Coronary Artery Disease: Symptoms, Diagnosis and Treatment
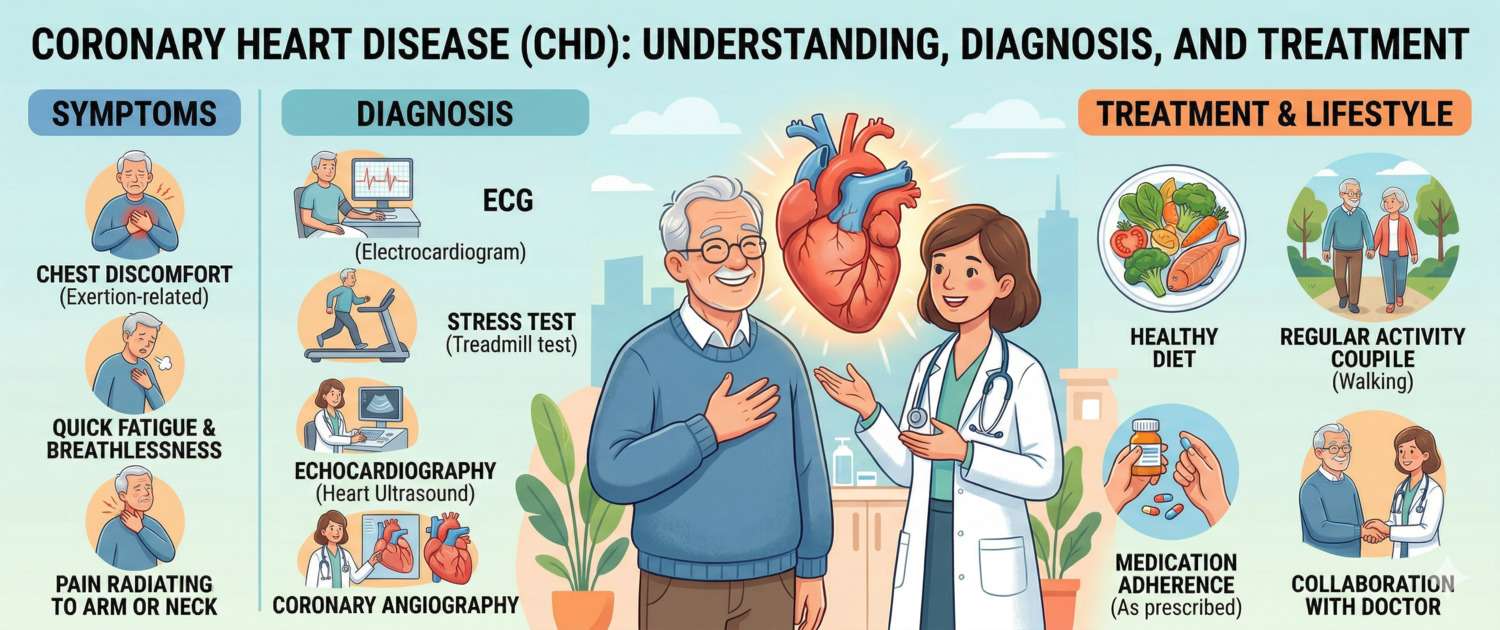
Coronary artery disease is the leading cause of death worldwide. More than 9 million people die from it every year. At the same time, CAD is one of the most preventable and controllable conditions in cardiology. The gap between these two facts has a simple explanation: the disease runs silently for decades, and when symptoms finally appear, a heart attack is often the first sign. This article covers the mechanism, symptoms, diagnostic workup, and modern treatment of CAD.
What Is Coronary Artery Disease
CAD is a clinical syndrome caused by a mismatch between the myocardium's oxygen demand and its actual supply through the coronary arteries. The heart muscle "starves" — and signals this through pain, arrhythmias, or reduced pumping function.
The anatomical basis of CAD in the overwhelming majority of cases is atherosclerosis of the coronary arteries. Cholesterol plaques narrow the arterial lumen, reduce blood flow, and destabilise the vessel wall. Rupture of an unstable plaque with thrombus formation is the mechanism of acute coronary syndrome.
CAD is not a single disease but a group of clinical entities sharing the same pathogenesis. It includes: stable exertional angina — predictable episodes of ischaemia under demand; unstable angina — escalating attacks that precede infarction; myocardial infarction — acute necrosis of a myocardial territory; silent myocardial ischaemia — ischaemia without clinical symptoms, common in diabetic patients; post-infarction cardiosclerosis — scar tissue following a previous infarction; and ischaemic cardiomyopathy — progressive myocardial dysfunction from chronic ischaemia.
Causes and Risk Factors for CAD
The primary cause of CAD is atherosclerotic coronary artery disease. Plaque formation begins in young adulthood and progresses over decades. By the time an artery is narrowed by 50–70% and first symptoms appear, the pathological process is already deeply established.
CAD risk factors fall into non-modifiable and modifiable categories. Non-modifiable: age (risk rises sharply after 45 in men, after 55 in women), male sex (oestrogens protect the vasculature before the menopause), and family history (early CAD in first-degree relatives). Modifiable: dyslipidaemia (high LDL, low HDL), arterial hypertension, smoking, diabetes, obesity, metabolic syndrome, physical inactivity, and chronic inflammation.
The risk of infarction with multiple concurrent factors does not add — it multiplies. A hypertensive patient with high LDL who smokes carries 5–8 times the risk of an age-matched person with none of these factors.
Symptoms of CAD: From Angina to Silent Ischaemia
Typical exertional angina. Crushing, squeezing pressure behind the sternum during physical exertion, cold exposure, or emotional stress. Resolves at rest within 3–5 minutes or after nitroglycerine. Radiation to the left arm, shoulder, or lower jaw is characteristic. For a detailed approach to chest pain symptoms, see the chest pain article.
Atypical CAD. In women, older patients, and diabetic individuals, ischaemia frequently presents differently: breathlessness without pain, unexplained fatigue, back or epigastric discomfort, nausea. Silent infarctions in diabetes are a major reason for late presentation.
Silent ischaemia — ischaemic ECG changes or abnormal stress test without subjective symptoms. Found in 25–30% of CAD patients, particularly in diabetics. Prognostically no less dangerous than symptomatic ischaemia.
Unstable angina — deterioration of stable angina: attacks triggered by less exertion, occurring at rest, lasting longer, and responding poorly to nitroglycerine. This is an acute coronary syndrome — an indication for emergency hospitalisation.
Diagnosing CAD: Blood Tests and Investigations
CAD diagnosis is multi-layered, combining blood tests, functional investigations, and coronary imaging.
Blood tests in CAD. Troponin (I or T) — the key marker for excluding acute infarction in any chest pain syndrome. A normal high-sensitivity troponin at 3 hours from symptom onset virtually rules out infarction. CK-MB — an additional marker of myocardial necrosis; used to estimate the time of infarction onset and quantify its extent.
The lipid panel is the essential investigation for atherosclerotic risk assessment and therapy monitoring. Target LDL in established CAD is below 1.4 mmol/L (very high risk category per ESC guidelines). Statin efficacy is first checked 4–6 weeks after initiating therapy, then every 3–6 months.
Total cholesterol on its own provides limited risk information in established CAD; the full lipid profile with LDL, HDL, and triglycerides is required.
The complete blood count — anaemia as a factor worsening ischaemia: reduced haemoglobin lowers the oxygen-carrying capacity of the blood and increases the metabolic stress on already ischaemic myocardium.
Functional and imaging investigations. Resting ECG — often normal in stable CAD. Stress ECG (bicycle ergometry, treadmill) — reproduces ischaemia; ST-segment depression on exercise confirms the diagnosis. Stress echocardiography and myocardial perfusion scintigraphy are more sensitive. Coronary CT angiography — non-invasive visualisation of the coronary arteries, detecting plaques and quantifying stenosis. Coronary angiography — the gold standard for precise staging and revascularisation planning.
Treatment of CAD: Medications and Procedures
CAD treatment has two distinct goals: relieving symptoms and improving prognosis (reducing the risk of infarction and death). These are addressed by different instruments.
Lifestyle modification — the foundation without which any treatment is incomplete. Smoking cessation (the single most powerful intervention — halves infarction risk), a Mediterranean diet, regular aerobic exercise within the safe exertion threshold, and weight normalisation.
Antiplatelet therapy (aspirin 75–100 mg/day) — lifelong in all patients with established CAD. Prevents thrombus formation on plaque surfaces. In high-risk patients or after stenting — dual antiplatelet therapy (aspirin + clopidogrel or ticagrelor) for 6–12 months.
Statins — mandatory in all forms of CAD regardless of baseline cholesterol. Dual mechanism: they lower LDL and stabilise atherosclerotic plaques, reducing the risk of rupture. Atorvastatin 40–80 mg or rosuvastatin 20–40 mg are standard doses in CAD.
Beta-blockers reduce myocardial oxygen demand, lower heart rate and blood pressure. Particularly indicated when LV systolic function is impaired and after myocardial infarction.
ACE inhibitors / ARBs — reduce afterload, provide cardioprotection. Indicated in CAD combined with hypertension, diabetes, or reduced ejection fraction.
Nitrates — relieve and prevent angina attacks. They do not alter prognosis but meaningfully improve quality of life.
Revascularisation. Percutaneous coronary intervention (PCI, stenting) — restores the lumen of a stenosed artery via balloon catheterisation and stent implantation. The procedure of choice in acute coronary syndromes and significant single-vessel disease. Coronary artery bypass grafting (CABG) — surgical creation of alternative blood supply routes to the myocardium. Preferred for multivessel disease, left main stem disease, or in diabetic patients.
Prevention of CAD: What Actually Works
Primary prevention — stopping CAD from developing in people without established disease. The key tools: blood pressure control (target < 130/80 mmHg), LDL lowering at high calculated risk, smoking cessation, diabetes treatment, regular physical activity.
10-year cardiovascular event risk is calculated using SCORE2 (Europe) or the Framingham risk score (USA) — and the result drives the strategy: observation, pharmacological prevention, or invasive intervention.
Secondary prevention — preventing recurrent events in patients with established CAD. The approach is more aggressive: LDL < 1.4 mmol/L is mandatory; dual antiplatelet therapy follows stenting; cardiac rehabilitation is standard after myocardial infarction.
When to Call Emergency Services
Call emergency services immediately if:
- Crushing or burning central chest pain lasting more than 15–20 minutes that is not relieved by nitroglycerine — acute coronary syndrome until proven otherwise.
- A usual angina attack behaves differently: lasts longer, is triggered by less exertion, or occurs at rest — signs of CAD destabilisation.
- Sudden severe breathlessness, cold sweat, and fear of death alongside chest pain — the classic presentation of infarction.
- Syncope or near-syncope in a patient with known CAD — possible life-threatening arrhythmia on an ischaemic background.
- Any new cardiac symptom in a patient with established CAD — the threshold for seeking medical attention should be very low.
For planned consultation: if a routine check reveals high LDL, arterial hypertension, or an incidental ECG abnormality — see a cardiologist for risk calculation and a decision on preventive therapy.
This article is for informational purposes only and does not replace medical consultation. Result interpretation and diagnosis are made by a qualified physician.
Frequently Asked Questions
CAD is the umbrella term for a group of conditions caused by coronary atherosclerosis. Angina and heart attack are its specific clinical forms. Angina is reversible ischaemia without cell death, triggered by exertion. A heart attack is irreversible necrosis of a myocardial segment due to complete arterial occlusion. CAD is the diagnosis that encompasses both and all related manifestations of impaired coronary blood supply.
The baseline panel in CAD: a lipid panel (LDL, HDL, triglycerides, total cholesterol) — for risk assessment and statin monitoring; troponin — in any chest pain syndrome to exclude infarction; glucose and HbA1c — diabetes doubles cardiovascular risk; complete blood count — to exclude anaemia as an ischaemia-aggravating factor. These form the minimum required at diagnosis and for regular follow-up.
Coronary atherosclerosis is a chronic, irreversible process — existing plaques cannot be fully eliminated. However, modern statin therapy can stabilise plaques, prevent their rupture, and substantially reduce infarction risk. Revascularisation eliminates critical stenoses. Smoking cessation, dietary change, and physical activity demonstrably slow disease progression — some patients achieve sustained remission of symptoms.
The combination of CAD and type 2 diabetes is particularly adverse. Diabetes accelerates atherosclerosis progression, damages the myocardial microvasculature, and blunts pain sensitivity — infarctions in diabetes frequently present without chest pain or with atypical symptoms. LDL target with this combination is below 1.4 mmol/L; blood pressure below 130/80 mmHg; HbA1c below 7%. SGLT-2 inhibitors and GLP-1 receptor agonists reduce cardiovascular risk in diabetes beyond the effect of statins.
CAD in women is systematically underdiagnosed and undertreated. Oestrogens protect the vasculature before the menopause, but after age 55 risk in women rises rapidly and by age 70 matches men's. Women more often have atypical presentations (breathlessness, fatigue rather than pain), contributing to delayed diagnosis. Arterial hypertension and metabolic syndrome carry a proportionally greater cardiovascular risk contribution in women than in men. Treatment is equally effective regardless of sex.
Upload your lab results photo or PDF
AI explains your results in 30 seconds
Choose fileRate the service
Your feedback helps us improve the service