Liver Cirrhosis: Symptoms, Stages, Lab Tests and Treatment
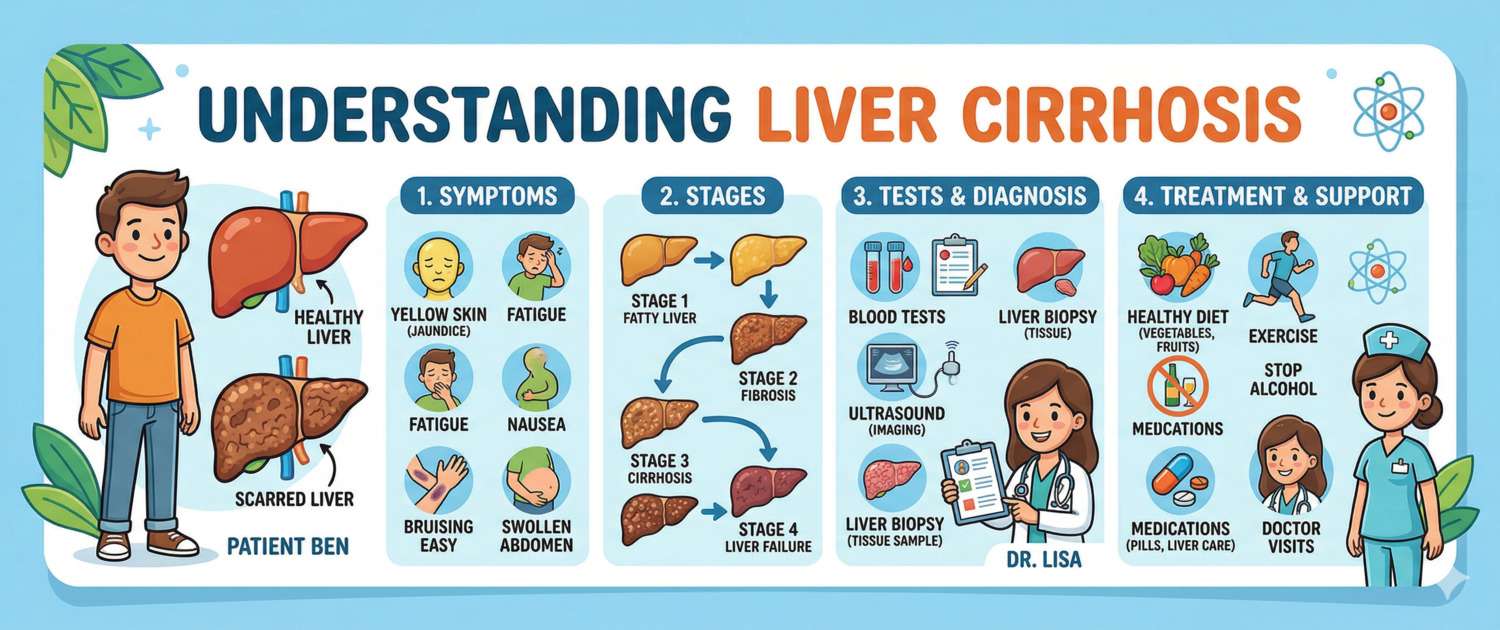
Cirrhosis is not a disease in the conventional sense — it is the end point of many liver diseases. When healthy liver tissue is replaced by scar tissue, the organ loses its ability to synthesize proteins, detoxify waste, and regulate blood clotting. The insidious nature of cirrhosis is that it can remain silent for years — and then present in a stage of decompensation, when reserves are already exhausted.
What Cirrhosis Is and How It Forms
Liver cirrhosis is a chronic diffuse disease in which the normal architecture of hepatic tissue is irreversibly replaced by fibrotic (scar) tissue with the formation of pseudonodules. It is the final stage of any chronic liver injury, regardless of its cause.
The underlying mechanism is universal. Any hepatocyte injury — whether from alcohol, viruses, fatty change, or autoimmune processes — activates hepatic stellate cells (Ito cells). These begin synthesising collagen, forming fibrous bands. Normal lobules become encircled by scar tissue; blood flow through the sinusoids is disrupted; pressure rises in the portal venous system — portal hypertension develops.
The defining property of cirrhosis: fibrosis is irreversible. Treatment can halt progression but cannot remove established scar tissue. This is precisely why early diagnosis and elimination of the underlying cause are so critical.
Causes of Cirrhosis
Any chronic liver disease left untreated can lead to cirrhosis. The most common causes:
Alcoholic cirrhosis — the leading cause in most developed countries. Daily consumption of > 40–60 g pure ethanol in men and > 20–40 g in women over 10–20 years leads to cirrhosis in 15–20% of heavy drinkers. Women are more vulnerable at equivalent intake levels.
Viral hepatitis — chronic hepatitis B and C without treatment progress to cirrhosis in 20–30% of patients over 20–30 years. Chronic hepatitis is the most important precursor to cirrhosis.
Non-alcoholic fatty liver disease (NAFLD/NASH) — a rapidly growing cause driven by the global epidemic of obesity and metabolic syndrome.
Autoimmune liver diseases — primary biliary cholangitis, primary sclerosing cholangitis, autoimmune hepatitis.
Genetic disorders — haemochromatosis (iron overload), Wilson's disease (copper overload), alpha-1 antitrypsin deficiency.
Drug-induced hepatitis — prolonged use of hepatotoxic agents (methotrexate, amiodarone).
Stages of Cirrhosis: Compensated and Decompensated
Clinically, cirrhosis divides into two fundamentally different states.
Compensated cirrhosis (Child-Pugh class A): scar tissue is present, but the remaining hepatocytes manage to maintain function. The patient may have no symptoms for years. Often discovered incidentally on ultrasound or blood tests. Prognosis: 10-year survival > 80%.
Decompensated cirrhosis (classes B and C): functional reserve is exhausted. Life-threatening complications develop. Prognosis worsens sharply: without transplantation, 5-year survival in class C is approximately 20%.
The Child-Pugh score evaluates 5 parameters (1–3 points each): bilirubin, albumin, prothrombin time, presence of ascites, and degree of encephalopathy.
| Class | Score | Characterisation | 1-year survival |
|---|---|---|---|
| A | 5–6 | Compensated | 100% |
| B | 7–9 | Moderate decompensation | 80% |
| C | 10–15 | Severe decompensation | 45% |
Symptoms of Cirrhosis by Stage
Compensated stage: often asymptomatic. Possible non-specific complaints — fatigue, right upper quadrant heaviness, reduced appetite, bloating. Physical findings: mild hepatomegaly or a shrunken liver (in advanced disease), "liver signs" — spider angiomata, palmar erythema, leukonychia.
Decompensated stage — four major complications:
Ascites — fluid accumulation in the peritoneal cavity due to portal hypertension and reduced oncotic pressure (from low albumin). The first manifestation of decompensation in most patients. Tense ascites causes dyspnoea and abdominal pain.
Variceal haemorrhage — dilation of oesophageal and gastric veins from portal hypertension. Bleeding from varices is the most dangerous complication of cirrhosis, with mortality of 15–20% per episode.
Hepatic encephalopathy — impaired brain function due to the accumulation of toxins (primarily ammonia) that the damaged liver cannot neutralise. Ranges from mild forgetfulness and personality change to coma.
Spontaneous bacterial peritonitis (SBP) — infection of ascitic fluid without an obvious external source. Mortality without treatment exceeds 50%.
Additionally: jaundice (impaired bilirubin excretion), bleeding tendency (reduced clotting factor synthesis), muscle wasting (sarcopenia), hepatorenal syndrome.
Liver Cirrhosis Blood Tests: What and Why
The laboratory picture of cirrhosis reflects the loss of the liver's synthetic and detoxifying functions. Key markers:
Synthetic function:
- Albumin — falls as cirrhosis progresses: < 35 g/L indicates moderate insufficiency; < 28 g/L indicates severe insufficiency
- Total protein — falls in parallel with albumin
- Prothrombin time (PT) / INR — prolonged; the liver cannot synthesise adequate clotting factors
Metabolic function:
- Bilirubin — rises during decompensation
- Urea — falls in severe cirrhosis (ornithine cycle is disrupted); normal urea with elevated ammonia is a warning sign
- Blood ammonia — elevated in encephalopathy
Hepatocyte injury:
- ALT and AST — may be mildly elevated or even normal (in "burned-out" cirrhosis, transaminases paradoxically decline in the final stages)
- LDH — elevated during active hepatocyte necrosis; rises particularly markedly in congestive hepatopathy secondary to heart failure
- GGT and ALP — reflect the cholestatic component
Portal hypertension and complications:
- Platelets — fall with hypersplenism: < 100 × 10⁹/L indicates significant portal hypertension
- Sodium — hyponatraemia (< 130 mmol/L) with severe ascites carries a poor prognosis
A liver function panel is the mandatory starting point for assessment and ongoing monitoring of cirrhosis.
Liver Cirrhosis Treatment: Halting Progression and Managing Complications
Eliminating the cause — the only way to stop progression:
- Alcoholic cirrhosis: complete abstinence — even in decompensated disease, this improves prognosis
- Hepatitis B: nucleoside analogues (tenofovir, entecavir)
- Hepatitis C: direct-acting antivirals (DAAs) — cure in > 95% of cases halts fibrosis progression
- Autoimmune hepatitis: immunosuppressive therapy
Managing complications:
- Ascites: diuretics (spironolactone + furosemide), sodium restriction; for refractory ascites — large-volume paracentesis, transjugular intrahepatic portosystemic shunt (TIPS)
- Variceal haemorrhage: non-selective beta-blockers and nitrates (prophylaxis), endoscopic band ligation (treatment), octreotide (acute episode)
- Hepatic encephalopathy: lactulose (reduces ammonia production in the gut), rifaximin, protein restriction only in severe acute encephalopathy
- SBP: third-generation cephalosporins; albumin infusion to prevent hepatorenal syndrome
Liver transplantation — the only curative option in decompensated cirrhosis. Indications: Child-Pugh class C, MELD score > 15, refractory complications, and hepatocellular carcinoma within the Milan criteria — primary liver cancer that develops against a cirrhotic background in 80–90% of patients. This is precisely why all patients with cirrhosis require ultrasound plus AFP measurement every 6 months: early HCC detection opens the door to transplantation and curative treatment. Post-transplantation 5-year survival: 70–80%.
When to Seek Urgent Medical Attention
- Sudden abdominal distension with dyspnoea — tense ascites requiring urgent paracentesis
- Bloody vomiting or black tarry stools — variceal haemorrhage, life-threatening, call emergency services immediately
- Confusion, disorientation, or inappropriate behaviour — signs of hepatic encephalopathy
- Fever with abdominal pain in a patient with ascites — possible spontaneous bacterial peritonitis
- Sudden drop in urine output in a patient with cirrhosis — possible hepatorenal syndrome
This article is for informational purposes only and does not replace consultation with a gastroenterologist or hepatologist.
Frequently Asked Questions
Established cirrhosis is irreversible — scar tissue cannot be converted back to normal liver tissue. However, eliminating the cause (alcohol cessation, chronic hepatitis treatment) halts progression and stabilises liver function. In decompensated cirrhosis, the only curative option is liver transplantation. In compensated cirrhosis, appropriate management provides normal quality of life and life expectancy.
There is no single specific test. The composite picture includes: reduced albumin and total protein, prolonged PT/INR, elevated bilirubin, low platelets, and abnormal transaminases. The diagnosis is confirmed by liver biopsy or elastography (FibroScan) — a non-invasive method of fibrosis assessment. A liver function panel is the mandatory starting investigation.
Prognosis depends on stage. In compensated cirrhosis (Child-Pugh class A), 10-year survival exceeds 80%. In decompensated cirrhosis (class C) without transplantation, 5-year survival is approximately 20%. Key determinants: cause elimination, complete alcohol abstinence, timely complication management, and access to transplantation.
Absolutely. Even minimal alcohol consumption in established cirrhosis accelerates progression and sharply increases the risk of decompensation. Complete and permanent abstinence is not a recommendation — it is a mandatory condition of treatment. In alcoholic cirrhosis, cessation is the single intervention with proven prognostic benefit even at the decompensation stage.
Ascites is fluid accumulation in the peritoneal cavity. In cirrhosis, it arises through two mechanisms: portal hypertension (elevated pressure forces fluid out of vessels) and falling albumin (reduced oncotic pressure). Treatment: strict sodium restriction (< 2 g/day), diuretics (spironolactone). For tense ascites — therapeutic paracentesis with mandatory albumin infusion to prevent renal failure.
Upload your lab results photo or PDF
AI explains your results in 30 seconds
Choose fileRate the service
Your feedback helps us improve the service