Homocysteine: Normal Levels, Interpretation and Cardiovascular Risk
Homocysteine is an amino acid not found in food. It forms inside cells during methionine breakdown and is normally recycled immediately. When this cycle is disrupted — through vitamin deficiency or genetics — homocysteine accumulates in the blood and becomes a silent threat to vessels and the brain.
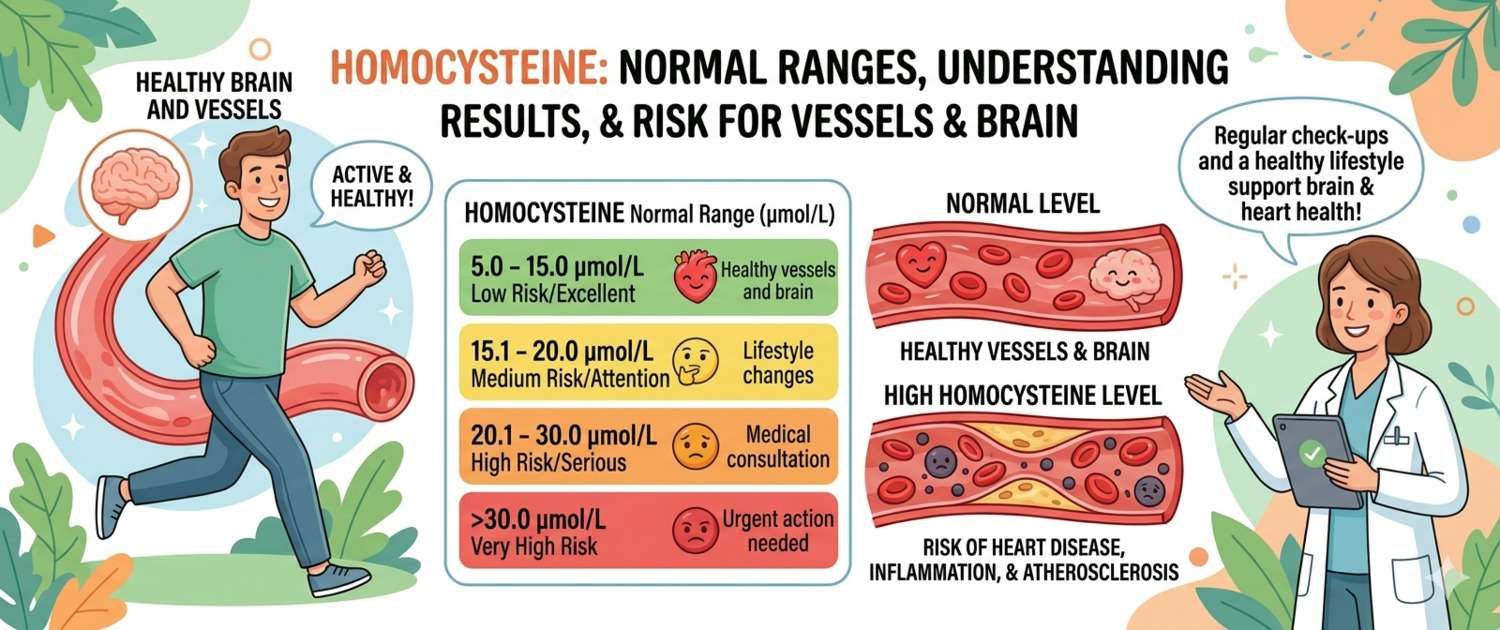
Interpreting homocysteine results requires different reference points than those printed on most lab reports. The standard "normal up to 15 µmol/L" represents a threshold for overt risk — not a longevity target. For optimal health, aim for under 8–9 µmol/L.
What Is Homocysteine and Where Does It Come From
Homocysteine is an intermediate in sulphur amino acid metabolism. The cycle: methionine (from meat, eggs, dairy) → homocysteine → back to methionine or cysteine. Three cofactors drive this conversion: vitamin B12, folate (B9) and vitamin B6.
If any cofactor is deficient, homocysteine cannot be cleared and accumulates. This is the basis of treatment: supply the missing vitamin, and homocysteine normalises within 8–12 weeks.
An additional factor: MTHFR mutation (methylenetetrahydrofolate reductase). This enzyme converts folate to its active form — 5-methyltetrahydrofolate. The C677T variant reduces MTHFR activity by 35–70%, impairing homocysteine clearance even when dietary vitamin intake is adequate.
Homocysteine Normal Ranges: Clinical vs Longevity Optimal
Lab reference ranges: 5–15 µmol/L. For preventive medicine and biological age assessment, stricter thresholds apply:
| Homocysteine Level | Interpretation |
|---|---|
| < 8 µmol/L | Longevity optimum |
| 8–10 µmol/L | Acceptable range |
| 10–15 µmol/L | Mild hyperhomocysteinaemia |
| 15–30 µmol/L | Moderate-high risk |
| > 30 µmol/L | Severe hyperhomocysteinaemia |
Note: men average 1–2 µmol/L higher than women. After menopause, women's homocysteine rises towards male levels.
Homocysteine and Vascular Risk: Research Evidence
The Homocysteine Studies Collaboration meta-analysis (2002, 30 prospective studies): each 5 µmol/L increase in homocysteine is associated with a 20% higher coronary heart disease risk and a 59% higher stroke risk.
The mechanism of vascular damage operates on three levels:
- Oxidative stress: homocysteine auto-oxidises → hydrogen peroxide and free radicals → endothelial injury
- Inflammation: elevated homocysteine raises C-reactive protein and pro-inflammatory cytokines
- Coagulation: homocysteine reduces prostacyclin activity and enhances platelet adhesion
The combination of high homocysteine with elevated fasting insulin and an impaired lipid panel multiplies cardiovascular risk. Homocysteine is a core marker in the metabolic cluster for biological ageing assessment.
Homocysteine and Brain Health
Framingham Heart Study (Seshadri et al., 2002, 1,092 participants): each 5 µmol/L increase in homocysteine raises Alzheimer's risk by 40%. Homocysteine above 14 µmol/L doubles dementia risk.
Mechanism: homocysteine crosses the blood-brain barrier, stimulates NMDA receptors causing neuronal excitotoxicity, disrupts neuronal DNA methylation and increases oxidative stress in the brain.
The Oxford Project to Investigate Memory and Ageing (OPTIMA): in patients with mild cognitive impairment and elevated homocysteine, B12 + folate + B6 supplementation slowed brain atrophy by 30–50% over two years on MRI.
For brain health, many neurologists target homocysteine below 7–8 µmol/L for neurodegeneration prevention.
Causes of Elevation: B12, Folate, B6 and MTHFR Mutation
Vitamin B12 deficiency — the most common cause in adults over 50. Vitamin B12 is essential for remethylation of homocysteine back to methionine. Gastritis, proton pump inhibitors, and vegan diets all reduce B12 absorption.
Folate (B9) deficiency — folate is the second key cofactor. Low green vegetable intake, methotrexate use, or oral contraceptives deplete folate and raise homocysteine.
Vitamin B6 deficiency — B6 is required for the alternative transsulphuration pathway converting homocysteine to cystathionine. B6 becomes critical when homocysteine exceeds 20 µmol/L.
MTHFR C677T mutation — homozygous carriers (5–10% of the population) have MTHFR working at 30–65% efficiency. Standard folic acid is insufficient here — methylated folate (5-MTHF, methylfolate) is required.
Other causes: chronic kidney disease (impaired excretion), hypothyroidism, smoking, excess alcohol, and certain medications (metformin, trimethoprim).
How to Lower Homocysteine in 12 Weeks: Protocol
Step 1 — Core protocol for everyone:
- Vitamin B12 (methylcobalamin): 1000 µg/day sublingually — or intramuscularly if malabsorption is suspected
- Methylfolate (5-MTHF): 400–800 µg/day — essential for MTHFR carriers
- Vitamin B6 (P5P form): 20–25 mg/day
Step 2 — When homocysteine exceeds 15 µmol/L:
- Betaine (trimethylglycine): 1000–3000 mg/day — an alternative methyl donor that bypasses MTHFR entirely
- Increase methylfolate to 1000–2000 µg/day
Expected results:
- 8 weeks: average 25–35% reduction
- 12 weeks: normalisation in 80–90% of people without severe renal impairment
Dietary measures: increase green leafy vegetables (spinach, rocket, Brussels sprouts — natural folate sources), reduce alcohol and excess coffee (both increase B-vitamin excretion).
Who Should Test and How Often
Primary screening: everyone over 35 at a preventive check-up. Priority cases: family history of early heart attack or stroke, chronic kidney disease, cognitive complaints, known MTHFR mutation.
Panel: homocysteine + vitamin B12 + folate — the baseline triad. If elevated, add vitamin B6 and MTHFR genotyping.
Frequency: with optimal values (< 9 µmol/L) — once yearly as part of the annual blood test checklist. With values of 10–15 — retest after 3 months of B-vitamin supplementation.
Homocysteine is part of the "inflammatory quartet" for biological age assessment alongside hs-CRP, fasting insulin and HbA1c. The full monitoring system is described in how to live longer: the evidence base.
Frequently Asked Questions
Risk begins at homocysteine above 10 µmol/L. Above 15, cardiovascular risk is meaningfully elevated — comparable to moderate LDL elevation. Above 20, the risk is high. The lab normal of 'up to 15' is the threshold for overt hyperhomocysteinaemia, not an optimal target. For longevity, aim for under 8–9 µmol/L.
Possible reasons: you are taking cyanocobalamin rather than methylcobalamin — the latter is better absorbed and utilised. Or you have an MTHFR mutation requiring methylfolate (5-MTHF) in addition. Or B6 is deficient. Homocysteine often only normalises when all three cofactors — B12, folate and B6 — are taken together. If it remains high, add betaine 1–3 g/day.
Not necessarily at first. If homocysteine exceeds 12–15 µmol/L and responds poorly to the standard B12 + B9 + B6 protocol, MTHFR C677T genotyping helps identify whether methylated folate is needed. If homocysteine normalises on standard supplements, genotyping loses its practical value.
Yes, the association is well documented. The Framingham Heart Study showed that homocysteine above 14 µmol/L doubles Alzheimer's risk. The OPTIMA trial showed that lowering homocysteine with B-vitamins slowed brain atrophy on MRI by 30–50% in patients with mild cognitive impairment. For brain health, target homocysteine below 7–8 µmol/L.
Core panel: homocysteine + vitamin B12 + folate. If elevated, add B6. For complete vascular risk assessment, add hs-CRP and a lipid panel. Homocysteine, CRP and fasting insulin together form the minimal panel for biological age assessment — each marker capturing a different dimension of the same ageing process.
With a correctly chosen protocol (B12 + methylfolate + B6), a reduction is visible within 4–6 weeks and normalisation occurs within 8–12 weeks in 80–90% of people without severe renal impairment. With MTHFR mutation or kidney disease, the process may take longer. A control test is recommended 3 months after starting supplementation.
Upload your lab results photo or PDF
AI explains your results in 30 seconds
Choose fileRate the service
Your feedback helps us improve the service