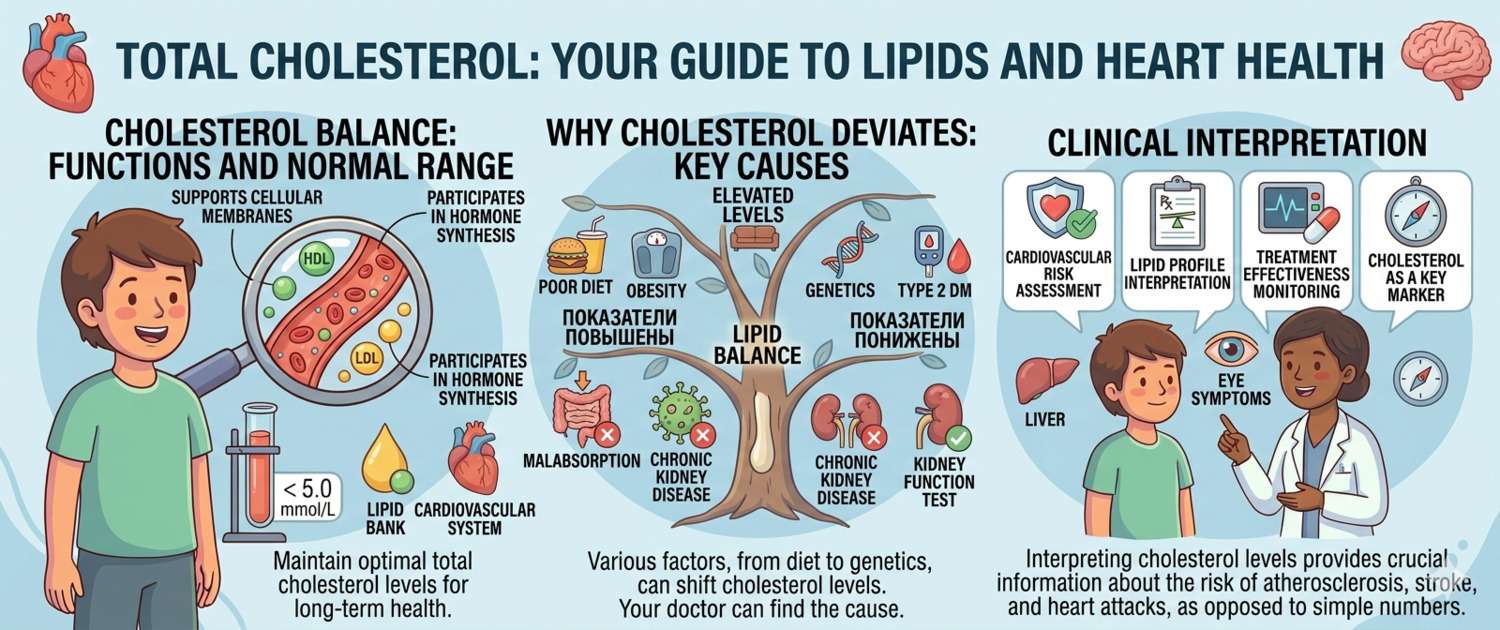
Cholesterol has earned a reputation as the enemy of arteries — largely warranted, but significantly oversimplified. In reality, cholesterol is essential: without it, the body cannot synthesize cell membranes, sex hormones, cortisol, or vitamin D. The problem is not cholesterol itself, but its excess and the form in which it circulates. Let's break down what total cholesterol measures, why it rises, and why a single number is insufficient for assessing cardiovascular risk.
What Cholesterol Is and Why the Body Needs It
Cholesterol is a fatty alcohol (sterol) found exclusively in animal tissues. Approximately 75–80% is synthesized within the body — primarily in the liver — and only 20–25% comes from food. This means that even on a strict cholesterol-free diet, the body compensates through endogenous synthesis — and conversely, when dietary cholesterol is excessive, the liver reduces its own production.
The functions of cholesterol are irreplaceable:
- Structural — a component of the phospholipid bilayer of every cell membrane, regulating its fluidity and permeability
- Hormonal — the substrate for all steroid hormone synthesis: cortisol, aldosterone, testosterone, estrogens, progesterone
- Vitamin — the precursor to vitamin D₃ synthesized in the skin under UV radiation
- Digestive — bile acids formed from cholesterol are essential for intestinal fat absorption
- Neural — a component of the myelin sheath of neurons
In blood, cholesterol circulates not in free form but within lipoproteins — protein-lipid complexes. The type of transport carrier determines whether cholesterol works against or for vascular health. LDL carries cholesterol to cells — and in excess deposits it into artery walls. HDL collects excess cholesterol from artery walls and returns it to the liver.
A lipid panel is the only way to view the complete lipid profile and assess true atherogenic risk.
Normal Total Cholesterol by Age and Sex
Total cholesterol aggregates all fractions: LDL-cholesterol, HDL-cholesterol, and VLDL-cholesterol (approximately TG/5 in mg/dL). Reference values differ by age and sex.
| Age | Men (mmol/L) | Women (mmol/L) |
|---|---|---|
| Under 18 | 2.9–5.2 | 2.9–5.2 |
| 18–30 years | 3.2–6.3 | 3.1–5.8 |
| 30–40 years | 3.4–6.9 | 3.4–6.3 |
| 40–50 years | 3.8–7.1 | 3.8–6.9 |
| 50–60 years | 4.1–7.2 | 4.2–7.4 |
| Over 60 years | 4.0–7.2 | 4.4–7.7 |
Clinically relevant thresholds (for all adults):
| Level (mmol/L) | Category |
|---|---|
| < 5.2 | Desirable |
| 5.2–6.2 | Borderline high |
| 6.2–7.8 | High |
| > 7.8 | Very high |
Premenopausal women have lower cholesterol than men of the same age — estrogens stimulate hepatic HDL receptors. After menopause, LDL rises, and by age 60–70 total cholesterol in women frequently exceeds that in men.
Pregnancy physiologically raises total cholesterol 1.5–2-fold — especially in the second and third trimesters. This is normal and requires no correction.
Critical point: total cholesterol is a crude summary figure. Two people with identical total cholesterol of 6.5 mmol/L may have fundamentally different risk profiles: one driven by high HDL and normal LDL, the other by high LDL and low HDL. Clinical decisions always require a complete lipid panel.
How to Prepare for a Cholesterol Blood Test
Cholesterol is tested as part of the lipid panel and requires standard preparation for the full profile.
- Strictly fasting — at least 12 hours. Food intake has minimal effect on total cholesterol itself (unlike triglycerides), but fasting is necessary for accurate Friedewald LDL calculation
- No alcohol for 48–72 hours — alcohol raises triglycerides and affects calculated LDL
- Stable diet for 2–3 weeks — a drastic dietary change before the test produces an unrepresentative result
- Acute illness and myocardial infarction reduce cholesterol by 10–40% — postpone testing 6–8 weeks after recovery
- For serial monitoring — same laboratory, identical conditions
- Disclose all medications: statins, fibrates, estrogens, glucocorticoids, antipsychotics — all significantly affect cholesterol levels
Causes of High Cholesterol (Hypercholesterolemia)
Hypercholesterolemia is the most common lipid disorder worldwide, affecting over 40% of adults. Causes divide into primary (genetic) and secondary (acquired).
Primary (genetic) causes:
| Condition | Cholesterol level | Features |
|---|---|---|
| Familial hypercholesterolemia (heterozygous) | 7–12 mmol/L | 1 in 250–500 people; tendon xanthomas |
| Familial hypercholesterolemia (homozygous) | 15–30 mmol/L | 1 in 300,000; MI in childhood |
| Polygenic hypercholesterolemia | 6–8 mmol/L | Most common form |
| Familial combined hyperlipidemia | Variable | LDL↑ + TG↑ |
Secondary (acquired) causes:
| Cause | Mechanism | How to identify |
|---|---|---|
| Hypothyroidism | Reduced LDL receptor activity | Elevated TSH |
| Type 2 diabetes | Insulin resistance → increased VLDL synthesis | Hyperglycemia; LDL↑ + TG↑ |
| Nephrotic syndrome | Compensatory lipoprotein synthesis | Proteinuria; edema |
| Chronic kidney disease | Impaired lipoprotein catabolism | Elevated creatinine |
| Obstructive liver disease / cholestasis | Impaired biliary cholesterol excretion | Elevated ALP, GGT, bilirubin |
| Obesity | Insulin resistance → excess VLDL | Abdominal pattern; TG↑ |
| Diet high in saturated fats | Reduced LDL receptor activity | Responds to dietary change |
| Glucocorticoids, progestins, retinoids | Reduced LDL receptor activity | Link to medication use |
| Pregnancy | Physiological increase in VLDL synthesis | Normalizes postpartum |
Causes of Low Cholesterol (Hypocholesterolemia)
Very low cholesterol (< 3.0–3.5 mmol/L) in adults is not always favorable. Cholesterol is required for steroid hormone synthesis and normal nervous system function.
Main causes:
- Severe liver disease (cirrhosis, acute hepatic failure) — reduced synthesis of all lipoproteins
- Severe starvation, cachexia, malabsorption — substrate deficiency and impaired fat absorption
- Hyperthyroidism — accelerated LDL catabolism through upregulated LDL receptors
- Chronic anemia, malignancies — cholesterol consumption by tumor cells
- Intensive statin therapy — deliberate reduction; values of 1.5–2.5 mmol/L are clinically safe
Very low cholesterol (< 2.5 mmol/L) without an identifiable cause warrants exclusion of severe liver pathology and malignant disease.
Total Cholesterol in the Lipid Profile Context
Total cholesterol is a composite figure and cannot be interpreted meaningfully without understanding its fractions. It is a starting point, not a final answer.
Atherogenicity index (AI) = (Total cholesterol − HDL) / HDL. Normal: < 3.0; borderline: 3.0–4.0; high risk: > 4.0–5.0.
With identical total cholesterol of 6.0 mmol/L:
- Patient A: HDL = 2.0 → AI = 2.0 → low risk
- Patient B: HDL = 0.8 → AI = 6.5 → very high risk
Non-HDL cholesterol = Total cholesterol − HDL. Captures LDL + VLDL + IDL — all atherogenic fractions. When triglycerides exceed 4.5 mmol/L, non-HDL cholesterol becomes the preferred therapeutic target instead of calculated LDL.
The link to atherosclerosis: excess LDL particles penetrate the subendothelial space, become oxidized, are engulfed by macrophages, and form plaques. This makes cholesterol control the central element of cardiovascular disease prevention.
How to Lower Cholesterol and When Medication Is Needed
Lifestyle changes (reduce cholesterol by 5–20%):
- Limit saturated fats (red meat, butter, coconut and palm oil, full-fat dairy) — to < 7% of daily calories
- Eliminate trans fats (industrial baked goods, margarine) — greatest impact on LDL/HDL ratio
- Increase soluble fiber: oat bran, legumes, psyllium — reduces LDL by 5–10%
- Plant sterols and stanols (2–3 g/day) — reduce LDL by 8–15%
- Regular aerobic physical activity — modestly lowers LDL and substantially raises HDL
- Weight normalization — losing 10% of body weight reduces total cholesterol by 10–20%
Pharmacological treatment:
- Statins — first line: reduce LDL by 30–55% and total cholesterol substantially
- Ezetimibe — blocks intestinal cholesterol absorption; reduces LDL by an additional 15–20% in combination with statins
- PCSK9 inhibitors — for familial hypercholesterolemia and statin-intolerant patients; reduce LDL by 50–65%
The decision to start medication is based not on total cholesterol alone, but on overall cardiovascular risk — accounting for age, sex, blood pressure, smoking, diabetes, and family history. After a heart attack or stroke, statins are prescribed lifelong regardless of cholesterol level.
For the extended lipid profile, the role of ApoB and longevity-optimal cholesterol levels, see the article extended lipid profile and longevity.
This article is for informational purposes only and does not replace professional medical advice. If you have high cholesterol, consult a cardiologist or GP.
Frequently Asked Questions
Partly. Eggs are rich in dietary cholesterol (~186 mg per yolk), but the impact of dietary cholesterol on blood cholesterol is substantially smaller than that of saturated and trans fats. In most people, moderate egg consumption (up to 6–7 per week) does not raise cardiovascular risk. Exceptions include people with familial hypercholesterolemia and hyper-responders. After a myocardial infarction, limiting intake to 3–4 eggs per week is a reasonable precaution.
Yes. Cholesterol is required for steroid hormone synthesis, vitamin D production, bile acid formation, and myelin integrity. Very low cholesterol (< 2.5–3.0 mmol/L) without an identifiable cause signals possible serious pathology: hepatic failure, cachexia, severe hyperthyroidism, or malignancy. Medically targeted reduction to 1.5–2.0 mmol/L during statin therapy is well-documented as safe.
Because it sums both harmful (LDL) and protective (HDL) cholesterol. High HDL raises total cholesterol — but reduces risk. Low HDL lowers total cholesterol — but increases risk. The same value of 6.0 mmol/L can represent low or very high atherogenic potential depending on the fractions. Clinical guidelines require a complete lipid panel with LDL, HDL, and triglycerides before any therapeutic decision.
It depends on overall cardiovascular risk. At 5.5–6.0 mmol/L in a young person without risk factors, lifestyle modification is the primary step. It is important to also evaluate LDL, HDL, and blood glucose: together they determine whether additional intervention is needed.
Yes, and substantially so. Familial hypercholesterolemia (FH) is one of the most common monogenic disorders — the heterozygous form affects 1 in 250–500 people. In FH, LDL receptors are defective or absent — the liver cannot clear LDL from blood, and levels build from birth. Without treatment, men with FH experience a heart attack by age 40–50, women by 50–60. Diagnostic features: cholesterol > 7–8 mmol/L, family history of premature myocardial infarction, and tendon xanthomas.
When overall cardiovascular risk is low. A young person (under 40) without diabetes, hypertension, or smoking, with total cholesterol of 6.0–7.0 mmol/L and normal LDL/HDL ratios, is a candidate for lifestyle change — not immediate statin therapy. The decision is made using a global risk score (SCORE, PCE). However, after a myocardial infarction, in diabetes with organ damage, or in familial hypercholesterolemia — statins are prescribed regardless of the absolute cholesterol value.
Upload your lab results photo or PDF
AI explains your results in 30 seconds
Choose fileRate the service
Your feedback helps us improve the service